Author: Abigail Craig, EMJ, London, UK
Citation: Dermatol AMJ. 2024;1[1]:23-26. https://doi.org/10.33590/dermatolamj/PEOU2148.
![]()
ALOPECIA AREATA
Brittany Craiglow, Yale School of Medicine, started her session by describing alopecia areata (AA) as “traumatic,” and highlighted a patient who described how it “took a toll” on him mentally. To date, there have been five randomized control trials exploring both oral JAKi and topical JAKi, with promising results in the former, resulting in the FDA approval of baricitinib and ritlecitinib for patients with severe AA aged ≥18, and ≥12, respectively. Specifically, ritlecitinib helped 23% and 43% of patients achieve a Severity of Alopecia Tool (SALT) score of ≤20 at 24 and 48 weeks, respectively. Craiglow attributed some of this success to the high levels of patient adherence, despite the slow progress when treating AA. A 4 mg dose of barictinib, the first JAKi to be approved at two different doses, resulted in 35–39% of patients achieving a SALT score of ≤20 at 36 weeks, rising to 41% at 52 weeks. Craiglow also highlighted a new JAKi, deuruxolitinib, likely to be a twice-daily dose, that is demonstrating promising results in ongoing trials.
In her concluding remarks, Craiglow explained that patients with less severe AA respond significantly better than those with a more severe disease. It is therefore important to consider dose, baseline severity, and the duration of the current episode, as these influence the response to treatment.
LUPUS, DERMATOMYOSITIS, AND STING-ASSOCIATED VASCULOPATHY
Tofacitinib was approved in 2012 for the treatment of rheumatoid arthritis. Ruth Vleugels, Brigham and Women’s Hospital, Boston, Massachusetts, USA, presented the case of a young patient with myositis treated with 10 mg tofacitinib twice daily, who responded “beautifully” 10 years ago. Since then, several cases of severe dermatomyositis have been successfully treated with this JAKi. This presented the question as to why JAKi improve dermatomyositis. Vleugels explained that there is a strong interferon (IFN) signature driven by IFN-β in serious cases of myositis, but a low signature in patients with mild disease. Thus, JAKi can aid the alleviation of the interferon signal. Subsequently, dazukibart, an immunoglobulin G neutralizing monoclonal antibody directed against IFN-β, is currently enrolling for a Phase III global trial after achieving a Cutaneous Dermatomyositis Disease Area and Severity Index (CDASI) reduction of >5 points in 100%, and 96% of patients receiving 150 mg and 600 mg, respectively.
SARCOIDOSIS AND GRANULOMA ANNULARE
Sarcoidosis is considered a T cell-dependent disorder, with macrophages and myeloid cells playing significant roles in pathogenesis. Granuloma annulare (GA) shares similarities with sarcoidosis, but is clinically and histologically distinguishable. William Damsky, Yale School of Medicine, summarized the promise JAKi have in treating these conditions during his talk in this session. Specifically, data from open-label studies and clinical trials using tofacitinib in patients with GA and sarcoidosis, respectively, demonstrated marked improvements in the conditions, and a reduction in inflammation.
PET scans, performed on patients with sarcoidosis prior to commencing treatment, permitted the assessment of the internal organs, and confirmed metabolic responses. Damsky stressed that not only did patients get better, but they were also able to taper off other medications, such as prednisone. Further molecular studies suggest IFN-γ is a key mediator in sarcoidosis pathogenesis, explaining the efficacy of JAKi. Specifically, the production of TNF-α, an inflammatory cytokine, occurs downstream of IFN-γ, a JAK STAT-dependent cytokine, thus controlling its production.
Regarding GA, molecular studies indicate the importance of IFN-γ, but also currently unknown secondary cytokines, possibly requiring broader therapeutic approaches. At present, there are no FDA approved treatments for GA, and Damsky stressed that with the exception of TNF inhibitors, current therapies are generally ineffective. Phase I studies with tofacitinib gel in GA have been conducted, with the aim for larger controlled studies to establish efficacy conclusively.
VITILIGO
Khaled Ezzedine, Greater Paris University Hospitals, France, spotlighted the use of JAKi for the treatment of vitiligo, a skin condition characterized by loss of skin color. The rationale for using JAKi in vitiligo treatment stems from their role in the JAK1 and JAK2 pathway, which is implicated in the pathogenesis of the disease.
