BACKGROUND AND AIMS
Patients with haematologic malignancies appear to have a greater risk of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection and severe disease due to myelosuppression.1-3 Furthermore, delays in treatment of patients with haematologic malignancies, especially those with acute leukaemia planned for chemotherapy or transplantation, are associated with a risk of disease progression. To date, some societies recommend that chemotherapy should generally not be started until COVID-19 symptoms have completely resolved and viral testing becomes negative. However, implications of the aforementioned recommendations remain uncertain in routine clinical practice, and data on COVID-19 in patients with haematologic malignancies are still limited.
MATERIALS AND METHODS
From February 2020 to February 2021, there was a total of 310 hospitalisations, where 163 adult patients were admitted to the authors’ centre for treatment of haematologic malignancies. The indication for admission was acute myeloid leukaemia (AML) in 50 (30%) patients, acute lymphoblastic leukaemia in 14 (8%), lymphoma in 54 (33%), myeloma in 14 (8%), and 31 (19%) as other.
Diagnosis of SARS-CoV-2 infection was based on virus detection by real-time polymerase chain reaction (SARS-CoV-2 E-gene RT-PCR) in respiratory tract specimens. Standard preventive measures for SARS-CoV-2 infection control were applied to the care of all patients, in accordance with national disease control and prevention guidelines.
RESULTS
Ten (6%) patients tested positive for SARS-CoV-2 via PCR in a unique COVID-19 outbreak during hospitalisation stay, and they were immediately transferred to the COVID Infectious Unit. All of these patients were affected by acute leukaemia (eight patients with AML; two patients with acute lymphoblastic leukaemia, Philadelphia chromosome-negative). Most patients were at the peak of cytopenia at the time of their COVID-19 infection. Nine patients had been treated with intensive chemotherapy before SARS-CoV-2 confirmation.
At SARS-CoV-2 diagnosis, one patient had untreated, newly diagnosed AML while three patients had refractory/relapsed AML. One patient was in complete remission with incomplete haematologic recovery. Deep vein thrombosis complicated by pulmonary embolism and interstitial pneumonia was observed in a patient despite anticoagulation and thrombocytopenia. After SARS-CoV-2 infection, no leukaemia-specific treatment was adjusted.
Three patients (30%) died due to severe acute respiratory distress syndrome despite extracorporeal membrane oxygenation in deep aplasia; all of these patients had refractory disease. Seven patients were delayed in receiving chemotherapy treatment for 34 days; chemotherapy started once COVID-19 symptoms had been completely resolved and two viral tests became negative. These patients maintained their complete remission and remained negative for SARS-CoV-2. One patient underwent bone marrow transplantation.
CONCLUSION
The authors’ findings support the vulnerability of patients with haematologic malignancies in the COVID-19 pandemic, and reported a high COVID-19 infection mortality of 30%, in accordance with other haematological case series. However, deaths owing to COVID-19 were observed in patients with leukaemia disease progression. Furthermore, the patients who recovered from COVID-19 in leukaemia remained negative for SARS-CoV-2 after delivery of chemotherapy and underwent their following chemotherapy and allogeneic bone marrow transplantation programme without any other complications.
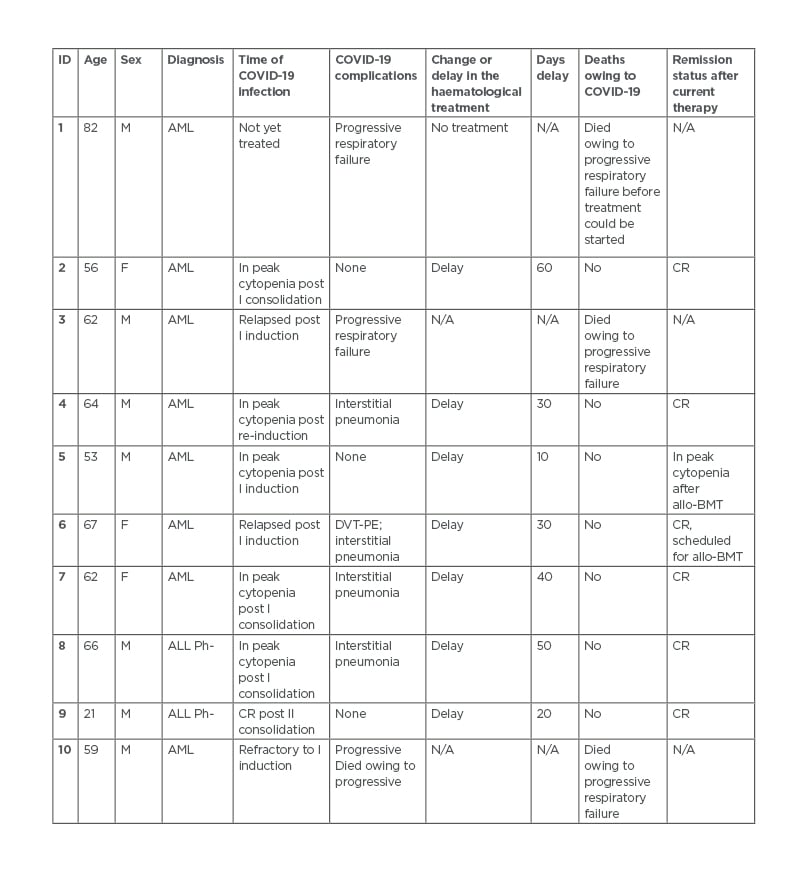
Table 1: Overview of patient characteristics.
Allo-BMT: allogeneic bone marrow transplant; ALL-Ph: acute lymphoblastic leukaemia Philadelphia (negative/positive); AML: acute myeloid leukaemia; CR: complete remission; DVT-PE: deep vein thrombosis-pulmonary embolism; F: female; M; male; N/A: not applicable.







