Abstract
Tropical diabetic hand syndrome (TDHS) is an acute complication that mainly affects patients with diabetes living in the tropics. The cause is usually unknown, but it is often preceded by minor trauma to the hand. Other risk factors for TDHS are poor glycaemic control, poorly treated wounds, malnutrition, and diabetic neuropathy. Early signs include swelling and ulceration of the hand. It can rapidly progress to sepsis and may further worsen, leading to deformity, disability, and amputation. If not treated promptly, death may occur. Unlike diabetic foot ulcer, TDHS often goes unreported. Here is a case of a 39-year-old female and a known patient with diabetes who presented to the outpatient department with swelling and tenderness of the left hand, along with foul-smelling purulent discharge. It began after the patient peeled off a patch of scaly, thickened skin over the distal part of their middle finger. Investigations showed high blood sugar and slightly increased leukocyte count. The patient was started on antihyperglycaemic medications and intravenous antibiotics. Urgent surgical debridement was done, which led to amputation of the middle finger. Thereafter, the patient showed significant improvement and was discharged with follow-up instructions. This case report emphasises the importance of timely intervention in cases of tropical diabetic hand syndrome, and the need for adequate patient education on this issue.
Key Points
1. Tropical diabetic hand syndrome, which manifests in swelling and ulceration of the hand and can lead to deformity, disability, amputation, and death, mainly affects patients with diabetes living inthe tropics.
2. Treatment includes antihyperglycaemic medications, antibiotics, and surgical debridement.
3. Timely intervention and adequate patient education are imperative to treat this condition, and measures to increase awareness of the condition should be taken.
INTRODUCTION
Diabetes is a public health burden and a leading cause of morbidity and mortality globally.1 Microvascular and macrovascular complications of diabetes include retinopathy, nephropathy, neuropathy, cardiovascular disease, and diabetic foot syndrome. Diabetes constitutes an important cause of ischaemic heart disease, stroke, end-stage renal disease, blindness, and nontraumatic limb amputations.2 A less frequently reported complication, prevalent in the tropics, is tropical diabetic hand syndrome (TDHS). TDHS is characterised by variable hand symptoms ranging from a localised cellulitis, ulcer, or abscess, to a rapidly progressive gangrene and attendant overwhelming sepsis, which may result in permanent disability and fatality.3,4 Poor glycaemic control, poor nutrition, peripheral neuropathy, and low socioeconomic status are major risk factors contributing to the development of TDHS, usually in the setting of a preceding minor hand trauma.4,5 Management of TDHS involves broad-spectrum antibiotic therapy as well as surgical interventions, including incision and drainage of wounds, debridement, amputation, and rehabilitation of the affected limb.4-6 Lack of awareness about this condition and poor health-seeking behaviours in the low-resource settings pose a challenge, and contribute to increased risks of morbidity and mortality. Hence, proper education of patients about this syndrome and its precipitating factors, early recognition and presentation, and prompt management of TDHS is of the utmost importance. Below is a more detailed outline of notable risk factors, proposed classification, and treatment options pertaining to TDHS.
Common identifiable risk factors include poor glycaemic control; low socioeconomic status and limited access to healthcare; hand trauma, including minor trauma; poor hand care; neglect or inadequately treated hand wounds; lack of patient education on the subject matter and the need to seek urgent care when need arises; lack of proper follow-up at office visits for regular evaluation; and peripheral neuropathy.
According to the proposed Lawal classification, Grade I TDHS is characterised by infections involving the skin, subcutaneous tissue, muscular layer, and metacarpal web spaces; Grade II TDHS involves infections extending to deeper tendons, bones, and joints without gangrene of the affected hand; and Grade III TDHS is associated with infections extending down to deeper structures with gangrenous elements noted.
The recommended treatment strategy includes adequate glycaemic control; early initiation of broad-spectrum antibiotics and subsequent adjustment based on culture and sensitivity results when necessary; and urgent surgical debridement with or without amputation (if need arises) and aggressive wound care.
