Acrokeratosis paraneoplastica (Bazex syndrome) is a paraneoplastic skin condition that can be found in the context of various internal malignancies, including squamous cell carcinoma of the head and neck, carcinomas of the aerodigestive tract, cholangiocarcinoma, and lymphoma.1,2 Men >40 years of age are the most commonly affected.1
The clinical aspects of this condition may mimic psoriasis, eczema, lupus erythematosus, hereditary palmoplantar hyperkeratosis, pityriasis rubra pilaris, mycosis fungoides, or syphilis.2 For this reason, there can be a delay in recognising this entity, which, therefore, may extend the period of time until a neoplasm diagnosis is established. Sometimes, the cutaneous manifestations may coincide with the tumour diagnosis or can appear later in the evolution revealing metastases.1,2 The clinical appearance of the eruption has three stages of development. Initially, acrokeratotic lesions are represented by scaly erythematous to violaceous papule and plaques can be observed on the fingers and/or toes, ears, and nose. Nail apparatus involvement can be noticed. In the second stage, the lateral part of the palms and soles becomes affected by keratoderma, without affecting the centre of the palms and soles. In the last stage, the eruption may extend to the limbs, trunk, and scalp.1 Histopathological findings are nonspecific. Acrokeratosis paraneoplastica is usually refractory to topical (corticosteroids or keratolytic products) or systemic (acitretin) treatments.3 The best approach is based on treating the underlying malignancy, which will lead to the resolution of the skin lesions in a few months in >90% of cases.3,4
We presented the case of a 50-year-old female patient who was examined for hyperkeratotic lesions affecting the hands and feet, which she had noticed a few months before. She was previously diagnosed with chronic eczema, for which she received topical corticosteroids and emollients without improvement. The eruption worsened in the weeks leading up to the examination and were associated with an intense pain confined to the skin lesions. On dermatological examination, hyperkeratotic erythematous and violaceous plaques were present on the palmoplantar area and associated with scaly plaques on the dorsal part of the toes with a tendency to extend over the medial part of the feet. A few violaceous shiny papules with a lichenoid aspect were noticed on the dorsal part of the hands. The patient was cachectic and depressed. Her medical history revealed a diagnosis of pulmonary carcinoma of the right lung 3 years before, for which a complete right pneumonectomy was performed, as well as chemotherapy and radiotherapy. The presence of psoriatic hyperkeratotic acral lesions, resistant to topical steroids, in a patient previously diagnosed with an internal malignancy resulted in the diagnosis of Bazex syndrome or acrokeratosis paraneoplastica.
The appearance of Bazex syndrome was concomitant with the extension of the carcinoma to the left lung and with the occurrence of metastases. This case is of particular interest considering that the skin disorder was absent 3 years before, that the ears and the nose were not involved at the time of the primary tumour diagnosis, and that it was associated with an intense pain.
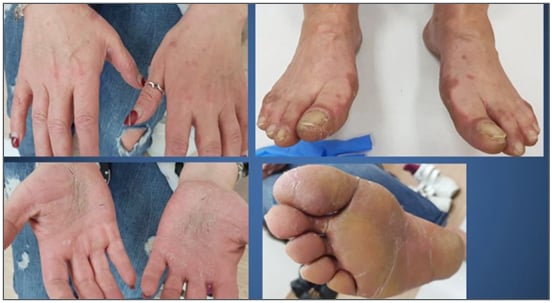
Figure 1: Bazex syndrome.
Hyperkeratotic erythematosus and violaceous plaques on palmoplantar area, associated with scaly plaques on the dorsal part of the toes and a tendency to extend over the medial part of the feet.








