Written by Kirstie Turner | Editorial Administrator, European Medical Journal![]()
INTRODUCTION
There is a high prevalence of allergic disease throughout Europe: 17.0–29.0% prevalence of allergic rhinitis,1 1.3–11.0% asthma,2 and 26.5% atopic eczema,3 among others. This high level of allergic disease places a burden of care that must be met by highly trained specialists. Fyhrquist et al.4 carried out a study regarding the availability of care services and specialist training availability. The findings are discussed in their paper: ‘The roadmap for the allergology specialty and allergy care in Europe and adjacent countries. An EAACI position paper’. This article will summarise the methodology, findings, and analysis of this European Academy of Allergy and Clinical Immunology (EACCI) position paper.
METHODOLOGY
The study was conducted using a survey created by the EAACI National Allergy Society Committee and the Union Européenne des Médecins Spécialistes (UEMS) Section and Board (S&B) of Allergology. The survey was compiled using questionnaires developed in previous research: the 2016 NASC registry data collection and the UEMS S&B and speciality committee 2016 survey for UEMS delegates. The survey questioned participants on the level of care services and training availability for the specialities and sub-specialities included within allergic care. Additionally, a strengths, weaknesses, opportunities, and threats (SWOT) analysis of the allergic disease care options was completed. This was sent to 51 NASC members and 30 countries linked with UEMA S&B, most of which were European.
RESULTS AND DISCUSSION
Speciality and Subspeciality
An important outcome of the questionnaire was the confirmation that most countries had recognised the full speciality. However, a small number of countries considered allergology as a subspeciality and some recognised neither the speciality nor subspeciality. The results also showed the number of new registered specialists and subspecialists each year in the surveyed countries: Italy, Spain, and Poland had the most specialists, with 40–42, 40–55, and 30, respectively; Germany was found to have the most new subspecialists each year, with 140 registering, although this number is decreasing. There was a mixed response in terms of the number of specialists and subspecialists being sustained, growing, or falling, although the majority of responding countries declared a sustained or growing number, which is positive news for the discipline. The researchers highlighted the importance of free movement for these specialists and subspecialists.
The number of subspecialists and specialists per 100,000 people varied greatly across Europe, highlighting the lack of standardisation across allergy disease care. For instance, there are 5.96 full speciality allergologists per 100,000 people in Georgia, while the corresponding figure for Luxembourg is 0.17. Additionally, although allergic disease is highly prevalent, the discipline reports a lower number of specialists per 100,000 people than many other specialities. For instance, dermatology has 5.84 per 100,000, compared to allergologists and subspecialists for allergology, which saw results of 1.81 and 1.84, respectively: an estimated 1 subspecialist available for every 53–54,000 people. However, it should be noted that this figure, for many countries, is simply a theoretical estimate as many specialists do not work as allergologists following completion of their study.
Training for Speciality and Subspeciality
The paper also goes on to highlight the variation of training in the speciality. Training duration for specialists and subspecialists ranges from 1.5–7.25 years, with a mean duration of full speciality and subspecialty measuring at 4.55 and 5.08 years, respectively. A point for concern was that many training schemes were not meeting the current requirements for the speciality of Allergology and Clinical Immunology (as amended in 1997–2003), which should be at least 2 years in a common trunk and a minimum of 3 years in the speciality. It was recommended that these requirements should be updated to reflect current training standards. Furthermore, the authors suggested efforts should be made to ensure countries followed harmonised training, while preserving the ability of individual countries to organise specialities nationally. While the requirements were often not being met, there were grounds for positivity when considering training for a subspeciality in Allergology. EAACI’s recommendation was that the minimum training requirement here was 18 months, a duration that most countries were exceeding.
Strengths, Weaknesses, Opportunities, and Threats Analysis
The SWOT analysis completed within the survey provided an in-depth exploration of allergic disease care. Participant responses often contradicted one another; diversity between the surveyed countries can be attributed to different local circumstances and policy, resulting in differing priorities and opinions. For example, a speciality could be present in one country, and therefore seen as a strength, or could be lacking in another and therefore seen as a weakness, or even a threat.
The low attractiveness of the role or specialisation was seen as a threat by some countries. Some also highlighted the danger of weak prioritisation of the discipline among authorities. A lack of funding and reimbursement opportunities were also a key concern, along with a need for standardisation and more prevalent availability of immunotherapy products.
On the other hand, several opportunities were identified, including the discipline’s continual growth, improved awareness of allergic diseases, better methods of prevention, focus on improvements of patient care, and investment in young doctors to specialise. The researchers considered answers given by ≥3 country representatives to be the most important topics. An overview of the SWOT analysis can be seen in Table 1.
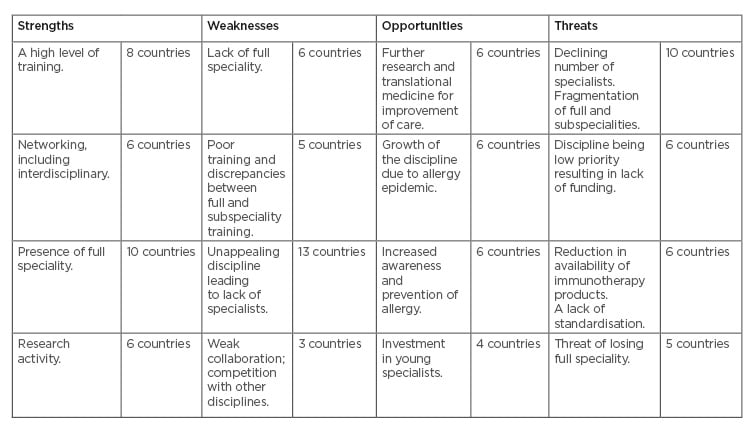
Table 1: Strengths, Weaknesses, Opportunities, and Threats analysis of allergic disease care.4
CONCLUSIONS
The researchers concluded that the specialty of allergology is recognised in most European countries, as well as in adjacent countries. There are, however, considerable variations across Europe regarding the care services available. Diversity within care systems includes the type of caregivers, specialist numbers, the training of specialists, and availability of training. Therefore, they recommended that standardisation of training should be implemented for allergologists and subspecialists. The authors recognised that having a mix of precise data and estimations was a limitation of the survey.
It was further recommended that there should be investment to train and specialise young doctors, as well as to create further opportunities for a full speciality in countries. The authors also outlined that free movement of allergologists should be better facilitated. The paper offers an important evaluation of the care availability for allergy diseases and well-informed recommendations to improve the availability and standard of care.








