Interview Summary
Epilepsy affects around 50 million people worldwide. Approximately 30% of them experience drug-resistant epilepsy (DRE), which is defined as the failure to achieve freedom from seizures following two or more standard antiseizure medications (ASM). DRE significantly impacts quality of life (QoL), and increases the risk of complications, including cognitive decline, mental health issues, and sudden unexpected death in epilepsy (SUDEP). The neuromodulation therapy vagus nerve stimulation (VNS) was first approved as a DRE treatment in the 1990s. With the advent of newer ASMs in the intervening years, however, its use has become underutilised in some epilepsy and seizure types, and it is often considered only after multiple ASMs have failed.
In this article, Ana Suller-Marti, Associate Professor of Neurology, Western University, London, Ontario, Canada; James Wheless, Professor and Chief of Paediatric Neurology, University of Tennessee Health Science Center, Memphis, USA; and Steven Wolf, Chief of Paediatric Neurology, Boston Children’s Health Physicians, New York City, New York, USA, discuss the role of VNS in the modern DRE treatment pathway. They outline real-world evidence, presented at the American Epilepsy Society (AES)’s 2024 Annual Meeting, that reaffirms the efficacy of the neuromodulatory therapy, and talk about overcoming barriers to effective management. Earlier intervention with VNS, they argue, could enhance seizure control, decreasing the risk of complications while enhancing QoL.
INTRODUCTION
Epilepsy is a neurological condition characterised by recurrent, unprovoked seizures.1 It affects around 50 million people worldwide and can have a significant impact on morbidity, mortality, and QoL.1,2
Suller-Marti explained that there are more than 30 different subtypes of seizures, falling into the three groups of focal onset, generalised onset, and unknown onset. Focal seizures occur in a localised region of the cerebral cortex, whereas generalised seizures affect both brain hemispheres.3
The ideal goal of treatment, explained Wolf, is freedom from seizures. The first step is clarifying the seizure type or epilepsy syndrome through clinical history and a detailed semiological description of the seizures, as well as brain MRI, EEG, and genetic testing.3 This will inform the choice of ASM, whether that be a sodium channel blocker or a γ-aminobutyric acid agent, for example, he added.3 “You want to match the mechanism of action (MOA) to the seizure type, and then keep adding different or complementary MOAs to achieve maximum seizure control,” he said.
Drug-Resistant Epilepsy
Meeting the goal of seizure freedom, however, is not always possible. “While ASMs aim to control seizures, they do not cure epilepsy,” said Suller-Marti. “Unfortunately, around 30% of individuals with epilepsy do not achieve seizure freedom, even after trying multiple ASMs or combinations of ASMs.”4,5
DRE is defined as the failure of at least two ASMs used at an efficacious daily dose.4 Wolf said: “We know that there’s a significant drop-off in seizure control after drug number two. So, if drug number two fails, the likelihood of a third drug working becomes significantly, exponentially smaller.”4 The impact of DRE can be profound.4-7 “Having repetitive, frequent seizures will affect your intelligence, your ability to focus, your memory, your learning, and your QoL; it stops you from just being able to go out and do things,” Wolf explained.
Suller-Marti explained that DRE was associated with higher rates of depression, social isolation, and suicidality.6,7 Epilepsy is associated with two-to-three-fold more mental health comorbidities (including anxiety and depression) than the general population, and suicide risk is three times higher than in the general population.4 Those figures are higher still among those with DRE.4 “The relationship is bidirectional: the seizures negatively impact QoL and contribute to social isolation, which in turn exacerbates the mental health challenge. In addition, some ASMs may also adversely affect mood and emotional wellbeing,” explained Suller-Marti.
One of the most severe potential outcomes of uncontrolled seizures is death. “This may occur through various mechanisms, including drowning accidents, bleeding, or falls. Another major entity is SUDEP, a phenomenon where an individual dies after a seizure, suddenly and unexpectedly,” Suller-Marti added.
The incidence of SUDEP increases in line with disease severity. One study showed it to be 1.2 per 1,000 person years in the general epilepsy population, compared to 4.2 in those with DRE. In individuals evaluated for epilepsy surgery, the incidence was 6.2 per 1,000 person years.7 “Patients with DRE require close follow-up. Neurologists and epileptologists must act proactively, including referring patients to specialised epilepsy centres and arranging for surgical evaluation and epilepsy monitoring,” said Suller-Marti. “You need to explore further treatment options without unnecessary delays.”
