Abstract
Skin, with its many biological functions, has a unique aesthetic value and determines the self-image and psyche of the person in terms of how they think about themselves. In modern times, smooth-textured flawless skin is a preferred characteristic. Any change in this highly aesthetic organ due to a disease has significant repercussions on personal and social life. There is a bidirectional relationship between dermatological diseases and psychiatric disorders. These can be studied under three categories: psychophysiological disorders, which are dermatologic conditions that fluctuate in clinical severity according to psychological state; primary psychiatric disorders presenting with dermatological manifestations; and dermatological adverse effects of psychotropic medication. Psychiatric disorders are highly prevalent in dermatological patients. Dermatologists should be aware of the psychological factors contributing to or arising from skin disease in common dermatological conditions. Management of psychiatric comorbidities in these patients will help decrease the stigma, stress, and distress, and thus will improve the quality of life of patients and overall treatment success.
INTRODUCTION
The skin is the largest organ in the body and serves many functions, including acting as a barrier, immune regulator, and endocrine organ, as well as also having an aesthetic role. There is a strong bidirectional relationship between dermatological diseases and psychiatric disorders. The origin of this relationship may be due to common neurobiological, psychological, and social aspects. Skin diseases account for 12.4% of all the diseases seen by general practitioners.1 The prevalence of psychiatric morbidity in dermatological outpatients is reported to be 25%.2 Despite the high prevalence of psychiatric morbidity, it has received scarce attention. Dermatological diseases can increase the risk of developing or worsening an existing psychiatric disorder. The relation between the psychiatric morbidity and skin diseases can be understood in four ways:
- The skin diseases of a chronic nature and disfigurement may frequently affect the quality of life of patient; thus, increasing psychiatric morbidity.
- Less frequently, skin diseases may result from primary psychological diseases, such as obsessive compulsive disorders, impulse control disorders, and delusional disorders.
- Both skin findings and psychiatric complaints may develop secondary to a disease, such as systemic lupus erythematosus.
- Dermatological adverse effects that are due to psychotropics, such as lithium, lamotrigine, and chlorpromazine.
NEUROBIOLOGICAL LINK BETWEEN MIND AND SKIN
There is an intricate relationship between stress and skin conditions. Stress exerts its effects on skin mainly through the hypothalamic-pituitary-adrenal axis. The skin has developed a fully functional, peripheral hypothalamic-pituitary-adrenal system in which corticotropin-releasing hormone (CRH), adrenocorticotropic hormone, and their receptors are produced in skin cells.3 CRH is produced in the epidermis and hair follicles by keratinocytes, melanocytes, sebocytes, and mast cells upon stress. CRH inhibits proliferation by arresting cells at the G0/1 cycle and induces differentiation by calcium influx and the AP-1 transcription pathway.4 In mast cells, CRH induces degranulation and increases vascular permeability, demonstrating proinflammatory functions.5 The adrenocorticotropic hormone stimulates interleukin-18 production in skin keratinocytes; interleukin-18 is a proinflammatory cytokine that enhances T cell activity and promotes T-helper type 2 cytokine production.6
Stress also induces the release of catecholamines through the sympathetic-adrenal medullary axis, which excretes adrenaline. Adrenaline acts by binding to a variety of adrenergic receptors, leading to decreased skin blood flow, and altered immune and inflammation functions, including lymphocyte trafficking, circulation, proliferation, and cytokine production.7 The skin also holds a peripheral catecholamine system where adrenaline is synthesised in keratinocytes while the adrenergic receptors are present in both epidermal keratinocytes and melanocytes. Adrenaline, through its action on beta-2 receptors, regulates both epidermal proliferation and differentiation.8
The skin is highly innervated and, as such, peripheral nerves can also impact skin health through secreted factors like neuropeptides (substance P) and neurotrophins (NT). Substance P is a stress-related proinflammatory neuropeptide that is released from cutaneous peripheral nerve terminals. Nerve growth factor, one of four NT family members, binds to the high-affinity tyrosine kinase receptors (TrkA, TrkB, and TrkC) and low affinity p75 NT receptor promotes neurogenic inflammation by stimulating cytokine releases from skin mast cells.9
Stress also has a negative impact on wound healing. Anxiety and depression are associated with delayed wound healing in chronic wounds10 and it was found that chronic stress leads to elevated cortisol and dysregulation of healing biomarkers, which contributes to a delay in wound healing.11
PSYCHOPHYSIOLOGICAL DISORDERS
Psychophysiological disorders are when the course of the skin disease is affected by the psychological state of a person or psychological disorders arising due to dermatological diseases. Patients with real and perceived imperfections in important body image areas, such as the face, scalp, hands, and genital area, due to various skin diseases, are prone to distress. Acne, psoriasis, atopic dermatitis (AD), and Hansen’s disease are common skin diseases that are well studied with respect to psychosocial health.
