Abstract
Sebaceous carcinoma is a rare and aggressive malignant cutaneous cancer that arises from the sebaceous gland epithelium. This type of cancer typically presents in the periocular area and is rarely expressed in the extraocular space. The estimated overall incidence rate is one to two per million people per year. Sebaceous carcinoma tends to carry a delay in diagnosis as its variability in presentation of histologic growth patterns and diverse clinical presentation causes it to frequently be mistaken for common benign entities. Here, the authors report a case of a rare extraocular sebaceous carcinoma presenting on the cheek of a 78-year-old Caucasian male and discuss commonly mistaken differential diagnoses and the standard approach to properly diagnose and manage this rare tumour. Dermatologic literature has limited reference to sebaceous carcinoma, because this is rarely seen in an extraocular location, thus this case report provides a primary dermatologic perspective on this rare and aggressive skin cancer.
INTRODUCTION
Sebaceous carcinoma is a rare and very aggressive malignant skin cancer of the sebaceous gland. While sebaceous glands are present all over the body, this malignancy is most commonly diagnosed in the head and neck: areas rich in sebaceous glands.1,2 This type of cancer typically presents in the periocular region but can be expressed as an extraocular sebaceous carcinoma variant. The estimated incidence rate for sebaceous carcinoma is approximately one to two per million people per year, making it the third most common eyelid malignancy after basal cell carcinoma and squamous cell carcinoma.1 Peak incidence occurs in older individuals aged 60–79. Typically beginning as a painless papule on the skin, diagnosis and therapy of sebaceous carcinoma tend to be delayed as its myriad presentation of histologic growth patterns and diverse clinical presentations cause it to frequently be mistaken for common benign entities.3-5 Sebaceous carcinoma has been documented to have the ability to locally recur, as well as metastasise regionally and distantly.5 Most dermatologic literature focusses on the more commonly presenting skin cancers including basal cell carcinomas and squamous cell carcinomas with minimal acknowledgement of the rare sebaceous carcinoma. Presented here is a unique case of a patient with extraocular sebaceous carcinoma of the cheek and the diagnostic and treatment steps conducted. This report aims to increase clinical knowledge for this rare and aggressive skin cancer, and help to improve earlier and appropriate diagnosis.
CASE PRESENTATION
A 78-year-old Caucasian male presented to the dermatology clinic with concerns of a lesion on the right temple that initially appeared approximately 2 years prior. The patient’s pertinent medical history included hyperthyroidism, prostate cancer, and a prior cutaneous squamous cell carcinoma on the right temple treated with Mohs micrographic surgery 3 years earlier. The patient did not follow-up post-surgery for routine skin examinations. In addition to his right templar lesion, the patient noted lesions on the right ala and left cheek.
A focussed skin examination of the right temple displayed an erythematous papule with an overlying hyperkeratotic crust, a flesh-coloured pearly telangiectatic papule on the right alar, and a pearly telangiectatic papule with indurated margins on the left cheek. Additionally, a few scaly papules with an erythematous base were scattered throughout the face (Figure 1).
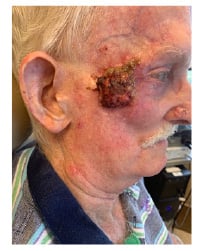
Figure 1: Sebaceous carcinoma of the right temple with cortical fixation to the zygoma.
Shave biopsies were performed on all three of the lesions of concern. On the right temple, biopsy showed atypical keratinocytes with many haematoxylin and eosin-stained cytoplasms emanating from underneath the epidermis and extending into the dermis, consistent with invasive squamous cell carcinoma. Histopathological examination of the right alar lesion demonstrated large, irregular aggregates of atypical basaloid epithelial cells with hyperchromatic nuclei, scant cytoplasm, and palisaded peripheral nuclei within the dermis, suggestive of nodular basal cell carcinoma. The shave biopsy performed on the left cheek revealed aggregations of immature sebocytes surrounded by sheets of atypical basaloid epithelial cells with increased mitotic figures emanating from the base of the epidermis and extending into the dermis, consistent with a well-differentiated sebaceous carcinoma. Immunostaining was negative for CEA and CK7.
The patient was initially considered for Mohs micrographic surgery to excise the three presenting skin cancers. However, upon further evaluation of the sebaceous carcinoma, MRI revealed cortical fixation to the zygoma. Consultation with the head and neck surgery department recommended urgent surgery to prevent further cortical invasion; however, the patient declined surgical options and opted to consider radiation therapy.
