BACKGROUND AND AIMS
Patient blood management encompasses all aspects of the transfusion decision-making process, beginning with the initial patient evaluation and continuing through clinical management.1 It involves the timely, multidisciplinary application of evidence-based medical and surgical concepts, aimed at diagnosing and appropriately treating anaemia, along with minimising surgical and iatrogenic blood losses and managing coagulopathic bleeding, as well as supporting the patient while appropriate treatment is initiated.1
Haemovigilance is the set of surveillance procedures covering the entire blood transfusion chain, from the donation and processing of blood and its components, through to their provision and transfusion to patients, including their follow-up.2
The restrictive transfusion threshold uses a lower haemoglobin concentration as a threshold for transfusion (most commonly 7–8 g/dL), and the liberal transfusion threshold uses a higher haemoglobin concentration as a threshold for transfusion (most commonly 9–10 g/dL).3
MATERIALS AND METHODS
In this retrospective analysis, the authors aimed to critique and study their own performance since the establishment of the Regional Blood Centre (RBC) Karachi (2020–2022), Pakistan, and its associated hospital-based blood banks (currently three).
The authors calculated parameters, including cross match to transfusion ratio and transfusion index; introduced the concept of maximum surgical blood ordering schedule; assessed the cold chain maintenance through data loggers and transportation containers; reported transfusion reactions; and overviewed the overall haemovigiliance concept over 3 years’ time.
RESULTS
When the authors started their blood banking in government sector hospitals of Karachi, whole blood was being issued to the patients. From the first day, RBC Karachi worked on blood products and did not issue a single whole blood to any patient. Initially, the cross match to transfusion ratio was 15:1, but with time and management, at the end of third year, they achieved the ratio of 1.5–1.7:1 for different hospitals (Figure 1). Transfusion index was also calculated to be 0.2 at the start of 2020 and was reported to be 0.8 at the end of 2022.
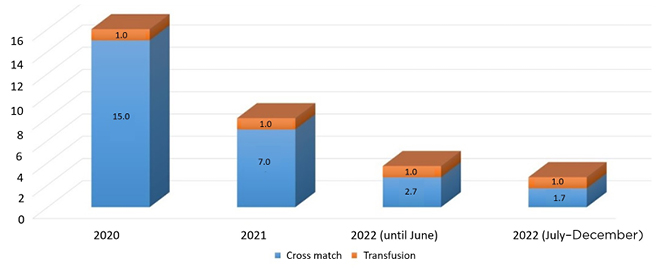
Figure 1: Graphical representation of cross match to transfusion ratio of red blood cells and its associated blood banks.
CONCLUSION
Initially, for 1.5 years, the authors were not able to get a single transfusion reaction reported; however, after several awareness and training sessions, and continuing medical education, they started getting transfusion reactions reporting around 2–3 times fortnightly. Initially, wastage was higher than utilisation; however, with hard work and communication, the authors were able to reduce the wastage and suggested the idea of a restrictive transfusion strategy, so that the right blood component is given to the right patient at the right time. It was a tough journey as there are, unfortunately, no haematologic units in the government sector hospitals, and dealing with doctors along with patients was not easy.
The authors’ aim is to provide the best transfusion services to those who cannot afford it and their journey is still ongoing.






