Interview Summary
Acne vulgaris (AV) is one of the most common inflammatory dermatological conditions affecting mainly adolescents, female adults, and individuals with underlying conditions such as polycystic ovary syndrome (PCOS). EMJ spoke to three dermatology experts who discussed how the impacts of acne go beyond the skin and can undermine selfesteem and lead to stigmatisation. Treatment guidelines recommend combination therapy addressing all four pillars of acne pathophysiology: increased sebaceous gland activity, inflammation, hyperkeratinisation, and Cutibacterium acnes (C. acnes) proliferation. Until recently only systemic treatments have existed to reduce sebum production. Increased sebum production starts during adrenarche and accelerates during puberty in response to hormonal changes. In people with acne, an over-production of sebum correlates with disease severity. The experts highlighted how clascoterone, a first-in-class topical androgen receptor inhibitor, has the potential to meaningfully broaden treatment options for acne. Now available for clinical use in the USA, EU, and UK, clascoterone directly targets androgen mediated sebum production and inflammatory processes that occur in acne. It offers a well-tolerated and efficacious treatment, compared to placebo, for patients with AV of all genders aged 12 years and upwards (only for facial AV in 12–18-year-olds in the EU), and can be used as a monotherapy and in combination with other topical and systemic agents. The experts discussed example cases and indicated that early control of sebum production, which is integral to developing acne, may help prevent scarring and hyperpigmentation, and so help to reduce the psychological sequelae of AV.INTRODUCTION
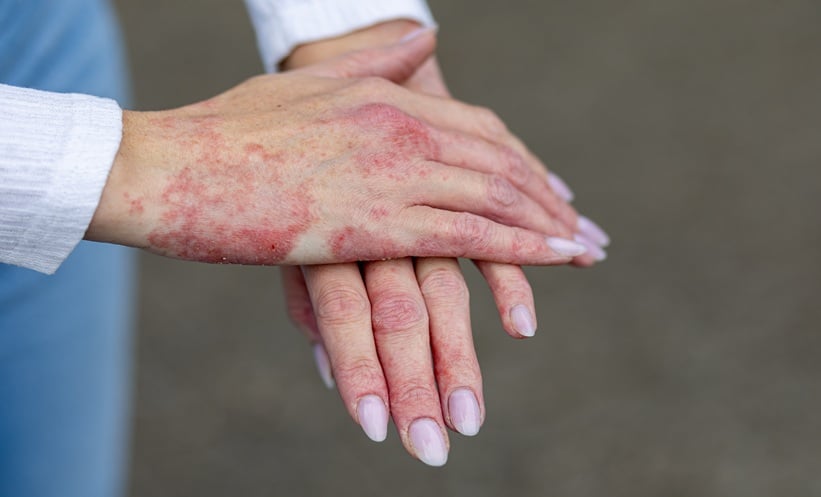
Acne Vulgaris (AV) is a common and often chronic skin disorder that affects most people at some point in their lives, regardless of gender, ethnicity, or skin tone.1 The clinical presentation is most prevalent in adolescents, but latest prevalence data suggest acne is starting earlier and lasting longer,2 particularly in adult women (>25 years old), with prevalence ranging from 12–54%.3
Most referrals to specialist dermatology clinics stem from physical AV affecting the face, but the condition can affect the chest, back, and neck, and as the condition progresses, the risk of permanent scarring increases.4 The impacts of AV go beyond the skin, with psychological sequelae adding to the burden, including low self-esteem, lack of self-confidence, and relationship problems.5 Stigmatisation and discrimination can also result.5,6
AV is underpinned by four pathophysiological pillars: excess sebum production and change in the constituents of sebum, follicular hyperkeratinisation, colonisation and proliferation of C. acnes, and inflammation.7,8 The sebum comprises fatty acids, squalene, cholesterol, and other components that also play important roles in skin hydration and antimicrobial defence.8 However, overproduction of sebum contributes to bacterial proliferation with concomitant inflammation, which together exacerbate AV.9 Androgens are known to play a crucial role in the regulation of sebaceous gland activity and sebum production,10 and the androgen-mediated increase in sebum production is implicated as a necessary early step inAV pathophysiology.10
Medications to treat mild-to-moderate AV include topical therapies such as retinoids, benzoyl peroxide, and antibiotics.1 For more severe AV, oral isotretinoin is recommended as an alternative. Off-licence use of spironolactone and oral contraceptives are options for female patients, but not males.1 Treatment guidelines recommend combination treatments that target all aspects of acne pathogenesis.11,12 However, until now, topical treatments that target androgen-mediated sebum production that could be used in both males and females have been lacking.10 Clascoterone is a recently licenced topical androgen receptor inhibitor that is effective and well-tolerated in both males and females.11-17 It is licenced for clinical use in the USA and Europe.18
EMJ spoke to three specialist dermatologists, Hilary Baldwin, Medical Director, Acne Treatment and Research Center, New York, USA; Pedro Herranz, Vice President of the AEDV Central Region, Hospital Universitario La Paz, Madrid, Spain; and Alison Layton, Consultant Dermatologist, Harrogate and District NHS Foundation Trust, UK, to find out how clascoterone is changing the treatment landscape for acne and to explore how it is impacting (or will impact) clinical practice, highlighting case examples.
