BACKGROUND AND AIMS
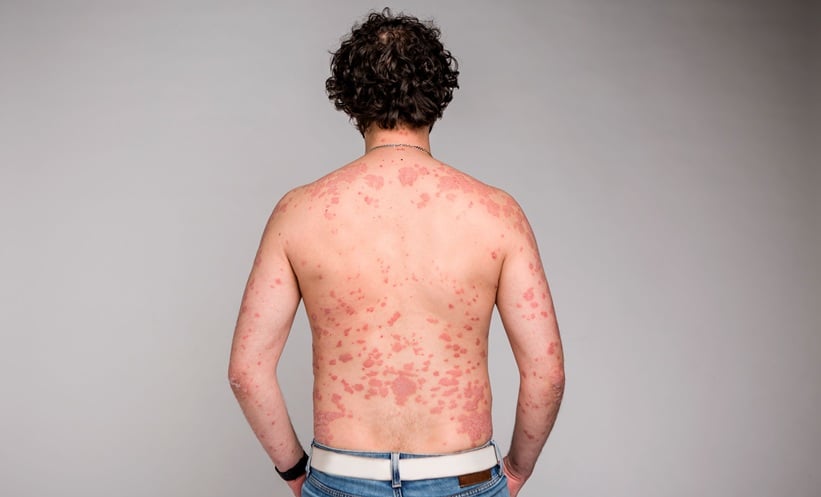
Chronic urticaria (CU) is a common skin condition defined as an urticaria lasting for more than 6 weeks. It is divided into chronic spontaneous urticaria (CSU) and inducible urticaria (IU).1 The aim of this study was to assess the epidemiological and clinical features of CU, as well as its impact on the quality of life of patients.
MATERIALS AND METHODS
This was a monocentric, descriptive, retrospective study spanning 28 months from January to April 2021. Patients with different forms of CU, seen in the outpatient Department of Dermatology at the Military Hospital of Tunis, Tunisia, were included regardless of their age and sex.
RESULTS
Among 60 patients, 63% had CSU and 35% had IU, while the remaining patients (2%) had both CSU and IU. The prevalence of CU was equal in both sexes (male-to-female sex ratio: 1.06). The mean age was 29.7 years (range: 2–82 years), with 55% of cases occurring in patients aged between 21 years and 40 years. Among patients with IU, the most common types of urticaria were cholinergic urticaria (43%), followed by dermographism (24%), and cold urticaria (19%). Eighteen (30%) patients had other allergic diseases and 13% had family history of urticaria. An autoimmune disease was found in 7% of patients. All of them had Hashimoto’s disease. Generalised eruptions of wheals were more common in patients with CSU (76%), whereas localised eruptions were preponderant in IU (63%). Nine patients (15%) presented an oedema of eyelids or lips. Two patients (3%) have been hospitalised due to urticaria. Second-generation antihistamines were prescribed as a first-line treatment in 59 patients, one individual was prescribed corticosteroids. Wheals completely disappeared in 43% of cases. The treatment reduced the symptoms in 27% of patients, whereas it had no effect in 28% of them. Pruritus was the most bothersome symptom in 90% of patients, causing disruption of daily living and sleep, followed by skin lesions (7%). CU was the cause of sick leave in 20% of patients.
DISCUSSION AND CONCLUSIONS
Most of the results were consistent with similar studies; however, the sex codominance was rarely reported. In line with the literature, CSU was more frequent in this study than IU (70–82% in the literature).2 CU is a challenging condition as the treatment is not always successful, especially in CSU. Almost all the patients received second-generation antihistamines as a first-line treatment. The majority of patients in different studies were treated with second-generation antihistamines, with up to 40% of remission reported by Jankowska-Konsuret et al.2,3 The lack of some drugs, such as omalizumab, in the authors’ country did not allow them to compare the effectiveness of the different treatments. In all the previous studies, as in this one, the most bothersome symptom was pruritus, accounting for 16.3% of absenteeism in a study in Poland.2