Resective epilepsy surgery, which removes the area of the brain from which the seizures originate, remains the most successful strategy for achieving seizure freedom, and can be successful in up to 80% of cases in selected patients.4 However, only a subset of patients, i.e., those with focal onset epilepsy in whom the epileptogenic zone can be clearly identified and does not overlap the eloquent cortex, “are lucky enough to be eligible for epilepsy surgery,” explained Suller-Marti.4,8 “Those with generalised epilepsy, where the seizure involves both hemispheres simultaneously, are not candidates for resective surgery.”
VAGUS NERVE STIMULATION
VNS is an adjunctive neuromodulatory therapy that can be efficacious in reducing the frequency and severity of seizures in people with DRE.6 The long-established non-pharmacological intervention involves a small pulse generator being surgically implanted under the skin of the chest and connected to the left vagus nerve via a lead wire. The generator transmits electrical signals to the vagus nerve. Suller-Marti said: “VNS has the potential to reduce seizure frequency and severity, prolong seizure-free intervals, and reduce the risk of SUDEP, thereby addressing critical unmet needs in this high-risk population.”
VNS was approved in people with focal and generalised onset seizures of all ages in Europe in 1994. In 1997, the USA approved it for use in focal onset seizures (FOS) in people over the age of 12 years, though the label has since been updated to include those with FOS aged 4 years and above.6
However, many new epilepsy drugs have become available over the last 30 years, and as of 2022, more than 40 ASMs were available.9,10 This raises the question, said Wheless, of the intervention’s place in today’s DRE treatment pathway. During the AES 2024 Annual Meeting, held in Los Angeles, California, USA, in December, researchers presented a number of studies that provide a picture of the current use of responsive VNS in the real world.
DRUG-RESISTANT EPILEPSY AND FOCAL ONSET SEIZURES
FOS are the most common seizure type in both children and adults.11 “They are important not just because of the numbers, but because we do not have one single treatment that will control all FOS in every patient,” said Wheless.
FOS are not what people typically picture when they think of an epileptic seizure, he went on. “If I had focal seizures, for example, I may just stare off, maybe have some lip smacking; I’m not fully aware. I may follow you with my eyes if you were to walk in front of me, but I can’t talk to you; I can’t respond. That lasts a minute or so, and I will be tired or really groggy for 5 or 10 minutes afterwards, and still not 100% myself for hours.” This will stop people from taking part in daily activities, whether that is going to work, going to school, or socialising, he said.
While the ideal is to achieve to seizure-free status, Wheless said that there are many people who, “even with all of our best therapies”, do not reach this treatment goal. He highlighted that DRE does not necessarily mean that ASMs do not work at all. “Instead of having maybe seven seizures a month, they maybe have two. That is still not seizure freedom, which is where we would like them to be,” he said. “It is still interfering with their QoL and keeping them from doing things they want to do.” In these patients, it is important to minimise seizures and improve QoL, he said.
VAGUS NERVE STIMULATION IN CHILDREN WITH FOCAL ONSET SEIZURES: REAL-WORLD EVIDENCE
Wheless was part of a group that evaluated VNS therapy after 24 months of use in children aged 4–12 years with DRE and FOS. Presented at AES 2024, the subgroup analysis of the prospective, multicentre, multinational observational CORE-VNS study included 150 children with DRE and FOS who were VNS naïve at baseline.12
At 24 months, the responder rate, defined as a ≥50% reduction in FOS frequency over the previous 3 months compared to baseline, was 59.2%. Approximately 40% had a >80% seizure response, and 22% were seizure-free, over the previous 3 months (Figure 1). The median seizure frequency reduction at 24 months was 64% for focal seizures. The analysis also found QoL improvements in more than half of participants, with only 31.4% reporting no change, and that responsiveness to VNS continued to increase over time.12
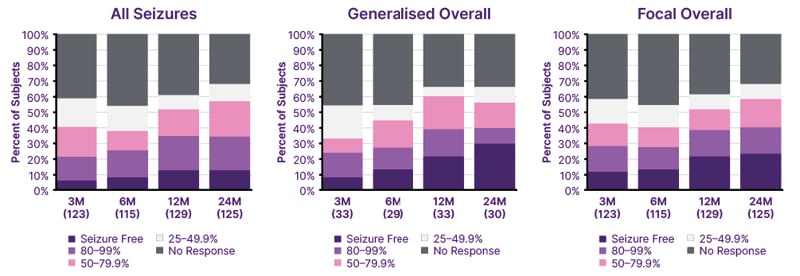
Figure 1: Seizure frequency reduction (implant naïve to 24 months) percent of subjects reporting.12
M: months.