THE CHALLENGES OF ACNE VULGARIS THAT GO BEYONDTHE SKIN
Acne presents significant physical and psychological challenges for patients.4-6 The majority of adolescents, both male and female, will experience the condition, whether mild, moderate, or severe, between the ages of 12–25 years.2 “Many of the adolescents we see in clinic have already spent significant amounts of money on over-the-counter medications before they are referred,” Layton explained. This reflects Herranz’s experience, who sees patients in private clinics and hospital settings. Although access to dermatologist expertise is relatively easy in Spain, they said, “Adolescents prefer to follow advice from their friends, family, or social media, and often they think they are using an active therapy when they are not.” Baldwin runs a tertiary referral clinic in the USA. The patients they see in clinic are evenly split between adolescents with moderate-to-severe acne and adult women, who are often experiencing acne for the first time in their 30s or 40s. Layton’s super-regional acne clinic also provides services for a range of patients, including those with endocrinopathies such as PCOS and late-onset congenital adrenal hyperplasia.
The experts agreed that, although most patients are concerned about their appearance and primarily want clear skin, it is the potential for scarring, both physical and psychological, that concerns their physicians. “We see many patients who haven’t responded to previous treatments or had delayed treatment and who are starting to scar,” Layton explained. Herranz added that it is critical to provide information to explain the importance of using medical therapies to help prevent scarring.
Acne can have a significant impact on health-related quality of life.4-6,19 “Your teenage years are when your sense of self is developing. Peer pressure is huge, and acceptance is enormous, so having acne is a real detriment during the teenage years,” Baldwin emphasised. In addition, there is evidence that people with acne and acne scarring are perceived differently.5,6 “Stigmatisation is a real issue,” added Layton, and this can be the case for both adolescent and adult patients.
Baldwin agreed, saying: “We are seeing more and more adult female acne patients, and they are suffering too, in different ways than adolescents; adolescents with acne may not look out of place, but for an adult female, they may be the only one with acne in their friendship circle, or in the work-place. It can cause discrimination and, at the least, impact self-confidence and potentially affect their ability to do a good job.”
Herranz emphasised the importance of having open and honest conversations with patients about their treatment options. “I am very frank with patients, explaining how the medication will work and to make them feel comfortable about the therapy.” Herranz went on to say that often the hardest patients to treat are those who have mild flares but never achieve clear skin. “These patients can suffer a lot. No one is offering them a true solution, and they may have acne for 6–7 years, developing anxiety and low self-esteem: psychological scars that can last a lifetime.”
“Education is very important,” Layton agreed. It helps to reduce the chances that patients will progress to severe disease with potential for scarring or hyperpigmentation, and the psychological impacts those sequelae can bring. “I discuss with the patient how different treatments work in relation to acne pathophysiology and why a combination therapy might be necessary.”
SEBUM PRODUCTIONAND THE PATHOGENESIS OF ACNE VULGARIS
Baldwin, Herranz, and Layton emphasised that sebum production is integral to the pathogenesis of AV. Longitudinal studies in children show that an increase in sebum is linked to acne development even before puberty, as they enter the adrenarche.9 Layton was succinct, saying, “no sebum, no acne,” and went on to explain that sebum contributes to acne development in a number of ways. “It’s not just the amount of sebum, but the constituents,” Layton said. “Within the follicles, different components can become oxidised and induce inflammatory cytokines, resulting in comedones.” The sebum also promotes C. acnes growth.20 There is evidence, Layton added, that “sebum production correlates with the severity of disease.” 1
Despite the importance of sebum in AV pathophysiology, few medications to date have targeted sebum production. “We’ve been talking about retinoids for hyperkeratinisation and antibiotics to kill C. acnes, and we’ve talked a lot about acne being an inflammatory disorder,” elaborated Baldwin, “But for sebum inhibition, we only had oral isotretinoin for severe acne and off-label spironolactone and birth control pills that could only be used in females.” Yet, Baldwin added, “Sebum is a foundational problem for everyone with acne. When androgens are produced, they stimulate the sebaceous glands, and everything happens downstream from there.” In addition, sebum plays a secondary role as part of the ongoing cycle of acne, inflammation, hyperkeratinisation, and C. acnes infection. Baldwin went on to point out that “people born with androgen insensitivity syndrome, where their end organs don’t recognise that androgen’s being produced, have many issues, but the one thing they don’t have is acne.21 The bottom line is: no androgens, no sebum. No sebum, no acne.” Herranz agreed, saying: “Sebum production is the orphan part of acne, and it is difficult to control.”
