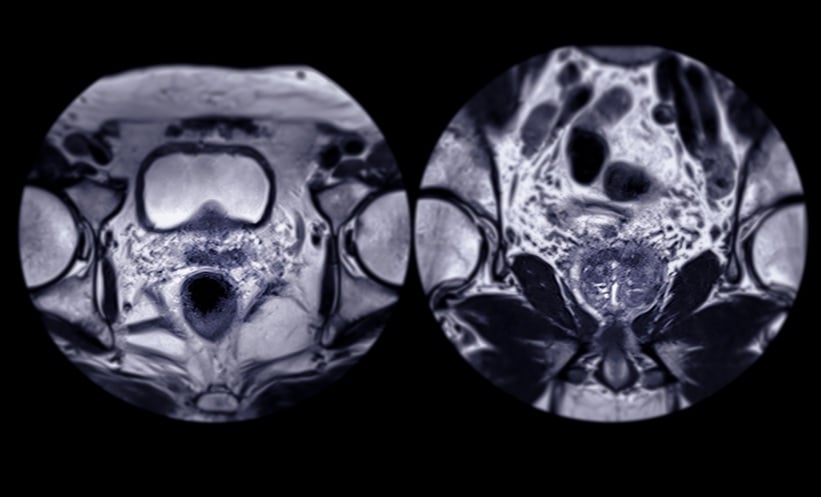
ARTIFICIAL intelligence (AI) integrated with magnetic resonance imaging (MRI) significantly improved biopsy decision-making in prostate cancer diagnosis, according to new research presented at the 41st Annual Congress of the European Association of Urology 2026.
Prostate cancer remains one of the most commonly diagnosed cancers in males worldwide. Detecting clinically significant disease while avoiding unnecessary biopsies has long posed a challenge for clinicians. Imaging techniques such as biparametric MRI (bpMRI) have become an important component of the diagnostic pathway, but interpretation can vary depending on the reader’s experience. Researchers therefore investigated whether AI-assisted imaging could improve the accuracy and efficiency of prostate cancer diagnosis.
AI Assistance Boosts Reader Performance in Prostate Cancer MRI
The retrospective study analysed patients who underwent pre-biopsy MRI between 2021 and 2024. Five radiology readers participated in the analysis, including two experts and three basic-level readers according to European Society of Urogenital Radiology–European Society of Urogenital Imaging criteria.
Each reader initially reviewed bpMRI scans independently and assigned Prostate Imaging Reporting and Data System (PI-RADS) scores. After a 45-day washout period, the same scans were reassessed with AI-generated reports from a decision-support platform, allowing investigators to compare performance with and without AI assistance.
Researchers focused on two key measures: biopsy selectivity, which reflects how well imaging identifies clinically significant cancer (Grade Group ≥2), and biopsy efficiency, which compares significant cancer detection with less serious or benign findings.
Across both diagnostic thresholds tested, AI support improved overall performance. At a PI-RADS threshold of ≥3, biopsy selectivity increased from 3.889±0.884 to 5.078±1.602, while biopsy efficiency rose from 1.688±0.404 to 1.992±0.053. When a combined threshold was applied – PI-RADS ≥4 or PI-RADS 3 with prostate-specific antigen density ≥0.15 ng/ml² – selectivity increased from 4.317±0.735 to 5.400±1.188 and efficiency improved from 2.166±0.699 to 2.363±0.250.
Notably, the greatest improvement occurred among less experienced readers. With AI decision support, basic readers achieved efficiency scores comparable to expert radiologists, suggesting that AI may help standardise prostate cancer diagnosis across different levels of clinical expertise.
Implications for Biopsy Decision-Making
The findings also showed that the composite diagnostic threshold combining PI-RADS scores with prostate-specific antigen density consistently produced the best biopsy selectivity and efficiency.
Among expert readers, AI support produced modest gains in selectivity while efficiency remained stable. However, the substantial improvements seen among basic readers highlighted AI’s potential to reduce variability in prostate cancer diagnosis and support more consistent clinical decisions.
Although the analysis was retrospective, the results suggested that AI-assisted bpMRI interpretation could help clinicians better identify patients who would benefit from biopsy while reducing unnecessary procedures. Future prospective studies will be needed to confirm whether these improvements translate into better outcomes in routine prostate cancer diagnosis.
Reference
Sighinolfi MC et al. Improving biopsy decision-making in prostate cancer using AI-assisted biparametric MRI. Abstract 0485. EAU26, 13-16 March, 2026.
Featured image: samunella on Adobe Stock