Topical JAKi have shown promise in treating vitiligo, with studies demonstrating improvement in skin pigmentation. A Phase III study involving topical ruxolitinib showed significant improvement in repigmentation of vitiligo lesions, with sustained effects even after treatment cessation. Specifically, at Week 52, the Facial Vitiligo Area Scoring Index (F-VASI75) was achieved by a greater percentage (52%) of patients applying ruxolitinib cream compared to a vehicle. However, safety concerns with topical JAKi include application site acne-like lesions, which can be bothersome to the patient, especially in visible areas. The recent addition of narrowband UVB phototherapy to topical JAKi treatment has shown to enhance repigmentation, though careful consideration of immunosuppression risks is warranted.
Four oral JAKi have also been explored in vitiligo treatment, with several drugs undergoing Phase II studies. Ritlecitinib specifically met key secondary endpoints when administered as a 50 mg daily dose, with or without an induction. Future challenges in vitiligo treatment include determining optimal dosing regimens, identifying maintenance strategies to prevent relapse, and addressing safety concerns associated with systemic JAKi therapy.
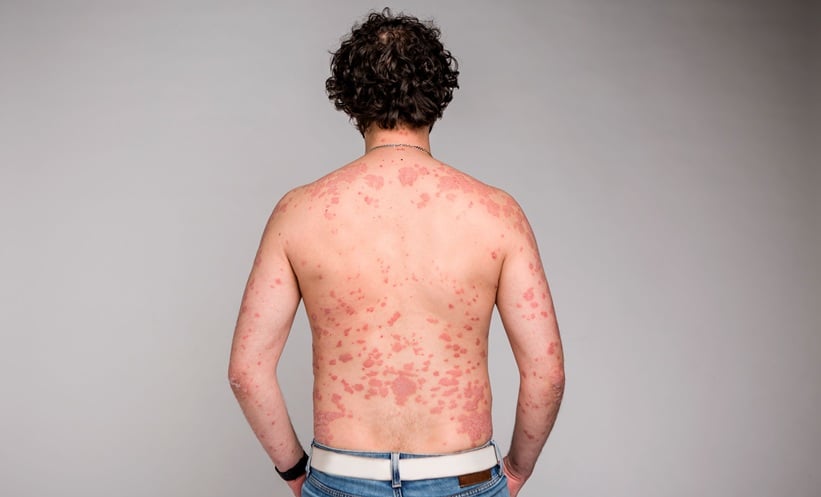
PSORIASIS
JAKi are a significant topic in psoriasis treatment, stressed Melinda Gooderham, SKiN Health, Peterborough, Ontario, Canada, who summarized the mechanism of action of JAKi, and their relevance to psoriasis treatment, during her talk.
Competitive inhibitors, which bind at the kinase domain, were initially explored, with tofacitinib being one of the first studied for plaque psoriasis, followed by trials of baricitinib and tofacitinib for psoriasis and psoriatic arthritis. While tofacitinib showed promising efficacy, it was not approved for plaque psoriasis, due to safety concerns and a narrow therapeutic index. Newer approaches shifted focus to allosteric inhibition, where drugs like deucravacitinib target the pseudokinase domain, allowing ATP-binding to proceed, maintaining normal JAK function. Deucravacitinib, a tyrosine kinase 2 inhibitor, has shown significant efficacy in plaque psoriasis, with 50% of patients achieving Psoriasis Area and Severity Index (PASI) 90, maintained for up to 3 years with a good safety profile.
Safety concerns with JAKi include risks such as venous thromboembolism and major adverse cardiovascular events, but the allosteric inhibition mechanism offers a better safety profile by allowing normal JAK function. In summary, JAKi, particularly deucravacitinib, offer a valuable treatment option for patients with psoriasis, providing efficacy comparable to biologics, with a different safety profile. Gooderham suggests considering JAKi as an option, especially for patients who prefer oral medication, or have specific comorbidities, like psoriatic arthritis or palmoplantar psoriasis. Future research and ongoing trials aim to explore the efficacy of JAKi in other conditions, like hidradenitis suppurativa and palmoplantar psoriasis, expanding their potential therapeutic use.
CONCLUSION
Further topics discussed in this fascinating session include JAKi for the treatment of lichen planus, hidradenitis suppurativa, pyoderma, atopic dermatitis, and prurigo nodularis. King concluded the session by considering the safety profile of JAKi, emphasizing the need to balance the risks of adverse events with the suffering of patients with skin diseases. Delving into data comparing safety profiles across different diseases, King cautioned against overreliance on theoretical selectivity data, and advocated for decisions based on efficacy and safety data, despite the “unmatched ability” of this class of medicines in addressing inflammatory skin diseases.