Despite VNS being indicated after the failure of at least two ASMs, a median of six (range: 2–17) had been tried in this group. The median age at first implant was 10.4 years (range: 4.05–17.99), with a median duration between diagnosis and informed consent of 6.5 years.12 Highlighting these figures, Wheless said that early intervention was crucial, particularly in children. There should, he said, be a “sense of urgency” around controlling seizures, minimising medication side effects, and enhancing QoL. “Often, seizures are allowed because they are not convulsive. People think, ‘the child stares off, they recover, and they do fine afterwards’. Yet we know if that goes on for long periods, abnormal connections are set up in the brain. Then when we try to pursue other therapies down the road, they are not as effective as they would have been if we had used them earlier.” The potential impact on development must also be considered, he went on. “We know there are critical developmental time windows,” he said. “Children are supposed to do things a certain time, and if their seizures (or treatment side effects) interfere with that progress, we can’t just go back when they’re older and fix it.”
The other key point, he went on, was the side effect profile, which he described as “mild.” Around a quarter (24.7%) of children reported at least one treatment-emergent adverse event. The most common were cough (5.3%), dysphonia (7.3%), and other respiratory, thoracic, and mediastinal events (10.7%).12 “I think we sometimes forget that, compared to a lot of other treatments, VNS is very well tolerated.”
Over the last 30 years, he added, clinicians have learned how best to use the device in a way that minimises both side effects and seizures. “It is unique to have that longevity of data… and it tells us that, if our patient responds to this treatment, […] they are likely to continue to respond over time.”
Reflecting on his own practice, he added that there were various other benefits to VNS in this group. It is not a medicine, meaning that drug–drug interactions are less of a concern, and it is an “automatic treatment” that “works in the background.” “It is one less thing the families and the children have to think about every day. It is like having the thermostat set on your heating at home; it’s just working away.” VNS can contribute to the lowering of ASMs, thereby reducing side effects, and also have a positive impact on mood, he said. This is important as children grow into adolescence and adulthood, when FOS become closely associated with mental health issues.
The CORE-VNS sub-analysis data “reaffirm the efficacy of VNS,” said Wheless. “I think it will make clinicians rethink where they place it in the treatment list. We shouldn’t be waiting until after the sixth or seventh medicine. We should be thinking about this early on because the data supports it.”
DRUG-RESISTANT EPILEPSY AND GENERALISED TONIC-CLONIC SEIZURES
Generalised tonic-clonic (GTC) seizures are one the most common type of generalised seizure, and are associated with loss of consciousness.13 They begin with a tonic phase, where the body becomes very stiff, followed by a clonic phase, which is characterised by rhythmic jerking movements.13 GTC seizures may involve hypoxia,14 and “immediate assistance is usually needed,” said Suller-Marti.
Ongoing seizures can have a wide range of consequences,4-7 she went on. “Seizures can be frequent and unpredictable, significantly limiting daily activities, independence, employment, and overall QoL. Unfortunately, many patients are unable to maintain employment due to the frequency and severity of the seizures, and are not permitted to hold a driving license. In many countries, this severely limits their ability to participate in society, including working, attending school, or even living independently.” Memory complaints are common and can be associated with the administration of multiple ASMs.15 “While seizure control is currently the most effective strategy to improve memory, this remains particularly difficult in cases of DRE,” said Suller-Marti.
For all these reasons, individuals with epilepsy, especially those with DRE, require comprehensive and multidisciplinary care. “This will include psychological support and neuropsychological evaluation to assess cognitive function and develop tailored strategies to enhance memory and cognitive performance,” Suller-Marti explained. “Social support is also essential to ensure access to appropriate treatment and medication. Education plays a critical role in empowering patients, helping individuals better understand their condition and navigate the diagnosis and treatment.”