Acne
Acne is one of the most prevalent skin conditions, affecting >85% of teenagers.12 In 1948, Sulzberger and Zaidens13 wrote: “There is no single disease which causes more psychic trauma and more maladjustment between parents and children, more general insecurity and feelings of inferiority, and greater sums of psychic assessment than does acne vulgaris.” The change in the skin’s appearance may give rise to a changed body image that, in turn, is known to lead to anger, fear, shame, anxiety, depression, embarrassment, and stigmatisation within peer groups. Its substantial influence is likely related to its typical appearance on the face and would also explain the increased unemployment rate of adults with acne.14 In a study carried out in southern India by Durai et al.,15 it was found acne has a significant impact on quality of life. In another study of Iranian patients, the prevalence of anxiety was 68.3% in patients and 39.1% in the control group.16 The psychological effect of acne is unique for each patient; therefore, patients should be asked how much their acne bothers them, regardless of how severe it appears to physicians. Acne in adolescence can affect self-image, assertiveness, and the formation of friendships. The face is very important to body image, and as such young men with severe scarring acne are at particular risk of depression and suicide.17
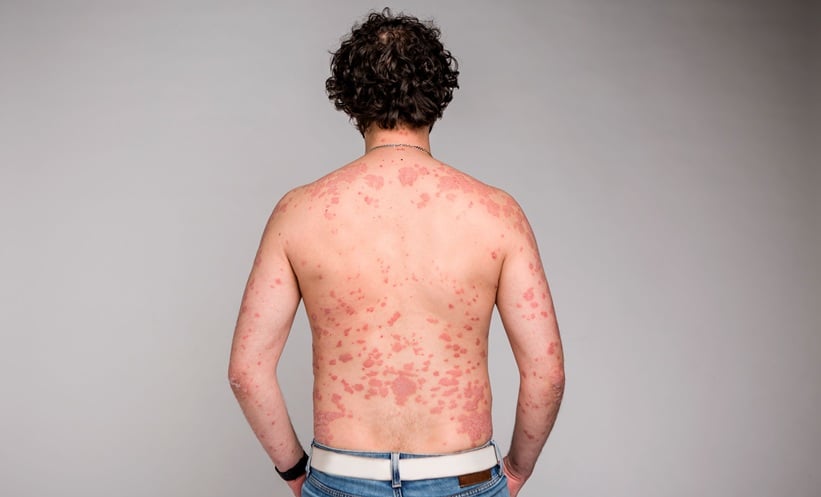
Psoriasis
Psoriasis can be considered a psychosocial skin disease. It is a chronic inflammatory condition of the skin associated with significant morbidity. The prevalence of psoriasis in children ranges from 0–2.1% and in adults it varies from 0.91–8.5%18 and comprises 2.6% of skin-related visits to primary care physicians.19 The morbidity in people with psoriasis is due to itching, scratching, bleeding spots, noticeable flakes, and unsightly physical appearance. People affected have poorer social lives, difficulties in getting jobs, and decreased quality of life due to embarrassment and the feeling of physical unattractiveness.20 The most prevalent psychiatric comorbidities in psoriasis are related to sexual (71%)21 and sleep problems (50%).22 In a study conducted in eastern India in a tertiary centre evaluating the psychiatric morbidity in psoriasis patients, 62.5% had psychiatric morbidity, compared with 18.5% in the control group. Guttate psoriasis had maximum association with psychiatric morbidity (100%), followed by plaque type (63.6%), and palmoplantar type (42.8%). The most common psychiatric symptom in psoriasis patients was anger (58%), followed by discomfort (52%), social problems (52%), cognitive impairment (50%), embarrassment (50%), physical limitation (48%), fear (48%), and depression (44%).23 In another study from northern India, patients with psoriasis were evaluated in two stages using the mini international neuropsychiatric interview (MINI), and it was found that 45% have psychiatric morbidity, with dysthymia (28.85%) followed by major depression (15.38%) as the next most common psychiatric disorders.24 In the same study, suicidality was found in 13.6% of patients. Furthermore, certain psychiatric conditions like depression and anxiety can worsen the severity of psoriasis.25
Atopic Dermatitis
