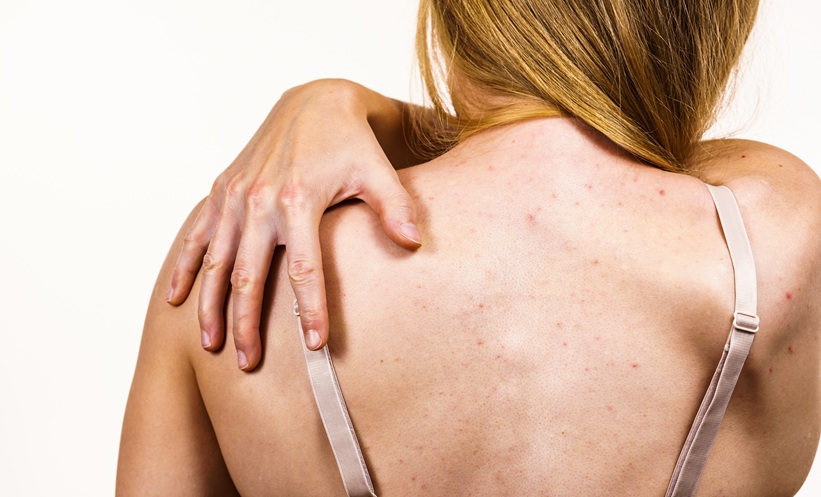
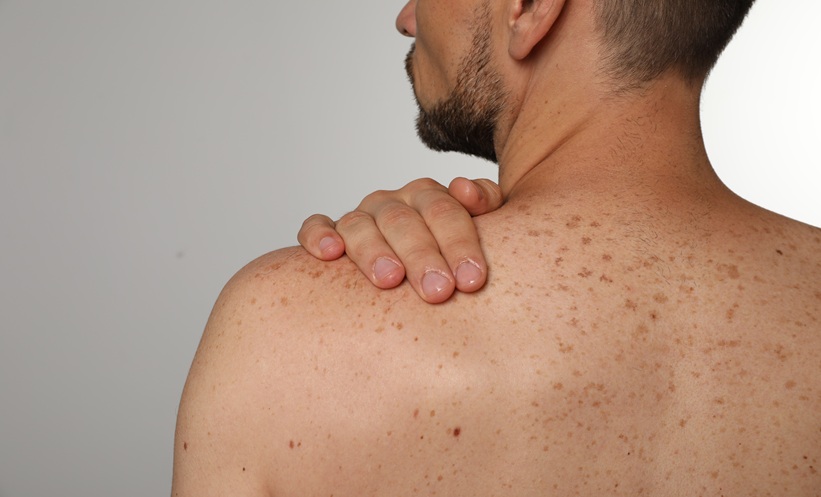
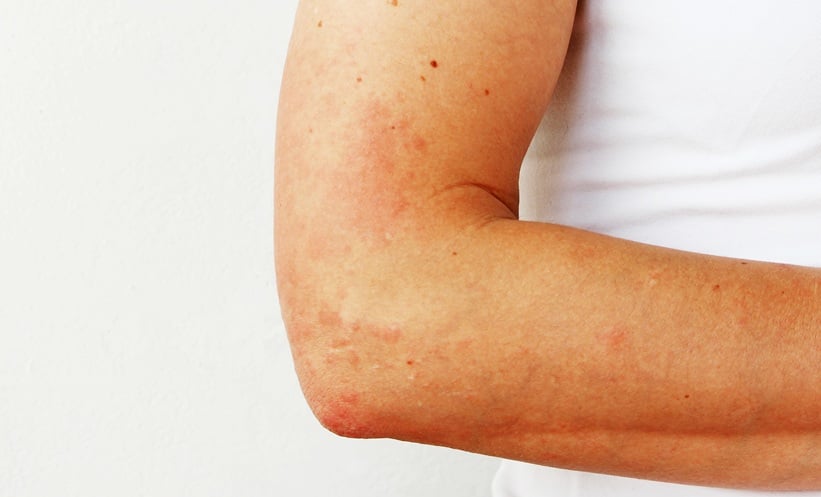
TRUNCAL acne may require more tailored treatment because truncal skin differs structurally and functionally from facial skin.
Truncal Acne Requires a Different Clinical Lens
Truncal acne is common, yet it remains underrecognized in both research and routine practice. In this narrative review, investigators examined how truncal skin differs from facial skin and why those differences matter for acne pathogenesis, treatment selection, and long-term management. Although truncal acne is often approached as if it behaves the same way as facial acne, the review suggests that assumption may overlook important anatomic and physiologic distinctions.
The authors found that truncal skin has a thicker stratum corneum, lower sebaceous gland density and activity, and site-specific variation in pH, sweat gland distribution, and microbiota. Clothing occlusion and friction may further shape the local skin environment. Together, these features appear to contribute to deeper and more extensive lesions, helping explain why truncal acne may present differently and pose distinct therapeutic challenges.
How Truncal Acne can Complicate Treatment
These skin-specific differences may also affect how well treatments perform. The review noted that topical absorption on truncal skin may be more limited, which could reduce efficacy in some cases. Adherence may also suffer, particularly when large surface areas are involved or when formulations are difficult to apply consistently.
Systemic therapies remain an important option, but the authors emphasized that clinicians must balance efficacy with safety when selecting these agents. The review did not frame truncal acne as simply a larger version of facial acne. Instead, it positioned truncal involvement as a clinical setting that may require more deliberate treatment planning, including thoughtful formulation choice and closer assessment of treatment burden.
Routine Skincare may Support Better Outcomes
Beyond pharmacologic therapy, the review highlighted the role of routine skincare in truncal acne management. Appropriate skincare may help reduce adverse effects, improve adherence, and enhance outcomes with topical treatment. This is especially relevant in a condition where tolerability and usability can strongly influence whether patients continue therapy as prescribed.
The authors concluded that clinicians should actively assess truncal involvement rather than focusing only on the face. Management should reflect the biologic and practical realities of truncal skin, with treatment strategies designed to optimize permeability, usability, and patient adherence. Future research will need to better define truncal-specific mechanisms and support development of optimized topical formulations and combination approaches.
Reference
Feng X et al. Truncal Acne: Pathophysiology, Clinical Features, and Management Strategies. J Cosmet Dermatol. 2026;25(2):e70715.
Featured image: Voyagerix on Adobe Stock.