It is pertinent to note that lack of patient education on the subject matter, late presentation for care, delay in initiation of broad-spectrum antibiotics (preferably intravenous antibiotics), poor glycaemic control, and inadequate wound care can significantly affect the patient’s prognosis.5-8
CASE PRESENTATION
A 39-year-old African female presented to the medical outpatient department with complaints of progressive left hand swelling with continuous discharge of pus from the base of the index finger, which began 10 days prior to presentation. The patient had noticed scaly and thickened skin over the distal phalanges of the left middle finger, which was peeled off by the patient. The lesion became pustular, erythematous, and painful, with discharge of purulent fluid from the primary site. The swelling and erythema extended over the full length of the left middle finger and up to the distal forearm, with a blister noted over the dorsum of the patient’s left hand. Prior to the hospital visit, the patient resorted to herbal treatment with the application of vegetable-based herbs. The patient also presented to a traditional practitioner who aspirated pus from the lesions using a syringe. Fever was noticed a day before the presentation. No history of numbness in the upper or lower extremities was reported. A 2-year history of Type 2 diabetes with poor compliance to oral antihyperglycaemic medications was stated at presentation. There was no history of hypertension or other medical comorbidities. No family history of diabetes was reported, and the patient had no previous history of smoking or alcohol use.
Physical examination revealed an acutely ill-looking patient, febrile (100.8 °F), with a BMI of 18.5 kg/m², not pale or dehydrated. Blood pressure at presentation was 130/70 mmHg. The left hand was swollen, warm, fluctuant, and tender. There were areas of ulceration over the dorsum of the hand, also involving the middle finger (Figure 1). Copious discharge of foul-smelling purulent fluid from multiple sites and surrounding tissue cellulitis were also noted. Sensations were preserved in both extremities. The radial and brachial pulses were palpated with normal intensity on both upper limbs.