AD is a chronic inflammatory skin disease, characterised by pruritic and eczematous skin lesions with a series of exacerbations and remissions. AD onset is commonly during childhood and adolescence. It affects 15–20% of children26 and constitutes approximately 15% of the skin-related concerns in general practice.19 Patients with AD experience unrelenting pruritus, which is the primary source of morbidity. Children with AD also experience significant psychosocial and behavioural issues compared to their peers. Parents of children with AD report increased fussiness, irritability, and crying in their children.27 Daud et al.28 found children with severe eczema, when compared to unaffected children, had difficulty with psychosocial adjustments and displayed more clinginess and fearfulness. In a study conducted to quantify the mental health burden associated with paediatric AD, it was found that the odds of having attention-deficit hyperactivity disorder was significantly increased in children with AD compared to non-AD controls (odds ratio: 1.87; 95% confidence interval [CI]: 1.54–2.27). In the same study the adjusted odds ratios for depression, anxiety, conduct disorder, and autism were 1.81 (95% CI: 1.33–2.46), 1.77 (95% CI: 1.36–2.29), 1.87 (95% CI: 1.46–2.39), and 3.04 (95% CI: 2.13–4.34), respectively.29 Adult patients with AD can have substantial salary loss from missed work, as well as financial strain due to multiple medications and possibly consultations with alternative medicine practitioners. In particular, work-related adult hand dermatitis is a common cause of worker compensation benefits and requires workplace modification.
Hansen’s Disease
Hansen’s disease (leprosy) is an uncommon skin disease in the Western world, but leprosy cases are still seen in developing nations. Hansen’s disease is associated with significant morbidity in the patient and their family. In society, there is significant stigma towards Hansen’s disease patients, due to factors such as fear of acquiring disease from patients, disfigurement, and deformities. The psychosocial issues faced by people with leprosy are high, and the rate of divorce, unemployment, displacement from area of residence, and loss of social status are common.30 Studies have shown that stigma is greater in educated women belonging to a higher socio-economic class staying in a joint family.31 A study was carried out in south-east Nigeria, where the psychiatric morbidity in leprosy patients was compared to albinism; the prevalence of specific psychiatric disorders among subjects with leprosy was depression (49%), generalised anxiety disorder (18%), and alcohol/drug abuse (16%). Over half (55%) of subjects with leprosy were general health questionnaire (GHQ) positive cases, while 41% with albinism were GHQ positive cases.32 Hansen’s disease complications can cause gross deformities of the face and limbs of infected individuals, as well as crippling disabilities involving sight, touch, and manual dexterity. Cumulative deformities add up to stigma, unemployment, and economic deprivation.33 In an Indian study evaluating the psychiatric morbidity among inmates of leprosy homes, it was found that 50% of subjects had very high distress as assessed by GHQ-12. Among them, 55.6% of subjects had a psychiatric disorder, the most common being dysthymia.34 There is a need for comprehensive psychiatric care for people with Hansen’s disease. The role of mental health professionals is also important in tackling psychosocial issues related to Hansen’s disease.
