Overcoming Challenges and Exciting Developments in Lupus
![]()
Written by James Coker | Reporter, European Medical Journal | @EMJJamesCoker
![]()
 This year marks a major milestone in the history of lupus disease: it is the 70th anniversary since the haematologist Malcolm Hargraves and colleagues discovered the lupus erythematosus cell, a seminal moment that precipitated a number of advances in the diagnosis and treatment of lupus.1 Knowledge of the mechanisms of this chronic autoimmune condition, in which the resulting symptoms can affect a plethora of areas of the body including the skin, joints, heart, and kidney, has increased enormously since that time, making it substantially easier to diagnose and manage patients with the condition. Nevertheless, there is currently no cure, and as one of the so-called ‘invisible’ illnesses, diagnosis remains difficult. There is also limited awareness among the public and even doctors about its symptoms and manifestation. The EMJ was therefore delighted to speak with Mr Paul Howard, Deputy CEO of the UK-based charity Lupus UK. During a wide-ranging interview, we covered a number of topics, including advancements in treatments both in the past as well as possible areas to target in the future; initiatives from the charity to help patients pre and post diagnosis; ways of helping doctors diagnose and treat the condition, including the publication of recent guidelines; and finally areas of ongoing research that could lead to exciting results in the future.
This year marks a major milestone in the history of lupus disease: it is the 70th anniversary since the haematologist Malcolm Hargraves and colleagues discovered the lupus erythematosus cell, a seminal moment that precipitated a number of advances in the diagnosis and treatment of lupus.1 Knowledge of the mechanisms of this chronic autoimmune condition, in which the resulting symptoms can affect a plethora of areas of the body including the skin, joints, heart, and kidney, has increased enormously since that time, making it substantially easier to diagnose and manage patients with the condition. Nevertheless, there is currently no cure, and as one of the so-called ‘invisible’ illnesses, diagnosis remains difficult. There is also limited awareness among the public and even doctors about its symptoms and manifestation. The EMJ was therefore delighted to speak with Mr Paul Howard, Deputy CEO of the UK-based charity Lupus UK. During a wide-ranging interview, we covered a number of topics, including advancements in treatments both in the past as well as possible areas to target in the future; initiatives from the charity to help patients pre and post diagnosis; ways of helping doctors diagnose and treat the condition, including the publication of recent guidelines; and finally areas of ongoing research that could lead to exciting results in the future.
Advancements in Treatment
Mr Howard, who was initially inspired to help lupus patients because of the death of a close friend after a severe flare of the condition, described what he believed to be the advances in treatment that have had the biggest impact over the last 70 years. He cited steroids becoming widely available in the 1950s as improving survival by a remarkable extent: “Before steroids were used as a treatment, 83% of people with lupus died within the first 2 years, whereas following steroids about two-thirds of lupus patients would survive at least 2 years and about 50% would live at least 5 years,” he stated.
The use of diuretics and dialysis from the 1960s to treat kidney disease has also had a major effect on survival rates of lupus patients, with kidney conditions being the biggest cause of death for such patients in that period. In more recent times, Mr Howard hailed the introduction of immunosuppressants as a therapeutic option, as these have greatly reduced the reliance on steroids, which can have negative side effects when taken long-term. “These immunosuppressants are being used to reduce the amount of steroids and they’ve also helped increase survival rates from lupus again; survival rate at 2 years is now around 98% and so a lot of people with lupus now expect to live a near-normal life thanks to those advancements in treatments,” he commented.
Targeting Side Effects
Despite these encouraging figures, side effects from these treatments are still a major issue that needs addressing. A notable side effect from immunosuppressants is an increased risk of infection, which is becoming one of the leading causes of fatality in lupus patients. “Anything that can target a specific part of the immune system without limiting the overall immune response to infections would be a fantastic step forward,” said Mr Howard.
The impact of lupus on quality of life is also an area Mr Howard would like to see a greater emphasis upon since current treatments are unable to prevent many of these issues occurring. One example of this is fatigue, which can be debilitating. “There’s not really anything that targets fatigue, but even in people who are experiencing clinical remission where their lupus activity is quite low and a lot of their symptoms are stable and fairly manageable, the fatigue still tends to linger there and has a big impact on their lives, so I think that will be an area that definitely needs further treatments developed,” emphasised Mr Howard. That said, he has been reassured that greater efforts are starting to go into finding treatments that can tackle such areas, as well as the more overt medical symptoms.
