SPINAL epidural arteriovenous malformations (SEAVMs) are rare, complex vascular lesions of the spine that most often affect younger adults. They commonly present with compressive myelopathy, causing motor weakness, sensory disturbances, radicular pain, and sometimes bladder or bowel dysfunction. SEAVMs differ from the more common spinal dural arteriovenous fistulas (SDAVFs) in age at presentation, angioarchitecture, and clinical features, making an accurate diagnosis important for treatment planning.
Imaging Detects Key SEAVM Features
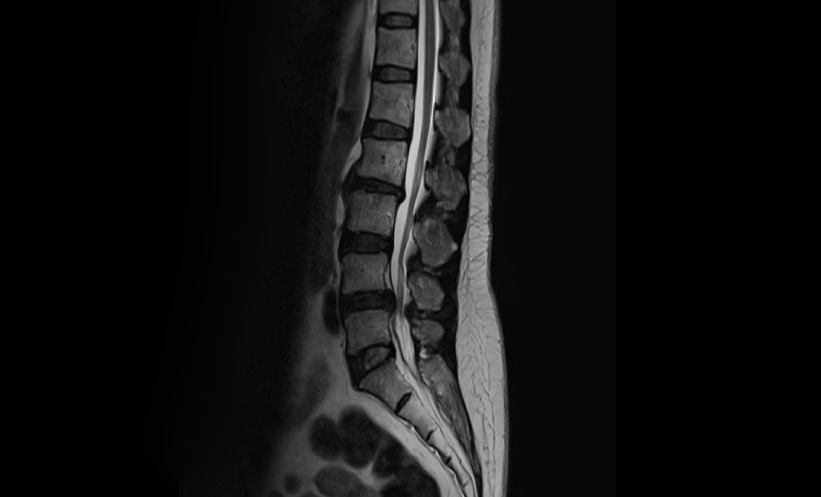
In this retrospective review of 24 patients treated between 2010 and 2025, MRI revealed epidural venous sacs and cord signal changes in 83% of cases. CT, available for 18 patients, showed vertebral osseous changes in 83% of scans. Lesions were mostly located in the lower thoracic spine, and intradural venous reflux was uncommon. These imaging features, particularly osseous involvement and venous sacs, help clinicians characterise SEAVMs and inform treatment strategies.
Endovascular Therapy Shows Efficacy and Strong Recovery Outcomes
Nineteen patients underwent targeted endovascular embolisation, with N-butyl cyanoacrylate (NBCA) used in 18 cases and successful venous sac penetration achieved in 17. There were no major periprocedural neurological complications. Functional outcomes were significant: the mean Karnofsky Performance Status (KPS), which measures patients’ ability to carry out daily activities, improved from 51.1 to 80.0, indicating a shift from needing assistance to largely independent function. Angiographic results ranged from complete to moderate obliteration of the malformations.
Limitations and Clinical Implications for SEAVM Management
The sample size was modest, follow-up varied, and imaging and endovascular techniques evolved over the 15-year period, introducing potential biases. Not all patients underwent long-term angiographic surveillance, so residual shunts or late recanalisation may have been missed.
The study confirms that SEAVMs represent a distinct spinal vascular lesion. MRI and CT frequently reveal osseous involvement and epidural venous sacs, supporting accurate diagnosis and guiding treatment decisions. Targeted endovascular embolisation of the venous sac or fistulae appears safe and often results in substantial clinical improvement, providing durable functional benefit for younger patients with these rare lesions.
Reference
Shah SA et al. Spinal epidural arteriovenous malformations: clinical, imaging, and angioarchitectural characteristics with endovascular treatment outcomes—a single-centre experience. Clin Radiol:2026;DOI:10.1016/j.crad.2026.107270.
Featured image: Issara on Adobe Stock