VAGUS NERVE STIMULATION IN GENERALISED TONIC-CLONIC SEIZURES: REAL-WORLD EVIDENCE
In the USA, VNS is only approved for use in focal seizures. However, it is licenced for GTC in Europe.6 Suller-Marti’s team’s sub-analysis of CORE-VNS data, also presented at AES 2024, sought to add to the evidence base for the device’s use in this indication, she explained.
A total of 59 participants met the criteria of a diagnosis of primary GTC and receiving VNS for the first time. Twelve were implanted within 5 years of diagnosis, while 47 started VNS therapy ≥5 years after. Those who were implanted earlier tended to be younger (9.7 versus 25.9 years), and participants had tried a median of six (range: 2–20) ASMs before starting VNS therapy.16
Thirty-six-month follow-up data was available on 40 of these patients. It showed a responder rate of 70%, and a median seizure frequency change of –83.2% (Figure 2). This was regardless of the time between diagnosis and implantation. “Even though this is not seizure freedom, it is a big change in their lives,” said Suller-Marti. Those with earlier implantation were more likely to be responders at 36 months (83.3% versus 67.7%) and have a higher median seizure frequency change (–94.3% versus –76.4%).16
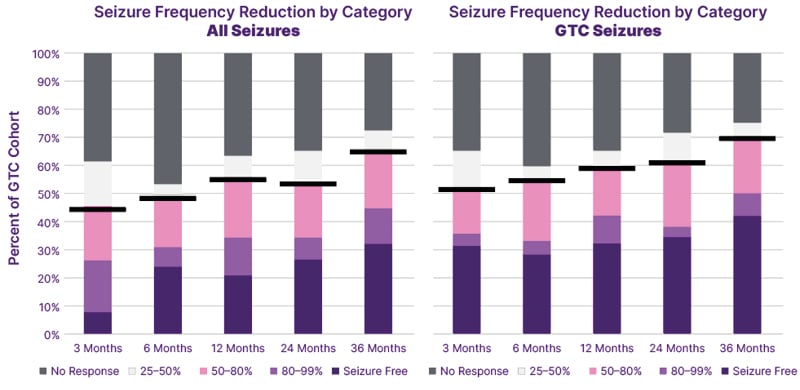
Figure 2: Seizure frequency reduction by category.16
GTC: generalised tonic-clonic.
There was also, Suller-Marti went on, a “notable reduction” in healthcare utilisation. At baseline, there were a total of 24 emergency department visits and 19 hospitalisations in the previous 12 months. At 36 months, each of these metrics had dropped to four.16 “The patients included in this study suffered from highly refractory epilepsy and uncontrolled seizures,” she highlighted. “This reduction indicates an improvement in their QoL, as each visit adds stress, which negatively impacts their and their family’s mental health.” It also reduces societal healthcare costs overall, she added. In addition, patients reported a decrease in their perceived severity of epilepsy,16 Suller-Mari went on. “It is all pointing in the same direction: that everything is better overall.”
The most frequent treatment-emergent adverse events were dysphonia (11.9%; n=7), dyspnoea (6.8%; n=4), and implant site pain (5.1%; n=3).16 “It was, overall, well tolerated, and there were no major or severe side effects that we did not expect.” It is important to remember, she went on, that many of the side effects can be easily managed with “proper parameter adjustments.”
The sub-analysis also looked at the proportion of patients reaching the target dose range. Suller-Marti explained that, while the device’s manufacturer recommends an output current of 1.625 mA as the therapeutic dose, this can vary in clinical practice according to the patient’s tolerability and even physician preference. At 12 months, 60% of patients were in the therapeutic range, and this rose to 70% at Month 24.16 “It is possible that this was associated with some of the positive results,” she said. It is important to remember, however, that some patients respond at a lower dose. “It must be adjusted based on the patient’s tolerability,” she added.
The results show that “there are treatment options beyond medications for these often-overlooked populations,” Suller-Marti explained, calling VNS “an excellent option.” “While we may not achieve complete seizure freedom, the level of seizure reduction observed is so significant that it dramatically improves patients’ lives and lowers their risk of SUDEP.”