DISCUSSION
Sebaceous carcinoma is a rare malignant cutaneous tumour that mainly arises in areas abundant in sebaceous glands. Derived from adnexal epithelium of the dermis, this tumour may arise in periocular or extraocular sites. The periocular variant constitutes approximately 75% of sebaceous neoplasms.6 The upper eyelid tends to be affected two to three times more than the lower lid.6 Extraocular sebaceous carcinoma represents 25% of the sebaceous tumours and has been reported to present more commonly on the head and neck followed by the trunk, salivary glands, genitalia, breast, ear canal, and intraoral activity.6
This cancer typically affects the elderly, with a peak incidence in individuals aged 60–79. Additional risk factors for this cancer include male sex, ethnicity (Caucasian, Asian, and Indians), irradiation, ultraviolet exposure, pre-existing nevus sebaceous, Muir–Torre syndrome, and immunosuppression.7
The typical clinical presentation of sebaceous carcinoma is a painless localised papular or nodular subcutaneous growth.1,6 These lesions grow insidiously within the surface epithelium and can appear yellow in colour, attributable to the lipid accumulation.1 It can also present as pedunculated lesions, an irregular mass, or diffusely thickened skin.6 The varying appearance allows sebaceous carcinoma to mimic other benign tumours or inflammatory conditions. This is the primary reason for delay in proper diagnosis, inappropriate management, and increased morbidity and mortality.8
Differential diagnoses for ocular sebaceous carcinoma include chalazion, cysts, blepharitis, or other inflammatory conditions of the eye. Differential diagnoses for extraocular sebaceous carcinoma include pyogenic granuloma, molluscum contagiosum, and nonmelanoma skin cancers, including squamous cell carcinoma, basal cell carcinomas, or adnexal neoplasms.1,5 Because of their nonspecific appearance, extraocular sebaceous carcinomas are difficult to diagnose clinically and, most often, thought to be basal cell carcinomas prior to
histopathological examination.
The diagnosis of sebaceous carcinoma is established via incisional or partial-thickness biopsy. Scouting biopsies have been noted to be performed when a presenting lesion is severely inflamed. The morphological hallmark of sebaceous differentiation is the detection of sebaceous cells and demonstration of fat in vacuolated tumour cells. Common positive immunohistochemical markers include CK, EMA, CAM 5.2, and Anti-BCA-225 antibody.6 The current case displayed sebocytes in cells with sebaceous differentiation on histopathology.
Sebaceous carcinomas are known to have a significant association with Muir–Torre syndrome, a subset of hereditary nonpolyposis colorectal carcinoma.9 The primary internal malignancies associated with this syndrome are genitourinary (22%) and colorectal cancer (56%) as seen in this patient. Other malignancies such as endometrial, ovarian, and small bowel are also common.10 Although this patient declined further genetic testing, it is recommended for all patients for this autosomal dominant DNA mismatch repair disorder.9
Wide excision with clear margins is the treatment of choice for well-differentiated sebaceous carcinoma.6 In poorly differentiated lesions, wide excision, adjuvant radiotherapy, and regular follow-up of the skin and lymph nodes are advised.6 Although not the mainstay treatment, limited data of Mohs micrographic surgery has been reported to have lower recurrence rates as compared to wide excision.11 Although radiation therapy is more often used as an adjuvant therapy, a few small-scale studies have shown that primary treatment with radiation provides complete or near-complete response and favourable prognosis for eyelid carcinomas, with a five-year progression-free survival ranging from 57–93%, correlating with radiotherapy dosing.12,13 Information regarding radiotherapy for
extraocular carcinomas is limited to nonsurgical candidates, metastatic cases, and residual tumours.14 It is important to be aware of sebaceous carcinoma’s risk for recurrence and distant metastasis: more common in the ocular type as compared to the extraocular. Long-term follow up is recommended for patients after resolution of the cancer because of reports of late relapses.15
CONCLUSION
The authors presented this case to highlight sebaceous carcinoma, a rare skin cancer, that in recent years has had a significant increase in overall incidence.16 Exhibiting a variable presentation of histopathological and clinical presentations, this cancer is often misdiagnosed, delaying proper patient prognosis and care. Increasing awareness of this disease can help expand the differential diagnoses in patients who present with relevant features and prompt an early diagnostic and management plan.