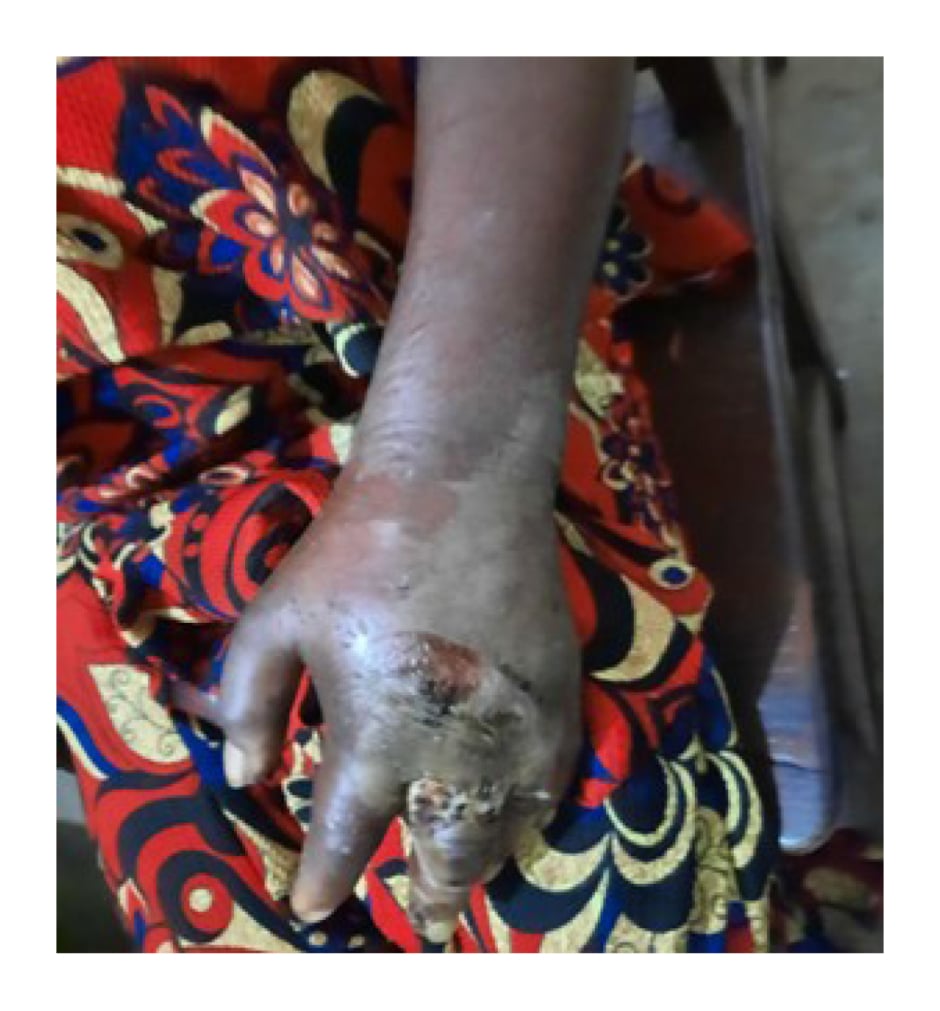
Figure 1: Tropical diabetic hand syndrome at presentation.
Investigations carried out at admission included random blood glucose of 13.3 mmol/L, full blood count with haemoglobin of 12 g/dL, and a high normal leukocyte count of 11.9×10⁹ cells/L. The patient was placed on intravenous antibiotics, analgesics, antioxidants, as well as oral antihyperglyacemic medications, including metformin and glimepiride at presentation. Intravenous ciprofloxacin, metronidazole, and ceftriaxone plus sulbactam were commenced empirically while awaiting the wound swab culture and sensitivity result. The wound swab culture and sensitivity yielded Escherichia coli, which was sensitive to ciprofloxacin, ofloxacin, gentamicin, and chloramphenicol. X-ray of the affected limb revealed no findings suggestive of bone involvement (Figure 2). The patient was counselled on the need for urgent surgical debridement. Surgical debridement was done on the sixth day of admission. Intraoperative findings revealed significant gangrene of the soft tissues of the left middle finger extending into deeper structures with copious purulent effluence. This prompted the amputation of the middle finger. Thereafter, daily wound dressing was done. Intravenous antibiotics were continued postoperatively with other medications including analgesics, oral vitamins, and antihyperglycaemic agents. Significant wound healing was noted postoperatively (Figure 3). Daily fasting blood sugar was done to monitor sugar control. Subsequently, intravenous antibiotics were switched to oral cefixime and flagyl. The dosage of oral antihyperglycaemic agents was adjusted in order to achieve adequate sugar control. The patient was discharged 4 weeks after surgery and asked to return for alternate day wound dressing on an outpatient basis. The patient was strongly counselled on the need to adhere to prescribed medications and comply with follow-up visits.