A good example of this is a pilot study currently ongoing at University College London (UCL), London, UK, funded by Lupus UK and led by Dr Christopher Wincup. It is hoped this study will identify biomarkers for fatigue in lupus or any abnormalities that cause this fatigue to provide the basis for new types of therapies.
Self-Management
A recent initiative of Lupus UK to help patients manage their condition has been to fund specialist nurses in hospitals around the UK for a term of 5 years; their target is to fund a minimum of one new nurse per year. The invaluable support provided by these nurses has led to several hospitals, such as Addenbrooke’s Hospital, Cambridge, UK, to take on these nurses permanently at the end of the 5 years. They have been highly effective in saving time for consultants by providing patients with certain levels of information and support; for example, through the provision of important educational sessions like workshops for managing pain and fatigue that help enable patients to self-manage their condition. The positive effect that the lupus nurses have had has led to increased numbers of grant applications being received by Lupus UK.
Diagnosis
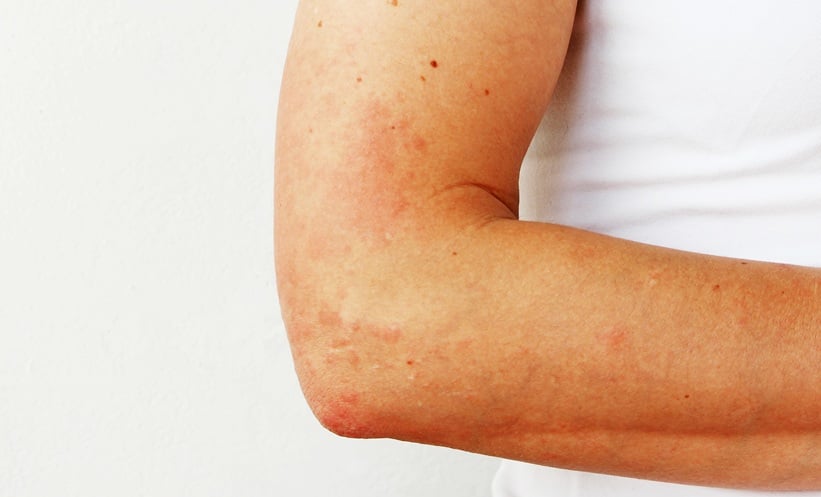
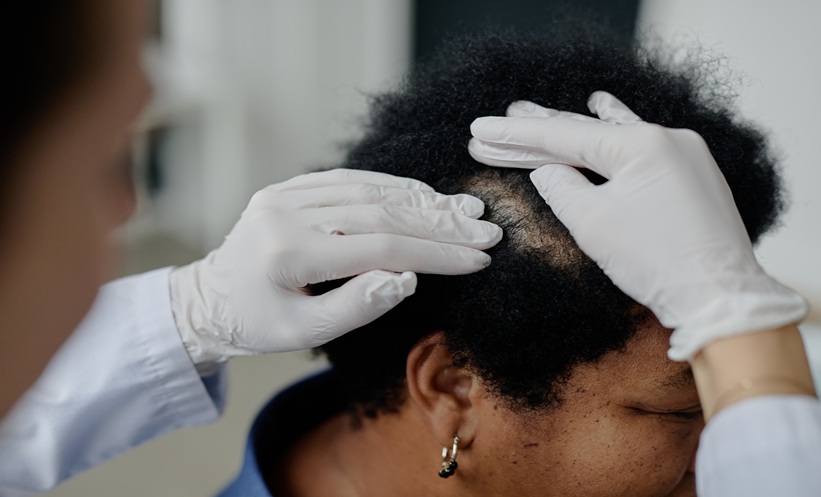
Diagnosis of lupus remains a major problem: recent survey results from Lupus UK showed that there was an average of 6.4 years between development of initial symptoms and diagnosis.2 Lupus is undoubtedly a very difficult condition to diagnose; in many cases there is a very gradual onset of symptoms that do not occur simultaneously and many symptoms, such as hair loss and skin rash, often share characteristics with a number of other conditions. Additionally, the symptoms tend to present differently between patients. However, Mr Howard does feel that doctors would benefit from extra training and information about lupus to help them in their practice. The charity has a book available named ‘Lupus Diagnosis and Treatment’3 aimed at primary care physicians, and is now working on a new edition, due to be released later this year. He also believes it is crucial that efforts are put into the development of more sensitive diagnostic methods, such as blood tests, to diagnose the condition on a more regular basis.
