BACKGROUND AND AIMS
Unplanned pregnancy remains a major public health issue worldwide, with well-described associations with delayed antenatal care, adverse maternal psychological outcomes, and increased health-system costs.1-3 Although data from Saudi Arabia show substantial regional variation in prevalence, evidence from the western region, particularly Jeddah, has been limited.4,5 Understanding pregnancy intention and its determinants in local antenatal populations is essential to guide family planning services, postpartum counselling, and pregnancy spacing initiatives aligned with international reproductive health priorities and Saudi Vision 2030.6 The present study was first presented at the International Society of Gynecological Endoscopy (ISGE) Congress 2026.7
MATERIALS AND METHODS
A descriptive cross-sectional study was conducted between September 2022–July 2023 among pregnant women aged 18–50 years attending routine antenatal clinics at King Abdulaziz Medical City (KAMC), Jeddah, Saudi Arabia. Using convenience sampling, 346 participants completed a self-administered electronic questionnaire. Pregnancy intention was measured using a modified Arabic version of the London Measure of Unplanned Pregnancy (LMUP), a validated multidimensional tool categorising pregnancies as planned, hesitant/ambivalent, or unplanned (mistimed or unwanted at conception).8 Descriptive statistics summarised participant characteristics and pregnancy intention. χ2 testing explored bivariate associations, followed by multivariable logistic regression to identify independent determinants of unplanned pregnancy. Statistical significance was set at p<0.05.
RESULTS
The mean participant age was 29.4±5.3 years. Planned pregnancy accounted for 63.0% of participants, while 19.4% reported hesitancy and 17.6% reported an unplanned pregnancy, indicating that more than one-third (37.0%) experienced unintended or ambivalent pregnancy intention (Figure 1).7
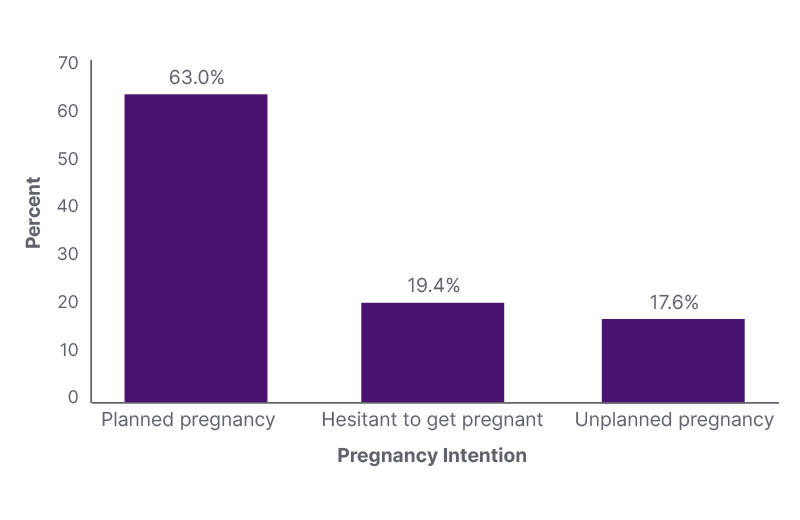
Figure 1: Prevalence of planned, hesitant, and unplanned pregnancies among antenatal clinic attendees at King Abdulaziz Medical City, Jeddah, Saudi Arabia (N=346).
Bivariate analysis showed strong associations between unplanned pregnancy and short interpregnancy interval (<2 years; 47% versus 25%; p<0.001), perceived inappropriate timing (p<0.001), thoughts/actions toward pregnancy termination (p<0.001), and contraceptive-related problems, including incorrect/inconsistent use or side effects (p=0.007), as well as unmet contraceptive needs (p=0.03).
In multivariable modelling, key independent determinants were short interpregnancy interval (<2 years; adjusted odds ratio [AOR]: 2.15; 95% CI: 1.34–3.47), inadequate contraceptive support (AOR: 1.76; 95% CI: 1.11–2.81), and perceived mistiming (AOR: 3.24; 95% CI: 2.05–5.11). In contrast, maternal age, income, and marital status did not show significant associations after adjustment in this cohort.
CONCLUSION
This study demonstrates that unintended or hesitant pregnancy intention remains common among antenatal care attendees in Jeddah. Importantly, reproductive history and contraceptive-related factors were stronger predictors than socio-demographic characteristics, consistent with global and regional evidence indicating that pregnancy spacing, contraceptive access, and method adherence are key determinants of pregnancy intention.9,10
The findings highlight persistent gaps in contraceptive counselling, unmet family planning needs, and challenges related to contraceptive misuse or side effects; factors known to contribute to unintended pregnancy and adverse maternal outcomes.3 Increasing awareness and accessibility of emergency contraception, alongside tailored counselling that aligns reproductive intentions with method choice, may help reduce the burden of unplanned pregnancy. Strengthening postpartum family planning pathways and proactive identification of women at risk due to short birth spacing are also warranted.
These results support ongoing efforts to enhance reproductive health services within Saudi Arabia and align with international commitments to universal access to sexual and reproductive healthcare.6 By targeting modifiable determinants through integrated antenatal and primary care interventions, healthcare systems can better support women’s reproductive autonomy and improve maternal health outcomes in line with Saudi Vision 2030 priorities.