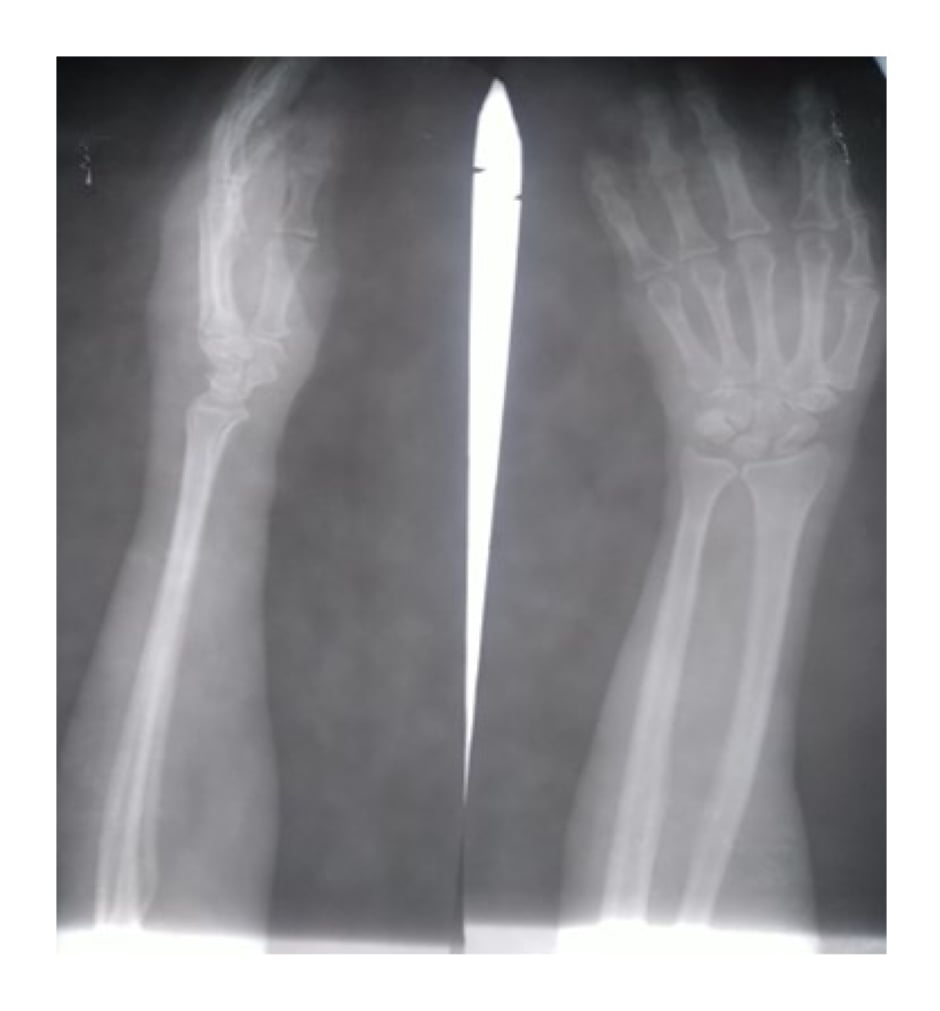
Figure 2: X-ray of the affected limb (left forearm and hand) with no bone involvement.
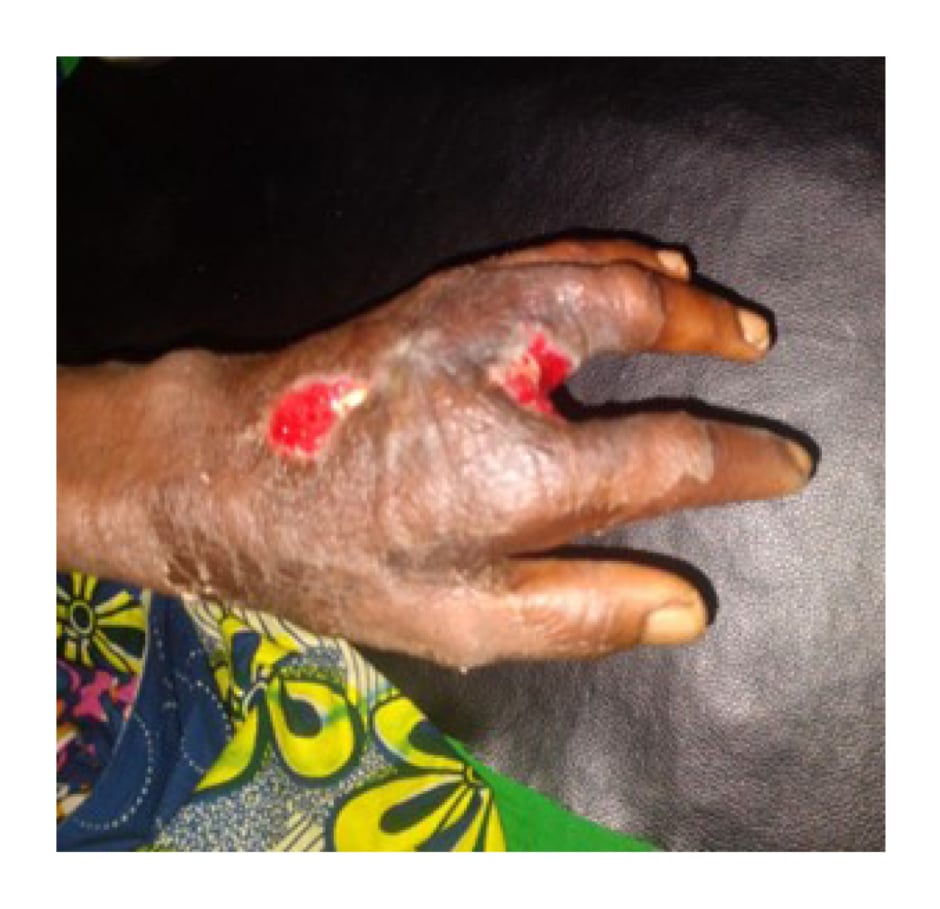
Figure 3: Wound condition 2 weeks after surgical intervention.