Guidelines
An important step in helping doctors diagnose and treat lupus came in October 2017, with the first UK guidelines for the management of systemic lupus erythematosus in adults from the British Society for Rheumatology (BSR),4 a development that Mr Howard believes could lead to profound enhancements in the diagnosis and care of lupus patients. “We haven’t been able to gauge the impact yet because it was only recently released, but I would say it is a very significant publication because there are many physicians who don’t have experience with diagnosing and treating lupus even within the specialist fields of rheumatology because it’s a relatively uncommon condition, and therefore having guidelines of best practice is really invaluable,” he elucidated.
Genetic and Environmental Causes
While it is extremely difficult to identify at-risk patients, there does appear to be increasing interest in establishing common causes of lupus. It is well known that lupus is much more prevalent amongst women (around 90% of cases). This has led to research suggesting that genetic faults in the X chromosome could be responsible for autoimmune conditions.5 Hormonal factors have also been proposed as a possible explanation for this much higher prevalence in females because lupus appears to be triggered in a lot of cases during changes in hormonal activity such as pregnancy and puberty.6 In addition, it is thought that genetic ancestry plays a major part in the onset; statistics show the disease is far more prevalent in those with a black, African, Jamaican, or Asian heritage,7 even taking into account other possible risk factors, such as socioeconomic. Mr Howard also made it clear that Lupus UK highlights these demographics when undertaking campaigns. In a recent survey of its membership,8 the charity found that black women had a significantly lower delay in diagnosis of lupus than Caucasian women, suggesting that this message might well be effectively getting through to these communities and also to doctors.
Despite this emerging evidence, much more research still needs to be undertaken to better understand the genetic links to the disease before any kind of genetic screen can be developed. Mr Howard also spoke about a recent growing interest in environmental triggers; research has shown possible links between the onset of the condition and environmental factors such as smoking, use of oral contraceptives, exposure to crystalline silica, and hormone replacement therapy.9
Room for Optimism
While there is clearly much more that needs to be understood to enable the development of prevention strategies in addition to improving diagnosis and treatment of lupus, there are many reasons for optimism. Awareness is improving, both among the public and doctors, of the symptoms to look out for and there is increasing literature outlining the genetic and environmental causes that could lead to the better identification of at-risk groups and prevention strategies in the future. Additionally, continuous improvements in treatments to manage the condition have been witnessed over the last 70 years or so, and significant efforts are now being put into finding therapies that start to tackle some of the side effects and quality of life issues that are associated with many current drugs. Mr Howard ended by saying: “There is more research being done now into the causes, the mechanisms, and the treatment of lupus than ever before.”
REFERENCES
- National Resource Center on Lupus by Lupus Foundation of America. The history of lupus. Available at: https://resources.lupus.org/entry/history-of-lupus. Last accessed: 29 March 2018.
- Lupus UK. People with lupus are waiting more than 6 years for a diagnosis in the UK. 2018. Available at: https://www.lupusuk.org.uk/six-year-diagnosis-delay/. Last accessed: 29 March 2018.
- Norton Y (Ed), Lupus Diagnosis and Treatment (2009), Lupus UK.
- Gordon C et al. The British Society for Rheumatology guideline for the management of systemic lupus erythematosus in adults: Executive Summary. Rheumatology. 2018;57(1):14-8.
- Sharma R et al. Rare X chromosome abnormalities in systemic lupus erythematosus and Sjögren’s syndrome. Arthritis Rheumatol. 2017;69(11):2187-92.
- Lupus International. SLE and Hormones. Available at: http://www.lupusinternational.com/Living-With-Lupus/Pregnancy-and-Lupus-/Hormones-and-SLE.aspx. Last accessed: 29 March 2018.
- National Resource Center on Lupus by Lupus Foundation of America. Lupus facts and statistics. Available at: https://resources.lupus.org/entry/facts-and-statistics. Last accessed: 29 March 2018.
- Lupus UK. Membership Survey Results Summary. 2018. Available at: https://www.lupusuk.org.uk/member-survey-results/. Last accessed: 29 March 2018.
- Parks CG et al. Understanding the role of environmental factors in the development of systemic lupus erythematosus. Best Pract Res Clin Rheumatol. 2017;31(3):306-20.
To find out more about the work of Lupus UK, click here.