EPILEPSY RESCUE MEDICATIONS
Rescue medications are an important tool in epilepsy management. They can abort prolonged seizures with the potential to evolve into status epilepticus, as well as prevent subsequent repeat, or cluster seizures, explained Wolf.17 “We know that there is a subset of patients who, if they have one seizure, are going to have another one in the next 24 hours. If you can interrupt that with a rescue medication, that will drop the likelihood of a subsequent seizure and allow them to get on with their day.”17,18
Common rescue medications include benzodiazepine tablets, rectal solutions, and intranasal sprays.17 There are challenges with these traditional approaches, however, said Wolf. He explained that tablets have a slow onset, rectally administered formulations come with social issues, and all can have sedative effects. VNS has become something of a rescue treatment in recent years, Wolf said, explaining that a magnet stimulus can be passed over the device to temporarily increase the dose.19 “Some people can feel an aura coming on. They want to be proactive, but they know a pill will take half an hour; swiping the magnet allows for rapid treatment,” Wolf explained. “Then you have the patient who is having 30 seizures a day. There’s no way you can give that many benzodiazepine-type medications; they become too sleepy. The family finds it really beneficial to have the VNS magnet as a rescue treatment.”
He also explained that clinicians often use the frequency of rescue medication use as a marker of disease activity and control.19 “If someone is using a lot of rescue medications, whatever I am doing as the baseline, daily preventative treatment is not enough. If they needed no rescue medications, and only had one small seizure, then maybe their treatment just needs a small tweak.” No seizures and no rescue medications are an indication that the current treatment plan is working, he said.
VAGUS NERVE STIMULATION AND RESCUE MEDICATIONS: REAL-WORLD EVIDENCE
In recent years, Wolf said he had seen an increase in the number of ASMs people living with epilepsy have tried before VNS implantation. “Over the years, as more and more new ASMs have come on the market, people keep going after medication number two or three,” he said. “By the time they came to our specialist epilepsy practice, they had been on seven or eight medications.” In the clinic, though, his team was noticing a reduction in rescue medication and, in some cases, ASM use, following VNS implantation.
To validate this, they analysed data from the Seizure Tracker® app (Seizure Tracker LLC, Springfield, Virginia, USA), which enables patients and their families to record seizures and rescue medication use in a diary. Wolf explained: “We wanted to try to make the point of ‘why are you waiting so long to introduce neurostimulation?’” Wolf’s team has been encouraging families to use the app for some time, and it has become a “trove of information,” he added.
The study, presented at AES 2024, included 95 patients. It evaluated trends in rescue administration frequency before and after the first recorded VNS magnet swipe in patients with DRE who had recorded at least one VNS magnet swipe or benzodiazepine rescue medication usage within the 90 days prior to the first swipe. At baseline, the mean seizure frequency reduction rate was 8.3 per month, with a median rescue medication use frequency of 2.1 administrations per month (SD: 3.3).Significant reductions in rescue medication usage were observed at 91–180 days post first VNS magnet swipe (median: 0.33 [quartile 1 (Q1)–quartile 3 (Q3): 0.00–2.30]; p=0.046), 181–360 days (median: 0.33 [Q1–Q3: 0.00–1.83]; p=0.009), 361–540 days (median: 0.17 [Q1–Q3: 0.00–0.83]; p<0.001), and at 541–720 days (median: 0.00 [Q1–Q3: 0.00–0.42]; p<0.001). Wolf highlighted that the magnitude of reduction increased over time (Figure 3).19
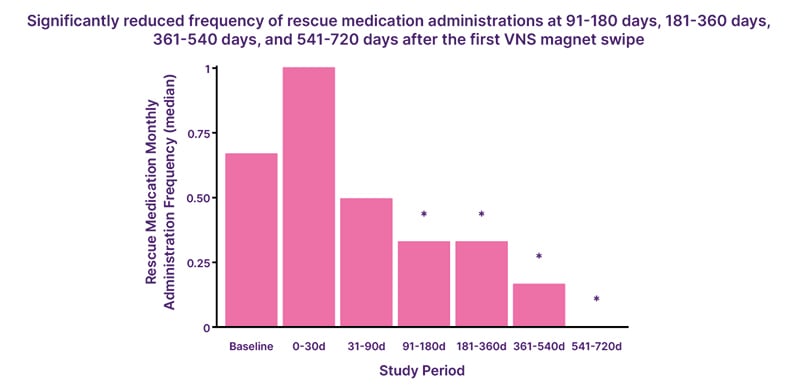
Figure 3: Use of rescue medication at 91–180 days, 181–360 days, 361–540 days, and 541–720 days after first vagus nerve stimulation magnet swipe.19
*statistical significance at the 0.05 level
d: days; VNS: vagus nerve stimulation.