PSYCHIATRIC DISORDERS WITH SKIN SYMPTOMS
Psychiatric disorders with skin symptoms are conditions in which there is no primary skin condition. Rather, lesions that are observed on the skin are self-induced because the problem is psychological. Patients with these disorders are more frequently seen in dermatology clinics, as these patients may be unwilling to acknowledge a psychiatric basis for their physical findings.
Impulse Control Disorders
Trichotillomania
Trichotillomania (TTM) is characterised by recurrent and persistent urges to pull out one’s own hair. A survey of 2,524 college students about TTM demonstrated that the lifetime prevalence rate was 0.6%.35 The scalp is reported as the most common site affected, followed by the eyelashes, eyebrows, pubic hair, body hair, and facial hair.36 This self-inflicted hair-loss can range from small, barely noticeable patches on various areas of the body, to total baldness. Despite normal hair density, patients present with different hair lengths, including tapered ends, demonstrating new growth, and blunt ends, representing broken hairs.37 One important dermatological differential diagnosis is alopecia areata. In alopecia areata, the bare regions of the scalp are smooth, and the scalp is often peach coloured.38 Psychiatric comorbidities are known to be frequent in TTM and include major depression, generalised anxiety disorder, obsessive compulsive disorder (OCD), other anxiety disorders, eating disorders, and substance abuse.36 Treatment of TTM includes pharmacologic and non-pharmacologic therapies. Recommended first-line therapy for this psychiatric condition is administration of selective serotonin reuptake inhibitors (SSRI). N-acetylcysteine is also found to be effective for patients with TTM.39 Non-pharmacologic therapies include behaviour modification through habit reversal therapy, which has been shown to have the highest rate of resolution for TTM.38
Neurotic excoriation
Neurotic excoriations are self-inflicted lesions that typically present as weeping, crusted, or lichenified lesions with post-inflammatory hypopigmentation or hyperpigmentation.40 This is also known as pathologic skin picking or skin excoriation. The usual sites are the extensor aspects of extremities, scrotum, and perianal regions. It is estimated that 2% of dermatologic clinic patients have the diagnosis of neurotic excoriations.41 It predominantly affects women, with an age of onset between the third and fifth decade.42 Medical reasons for pruritus that can induce self-excoriation include urticaria, uraemia, hepatitis, xerosis, cutaneous dysesthesia, and malignancies. The diagnosis requires evaluation of the patient for impulse control disorders and ruling out relevant medical diseases. The first-line treatment for neurotic excoriations may be SSRI, as they can reduce depressive and compulsive symptoms.43
Body dysmorphic disorder
Body dysmorphic disorder (BDD) is a condition in which the patient is preoccupied and distressed with an imagined defect in appearance or an excessive concern over a trivial defect. The prevalence of BDD in many studies varies from 0.75%–12%.44 Most patients are females who have been affected in their 30s.44 The affected individuals frequently complain about disfigurement of the nose, ears, and sometimes of the breast, even though there is no objective evidence. This leads to anxiety, insecurity, and tension. In order to reduce anxiety, patients exhibit behaviours such as mirror checking or reassurance seeking.45 These patients visit cosmetologists or dermatologists for correction of defects. Among BDD patients, 10–14% present to dermatologists requesting cosmetic surgery.46 The management of these patients is challenging, as they have variable insight about their problems and are also resistant to accepting the psychological nature of their illness.
