BACKROUND AND AIMS
Asthma is the most common chronic disease of childhood, with a prevalence of 4.4–30.6% among school-age children in European birth cohorts.1 The COVID-19 pandemic has affected healthcare services worldwide, and many clinics have ceased office appointments and stopped taking new patients.2 However, only few clinics reported more negative asthma disease control during the COVID-19 era.2
The objective was to evaluate the paediatric allergology unit and whether COVID-19 has affected physician–patient contacts or feedback of care. The hypotheses were that there was no significant reduction to patient contacts and the patients seemed to be pleased with telemedical visits.
MATERIALS AND METHODS
This was a register-based study from the electronic medical records at the Helsinki University Hospital, Skin and Allergy Hospital Paediatric Allergy Unit, Helsinki, Finland, from 1st April 2019 to 30th October 2020.
The proportion of telemedical visits via Terveyskylä internetplatform3 and telephone contacts was analysed. The patient feedback was documented using Net Promoter Score value (NPS),4 which was collected via short message service of the hospital.
Statistical analysis was performed with SPSS version 22 (IBM, Armonk, New York, USA). The Mann–Whitney U test was used for continuous variables and chi-squared for categorical data.
The monthly number of patients at the intensive care units in the Hospital District of Helsinki and Uusimaa was calculated as the mean number of patients on Wednesdays of each week according to the Finnish Institute for Health and Welfare (THL) database.5
RESULTS
In the paediatric allergology unit, the decrease of physician visits in April–May 2020 compared to 2019 was 9.7% (1,188 versus 1,315 visits). In April–October, the decrease was only 5.4% (4,039 versus 4,270 visits).
None of the 4,270 visits from April to October 2019 were telemedical. In April–May 2020, during the first peak of COVID-19 incidence in Helsinki, 59% of visits (n=698/1,188), and 19% (n=543/2,851) between June–October 2020, were performed using telemedicine (p<0.001) (Figure 1).
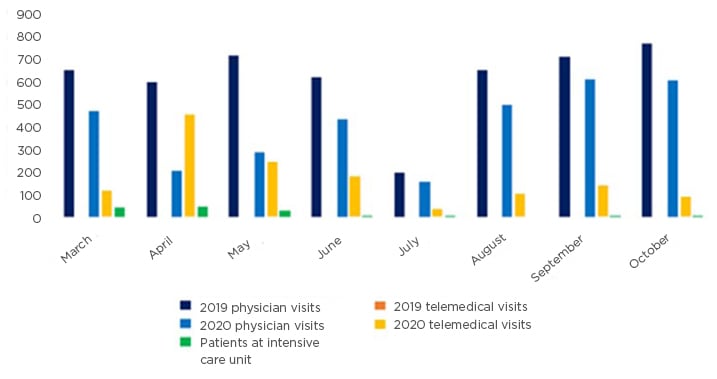
Figure 1: Physical and telemedical visits and number of patients in intensive care unit.
NPS feedback was improved significantly during the COVID-19 era from April to October 2020 compared to the period from November 2019 to March 2020 (median values of 76.9, range: 62.4–82.8; and 63.2, range: 61.1–65.4, respectively; p=0.018). The mean number of feedback per month was 120 from November to March and 110 from April to October.
CONCLUSION
There was only a minor decrease of patient visits, contacts, and appointments during the COVID-19 period. The majority of contacts in spring 2020 were performed using telemedicine. Also, after May 2020, 20% of visits were performed via internet or telephone. Patients were satisfied: NPS feedback was improved to the COVID-19 era.