DISCUSSION
TDHS is a rare but debilitating cause of morbidity, hospital admissions, and mortality amongst patients with diabetes, especially for patients in the tropics.7,8 Compared with diabetic foot infection, TDHS seems to be less prevalent.7-9 Some notable risk factors for TDHS include trauma, poor glycaemic control, and malnutrition.7-9 Complications can range from sepsis, limb deformity, amputation, and death.7-9 Therefore, the authors strongly feel that timing of presentation and intervention strongly affects the prognosis of patients with this condition. Some causes for delayed presentation include downplay of disease severity by patients; limited healthcare access; socioeconomic factors (in low- and middle-income countries); and improper health-seeking behaviours, such as initially resorting to traditional healers.8,9 In some studies, improper health-seeking behaviour was found to correlate with low-income earners, poor education, rural dwelling, and lack of health insurance.8-11 As in this case, the patient had initially attempted self-care by applying herbal mixtures to the wound, and subsequently visited a traditional healer who aspirated a purulent effluence from the wound site under questionable sanitary conditions. Likewise, due to the patient’s poor financial state and lack of insurance coverage, certain pertinent investigations such as lipid profile, extremity doppler ultrasound, serum electrolyte, urea, and creatinine tests could not be carried out while the patient was admitted. Early diagnosis and immediate treatment of TDHS favours better outcomes, as shown in several reports.8-11 It is important to carry out prompt surgical debridement when necessary to prevent promulgation of soft tissue infection and gangrene. Studies have shown that timely glycaemic control, antibiotic therapy, adequate wound care, and aggressive surgical intervention reduces morbidity and mortality associated with TDHS.8-11 There is a need to create better awareness of the potential severity of TDHS for patients and health workers, as well as to make available a well-structured health insurance system with adequate health coverage for patients, especially in low- and middle-income countries, or for patients of low socioeconomic status. Such incentives would help to shorten the interval between appearance of symptoms and presentation to the hospital, which may ultimately improve medical outcomes for patients with these conditions.
CONCLUSION
From the in-depth analysis of this case and recently published reports, it is evident that prompt presentation for appropriate care, adequate sugar control, urgent medical and surgical intervention, as well as proper wound care is highly recommended for patients with TDHS. It is imperative that patients with diabetes should be counselled and duly educated by their healthcare providers on precautionary measures to take to prevent this condition. Patients with diabetes should also be encouraged to adhere to their medications and follow-up visits, as this may help to prevent and quickly identify such complications. As diabetes is a disease of public health significance, measures should be taken to increase awareness of TDHS among the general population, which would further aid early recognition and presentation to the hospital, and reduce overall morbidity and mortality. The authors encourage more research on this topic to add to the available body of data, to further broaden the knowledge on this condition, and positively influence management practices.