METFORMIN reduced the incidence of intermediate age-related macular degeneration (AMD) by nearly 40% in people with Type 2 diabetes over 5 years in a 2026 observational study.
Metformin as a Potential Treatment for All Stages of AMD
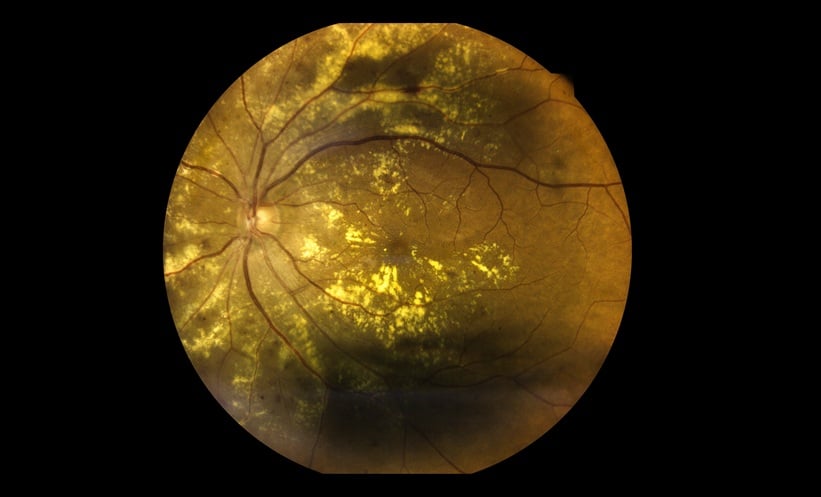
AMD is a common cause of blindness in high-income countries. It has previously been established that treatment has a high patient and financial burden, with limited long-term success.
Prior analysis has also identified metformin as a potential treatment for all stages of AMD. Researchers also noted that the common diabetes drug is readily accessible and has a strong safety profile.
Metformin Gave a 37% Lower Risk of AMD in Type 2 Diabetes
Researchers analysed more than 2,500 participants aged 50 or above who attended retinopathy screening in 2011 and were enrolled to the Individualised Screening for Diabetic Retinopathy study. All had Type 2 diabetes and gradable fundus photographs. Authors collected information on metformin prescription from GP records.
Those prescribed oral metformin had a 37% lower risk of intermediate AMD by 5 years. The results are consistent with known biological mechanisms, given metformin’s potential favourable effects on AMD progression, researchers reported.
Metformin Across Other Stages of AMD
In univariate analysis, metformin was associated with a lower incidence of late AMD, however the link was not significant after adjustment for age and sex. There was no association between metformin and early AMD incidence.
Limited Data and Generalisability
Researchers did not have data regarding the dose, duration of prior use, or compliance of metformin use. Further, there were only a relatively small number of participants developing advanced AMD – an inevitability in population-based studies.
The study also used colour fundus photographs as opposed to optical coherence tomography, the latter of which was unavailable but exhibits better sensitivity at detecting AMD. Inherently, results cannot be generalised past people with diabetes.
Future Research
Authors emphasised that further studies should focus on reducing the incidence of AMD at an intermediate stage, before vision loss, leading to favourable outcomes for patients and health systems.
References
Romdhoniyyah DF et al. Metformin and incidence of age-related macular degeneration in people with diabetes: a population-based 5-year case-control study. BMJ Open Ophthalmol. 2026;DOI:bmjophth-2025-002339.
Bourne RRA et al. Prevalence and causes of vision loss in high-income countries and in Eastern and Central Europe in 2015: magnitude, temporal trends and projections. BR J Ophthalmol. 2018:102:575-85.
Rofagha S et al. Seven-year outcomes in ranibizumab-treated patients in ANCHOR, MARINA, and HORIZON: a multicenter cohort study (SEVEN-UP). Ophthalmology 2013;120:2292–9.
Nadeem U et al. Using Advanced Bioinformatics Tools to Identify Novel Therapeutic Candidates for Age-Related Macular Degeneration. Transl Vis Sci Technol 2022;11:DOI:10.1167/tvst.11.8.10.
Vaughan EM et al. Reducing the Burden of Diabetes Treatment: A Review of Low-cost Oral Hypoglycemic Medications. Curr Diabetes Rev 2020;16:851–8.
Featured image: Richman Photo on Adobe Stock