TAILORING TREATMENT PLANSTO INDIVIDUAL PATIENTS WITH ACNE VULGARIS
Baldwin, Herranz, and Layton explained that, in their experience, acne presents in a myriad of ways, and patients vary in their attitudes to the disease, so individualised treatment plans are an important part of successful treatment. Baldwin explained that it is important to first assess the type of lesion the patient has and whether it is mostly comedonal or inflammatory, or a combination of both, and whether the trunk is involved or if it is only facial acne.
“I then ask them, ‘on a scale of one to 10, how much do you hate your acne?’” Baldwin continued. The answer to this question helps the expert assess the impact of acne on the patient’s quality of life and how likely they are to adhere to multiple treatments. Herranz and Baldwin agree that some adolescents just aren’t ready for treatment and sometimes their parents bring them into the clinic under duress. Baldwin added: “We have a conversation about their lifestyle, whether they think they will have time to apply medication and whether they have hobbies, like playing sport that involves wearing goggles, or helmets that may exacerbate acne, or reduce their ability to use medication.” Layton agreed, adding: ‘If the disease is extensive, it may not be practical to use topicals. Or if it extends to the trunk, it may not be practical to use benzoyl peroxide, which candiscolour clothing.”22
A patient’s age is also relevant. “Weknow that if we use isotretinoin in young patients, they are going to relapse, probably within 3 years,” said Layton. “Having a medication that could potentially stop relapse by keeping sebum levels down would be very useful,” they added. “We also need to consider the use of effective treatments to reduce the chance ofscarring and hyperpigmentation.”
In skin Types III–VI,23 acne pimples and pustules can develop into hyperpigmented spots, rather than clearing completely. This is due to post-inflammatory changes and melanin overproduction.24 According to Baldwin, the dark spots can last for 6–12 months and are a common feature of severe acne in people with darker skin tones, and irritants, including topical retinoids, can exacerbate the hyperpigmentation process. “For a person with skin type V or VI, every pimple has the potential to create a dark spot, so I want to make their acne better as quickly as possible.” Baldwin emphasised. Approximately 60% of Baldwin’s patients have skin Types IV–VI. “In these cases, we take a different treatment approach compared to someone with a light skin tone.” Baldwin explained. “I need to ensure they are not aggressively cleansing their skin and that they use quality moisturisers. I also recommend patients avoid products like shea butter and cocoa butter, which can be comedogenic,” they added.
“It’s important to have a conversation with the patient about how and when they might use the medications. We agree on a plan, and I write it down for them, so they understand how the treatments work and how they can use them practically in everyday life,” Layton added.
GAPS IN THE ACNE VULGARIS TREATMENT LANDSCAPE
Guidelines from the USA11 and UK12 recommend combination therapy to treat acne, addressing all four factors of acne pathophysiology for maximum efficacy. However, until recently, there has been a lack of treatments that effectively target androgen-mediated sebum production.15,25
Layton explained that in the UK, guidelines recommend fixed combination topical medications initially, coupled with a good skincare regime.12 “If the disease is moderate-to-severe, we add in an oral antibiotic. Second-generation tetracyclines are recommended [in the UK].” Layton added that, for some patients, fixed combination treatments are not well tolerated, and salicylic acid is used. “If the patient has significant acne and has not responded to combination therapy and there is a risk of scarring, we would consider oral isotretinoin.”12 This is the only oral medication to reduce sebum that is available for females and males.12 In the UK, oral isotretinoin is only available for those with severe acne. “This means if we see a male who hasn’t responded to fixed combination therapy plus an oral antibiotic, and their acne is not severe enough to merit oral isotretinoin or there are contraindications to using oral isotretinoin, until now we have had no other options to reduce their sebum,” Layton explained.
Clascoterone is available for clinical use in the USA, EU, and UK, and both Baldwin and Layton are now prescribing it for patients. At the time of speaking to Herranz, it had yet to be licensed in Spain; however, Herranz believes it may be a promising option for some people with acne. “It’s a topical treatment with a novel mechanism of action. I think most of my patients would benefit from it.”
In Spain, Herranz added, “The problem we have is that patients can see some improvements with currently available medicines, but they are still experiencing flares. We need to be aggressive with therapy to clear the skin, because if they are still having flares, they will quit the therapy.” Herranz offers patients combinations of treatments and monitors their progress over 3–4 months, but moves to systemic medications as quickly as possible when appropriate.