“The decreased use of rescue medications tells you a lot about how the patient is doing,” he said. “If you are not using the rescue medications as often, your brain is less exposed to benzodiazepines, which can slow you down and make you sleepy. That is a real plus.” It is a fair assumption, he added, that fewer seizures translate to “patients feeling better and having a lower risk of SUDEP.” “If the risk of your day being interrupted, your memory being wiped out, or missing a birthday party or going out for dinner is lower, then your QoL has got to be better,” he added.
What is important about these data, Wolf went on, is that they are “real numbers” from a “real, honest collective group” over 20 years. “It is a regimented group who are making sure they, their children, or their loved ones are taking their medication,” he said. “Patient perspectives are extremely valuable and we have to listen to them. I do not think this is the singular, perfect study; I think it is complementary to and validates the other studies that have shown the benefits… You need multiple sources of information to decide whether something is reliable.”
VAGUS NERVE STIMULATION IN TODAY’S DRUG-RESISTANT EPILEPSY LANDSCAPE
The results of these three studies demonstrate the role of VNS in today’s rapidly expanding treatment landscape, said the clinicians.
“I think our paper helps to bring back the conversation of VNS,” said Wolf. “When a treatment is more than 30 years old, people can forget about it. When the new drug with a fancy MOA comes along, they can forget about the true, tried, and tested approaches.” Clinicians may well remember those people who did not respond to VNS, but not those who “still have it in, and are doing really well,” because “they are barely in your office,” he added.
Unfortunately, said Wheless “we are still trying too many medicines before we get to the other options.” “We have a lot of faith in our modern medicines, and I think we delay because we think ‘we have all these good medicines, surely one of them will work’.” Wheless also noted that, as a non-pharmacological therapy, VNS can be used in combination with any ASM, without concerns around drug–drug interactions. That means new drugs can be added as and when they become available and/or indicated, or reduced or withdrawn if they are poorly tolerated. “We know that if a patient responds to VNS, they are going to continue to respond over time. It can be part of their foundation therapy,” he said.
Both Wolf and Wheless acknowledged that it is often easier to write a prescription than to refer a patient for neuromodulation. That does not, however, make it the right approach, they added. One potential barrier is patient or family reluctance, though this is often based on the misconception that VNS involves brain surgery. Open and honest conversations are vital, they agreed.
Wolf said: “You need to think about at which number of medications you should start the conversation. That does not necessarily mean you pull the trigger, but you talk about neuromodulation as a possible option.” At his centre, they start this process of outlining the pros and cons of VNS at the failure of two ASMs. “We tell them that there are three groups of patients,” he went on. “In one group, it does not do anything… We have a group that has a huge seizure reduction, and when they use the magnet, it stops the seizures… Then we have the group [which] has maybe a 50% to 60% reduction in seizures, but when they use the magnet, it aborts the seizure or prevents seizures going forwards.” It “might not be perfect” in that middle bracket, but it is “certainly better” than what they are used to, and may allow for the reduction of ASMs and their associated side effects, he added.
Explaining how the device works and the process of implantation should form part of those initial conversations. Wheless said: “We tell families that even though it’s ‘surgery’, it is not what they are typically thinking of. It is not permanently removing anything… and it is totally reversible. Worse case scenario, it does not work and we take it out.”
One challenge when talking to patients and their families is the pure number of options available, Wheless added. “I think it helps to tell families that VNS is a reasonable option, and that we should not wait 2 or 5 years or until they have had multiple medications before we do it. If we are going to do it, it will be better to do it at the front end, when you will get the most benefit,” he said.
CONCLUSION
Real-world evidence presented at AES 2024 complements the decades of existing data that demonstrate VNS’s efficacy in reducing seizure frequency and improving patient outcomes.
It also shows that VNS is often underutilised, with many patients being subjected to prolonged trials of multiple ASMs before neuromodulation is considered. This delay may limit the potential benefits of VNS, particularly for paediatric patients in whom earlier seizure control could mitigate developmental delays and cognitive impairments.
Moving forward, greater awareness and proactive consideration of VNS earlier on in the treatment pathway could improve outcomes for many people living with DRE.