Obsessive compulsive disorders
OCD affects 2–3% of the general population. Up to 25% of patients presenting to physicians with skin disease suffer from OCD.47 In the current classification in the Diagnostic and Statistical Manual of Psychological Disorders (5th edition), obsessive compulsive and related disorders are noted to include OCD, BDD, pathological hoarding, and skin picking.48 Some of these conditions are already discussed previously. OCD is characterised by obsessive thoughts and compulsive behaviours. Studies have shown that 16% of all OCD patients have washing compulsions.49 There have been reports of AD irritant toxic dermatitis of the hands in patients with washing compulsions.47 Therefore, dermatologists seeing patients with hand dermatitis in the presence of compulsive washing should consider OCD in their diagnosis.45 These patients might take several years before coming to a psychiatrist, causing significant morbidity. Regarding the treatment of OCD, SSRI in combination with behavioural therapy is the standard treatment.
Delusional infestation
Delusional infestation is a condition where an individual has a firmly fixed, false belief that they are infested with an infectious agent, including infestation with non-living things such as nanobots or fibres. Delusional infestation is favoured over the narrower term delusional parasitosis;50 it can also be called Ekbom syndrome. The condition is more common in women in their 5th or 6th decade of life.51 As part of this belief, patients may perceive parasites crawling or burrowing into their skin. Discrete bruises, nodular pruritus, ulcers, and scars are frequently produced by patients trying to extract the parasite. They commonly seek the attention of dermatologists or physicians and may continue seeking different therapies in search of a cure. In fact, <90% of patients with this condition are seen by dermatologists.52 Patients affected by delusional infestations are difficult to treat as they have no insight into their illness. Management requires establishing a good therapeutic alliance and antipsychotics.
DERMATOLOGICAL ADVERSE EFFECTS OF PSYCHOTROPIC MEDICATIONS
Psychotropic medications from all classes have been associated with a broad variety of dermatologic reactions with variable rates of incidence. Psychiatrists should be aware of the potential cutaneous adverse effects of the medications they prescribe.
Mood Stabilisers
Lithium is one the most common medications used to treat mood disorders. It has been found to cause cutaneous side effects, such as acneiform eruption, psoriasis, folliculitis, and maculopapular eruption.53 It has been associated with both the onset and exacerbation of psoriasis.54 In controlled studies, patients treated with lithium developed more cutaneous reactions, particularly acne and psoriasis, with prevalence as high as 45%. Lamotrigine, another mood stabiliser, is an anticonvulsive medication and can cause an uncommon, but serious, rash called Stevens-Johnson syndrome.55 Stevens-Johnson syndrome has high mortality and morbidity and requires careful attention while using lamotrigine in clinical practice.
Antidepressants
Antidepressants can cause serious skin adverse effects, but these are rare in routine clinical practice. However, there are case reports of mianserin and bupropion causing erythema multiforme.56 Fluoxetine57 and sertraline58 have also been reported to cause Stevens-Johnson syndrome.
Antipsychotics
Antipsychotic agents are known to cause adverse cutaneous reactions in approximately 5% of individuals.59 In particular, chlorpromazine is known to induce skin pigmentation in areas exposed to sunlight.60 The prevalence of skin pigmentation with chlorpromazine in chronic, hospitalised patients is reported as 1.0–2.9%.61
CONCLUSION
There are significant psychosocial issues in dermatological conditions. Dermatologists are expected to consider quality of life issues along with social aspects, nature of disorder, efficacy, and tolerability of various therapeutic options to optimise the relief and comfort of their patients.62 There is a high prevalence of psychiatric disorders in patients attending dermatology clinics. Somatisation symptoms occur in dermatology patients, but pure disorders, without other comorbid psychiatric disorders, are rather infrequent. Understandably, persons with cutaneous somatic or bodily symptoms would approach a dermatologist first. Addressing the psychosocial issues is critical in the management and improvement of the quality of life for patients.63 Here are a few suggestions to achieve this:
- Dermatologists should enquire about psychological distress in the patients.
- Dermatologists should be aware of the psychological issues in common skin diseases.
- Minimum psychiatry training should be given during post-graduate training of dermatologists.
- Good referral systems between dermatology and psychiatry are necessary.
- Both psychiatrist and dermatologist should work together in collaboration, at least in difficult cases.