“We need to hit as many of the four pillars of acne pathophysiology as we can,” reiterated Baldwin. “In the US, for mild acne we start with a retinoid and benzoyl peroxide, possibly including clindamycin, so we are hitting three of the four pillars.”11 “In reality, the toolkit of acne treatments is not that big. We have a handful of topicals, a handful of orals, and then we have our physical modalities. The art of treating acne is knowing how to combine those things.” According to USA guidelines,11 clascoterone, with conditional recommendations, can be considered as an additional medication to treat any level of severity of acne. However, in Baldwin’s opinion, it should be used right from the start of treatment.
CAN A TOPICAL ANTI-ANDROGEN MEDICATION TRANSFORM THE ACNE TREATMENT LANDSCAPE?
A topical anti-androgen treatment for acne has been a long-standing unmet therapeutic target, according to Baldwin, Herranz, and Layton. Widely used topical treatments do not address all elements of acne pathophysiology, while oral anti-androgen therapies that reduce sebum production can only be used in females.1
In the USA and in the UK, clascoterone is a first-in-class topical androgen receptor inhibitor for children ≥12 years old and adult acne patients of all genders.16,18,25,26 In the EU, clascoterone is for the treatment of AV in adult patients of all genders and of facial AV in 12–18-year-olds.27 Baldwin, Herranz, and Layton agree that clascoterone offers an alternative to the limitations of hormonal medications such as spironolactone, which does not have an indication foracne treatment and is restricted to usein females.28
Herranz is certain that having a topical medication that reduces sebum production through a novel mechanism will be welcomed by many patients who have tried everything that is currently available to them. Layton and Baldwin agree it is a very exciting addition to the acne treatment toolbox. For Layton, a topical treatment that reduces sebum is “a novel approach targeting a fundamental aspect of acne pathophysiology.” Before clascoterone, Layton explained: “We only had systemic oral isotretinoin for males and females licensed for severe disease, and off license hormonal therapies such as spironolactone for use in females to reduce sebum. Clascoterone provides a solution to an unmet need, […] and can be started at a young age (≥12 years old),18,27 achieving proven efficacy, and is generally well tolerated. It [clascoterone] is therefore an important novel product in terms of managing acne.”
Baldwin is clear that in their opinion, many patients may be considered for clascoterone and could benefit depending on their clinical profile and preferences. “Sebum is a foundational problem with every acne patient and suppressing it just makes sense,” they enthused, adding that sebum is a key contributor to AV and is also involved in its continuation. “By definition, reducing sebum is part and parcel of making anyone’s acne better,” Baldwin said. “The licencing of clascoterone is changing the treatment landscape. In my view clascoterone has the potential to completely change how we think about topical options for acne.”
According to Baldwin and Layton, like oral anti-androgens, clascoterone can take several weeks to reach full efficacy. “It is a bit slower than the other topicals, but it is generally well tolerated,”18,27 said Layton, so using it in combination with another topical in the early stages of treatment is preferable. Baldwin agrees and hypothesises that all the anti-androgens take longer to work than other types of medications because when treatment starts, the sebaceous glands are full of sebum, and it takes some time for the glands to clear. “I rarely use clascoterone as a monotherapy because it can take a while to see improvements, and I don’t want patients to be discouraged,” Baldwin added.
Sebum production is higher and earlier in children who develop AV.9 Clascoterone is licenced in the UK for use in children from 12 years old,18 and Layton has been using it to treat young patients in line with this. “It would be interesting to see whether we could prevent acne from progressing and modify the disease.” Layton said and continued: “If you could use it early in the course of the disease, you might be able to prevent comedones and inflammatory lesions developing, and in turn reduce the subsequent scarring and hyperpigmentation and the related psychological sequelae that can develop in the context of these clinical issues. In my experience to date, it is well tolerated and has consistent efficacy.”18
CONCLUSION
Early treatment intervention is crucial in AV to prevent both the physical and psychological impacts of the condition, and to reduce the burden of disease on young people in particular. Clascoterone is a first-in-class topical anti-androgen treatment that is well-tolerated.18,27 Expert dermatologists confirm that, in their clinical experience, it has generally been well tolerated when used to treat males and females aged over 12 years old and can be effective either alone or in combination with other medications.
CASE STUDIES
Case 1: USA Clinic
An adolescent male presented at the clinic with moderate AV affecting the face, but had ceased using topical retinoids as they caused significant irritant effects. Clascoterone was prescribed, which has been shown to reduce sebum production and increase skin hydration.29 The patient was advised to apply the clascoterone first and then put the retinoid on top.
Case 2: UK Clinic
A female with polycystic ovary syndrome with severe acne attended the clinic. She had previously completed two courses of oral isotretinoin very successfully but relapsed quickly with associated high sebum production. She was therefore treated with a third course of isotretinoin, which achieved clearance, and this was followed up with topical clascoterone, which was prescribed as a continuation to treatment to help maintain the improvements seen with isotretinoin, and to help prevent relapse by keeping skin sebum levels down.15,25