In patients with myeloproliferative neoplasms (MPN), including essential thrombocytosis (ET), polycythaemia vera (PV), and myelofibrosis (MF), symptoms may be diverse and debilitating. Pharmacological intervention, such as with janus kinase (JAK) inhibitor therapy, results in only partial amelioration of MPN-associated symptom burden. Patients and providers are often dissatisfied with unmet patient needs and limited therapeutic options.
Integrative medicine, defined as the use of evidence-based complementary and alternative medicine in conjunction with standard-of-care medicine, is an emerging field. In recent reports, ≤40% of cancer patients utilise integrative medicine. However, the usage patterns and potential impact of integrative medicine on MPN patients are unknown.
In the SIMM study, we investigated the utilisation preferences and symptom burden association of 858 MPN patients (338 ET, 315 PV, 188 MF, and 17 MPN not otherwise specified). Patients were recruited internationally by means of social media. Informed consent and online self-report surveys (via Qualtrics, Provo, Utah and Seattle, Washington, USA) were completed capturing patient demographics, disease-specific data, supportive care utilisation, MPN symptom burden via MPN Assessment Form Total Symptom Score, depression via Patient Health Questionnaire (PHQ)-2, fatigue via Brief Fatigue Inventory Usual, and an overall quality of life (QoL) single question assessment. ANOVA, chi-squared tests, and Wilcoxon rank sum tests methods were then applied.
We found the most common integrative interventions utilised by MPN patients included aerobic activity (n=442), massage (n=244), yoga (n=220), nutrition (n=216), strength training (n=204), acupuncture (n=166), meditation (n=163), breathing exercises (n=158), chiropractic (n=139), and support groups (n=124). Overall, patients had fewer MPN-related symptoms when participating in aerobic activity (p<0.001), massage (p<0.001), yoga (p=0.02), strength training (p<0.001), breathing exercises (p<0.001), and support groups (0.001). QoL was higher with aerobic activity (p<0.001), massage (p=0.02), yoga (p=0.02), strength training (p<0.001), breathing exercises (p=0.01), and support groups (p=0.001). Depression (PHQ-2 total >3 category) was lower in aerobic activity (p=0.001), yoga (p=0.001), strength training (p=0.001), and meditation groups (p=0.2). Fatigue was lower in aerobic activity (p<0.001), massage (p=0.04), strength training (p<0.001), breathing exercises (p<0.001), and support groups (p=0.001). In subgroup analysis, ET and PV patients had lower symptom burden (MPN assessment form total symptom score) with aerobic activity (p<0.001, <0.001, respectively), massage (p=0.01, 0.02, respectively), and strength training (p=0.03, 0.02, respectively). Support groups were found to be associated with lower symptoms in ET patients (p=0.03). In MF, breathing exercises (p<0.001) and support groups (p=0.03) were associated with lower symptom burden (Table 1).
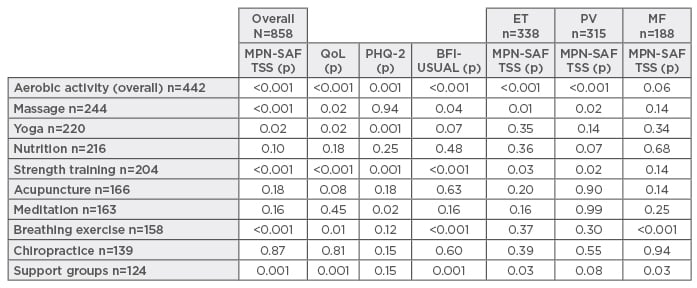
Table 1: The SIMM study: Survey of integrative medicine in myeloproliferative neoplasms results.
MPN-AF TSS: myeloproliferative neoplasm assessment form total symptom score; QoL: quality of life;
PHQ-2: Patient Health Questionnaire-2; BFI-USUAL: Brief Fatigue Inventory Usual; ET: essential
thrombocytosis; PV: polycythaemia vera; MF: myelofibrosis.
In this study, we demonstrated that integrative medicine interventions are associated with fewer MPN-related symptoms, reduced depression and fatigue, and higher QoL. Interestingly, unique patterns were observed within MPN subtypes and may represent unique supportive care needs. Future studies are needed to assess the impact of integrative medicine interventions on MPN patients. Ongoing efforts to meet the needs of MPN patients include a randomised controlled trial of an online-streamed yoga intervention, a multicentre nutritional intervention study, and an acceptance and commitment therapy pilot trial. We continue to seek non-pharmacological treatment approaches that may complement medical therapy and enhance MPN patients’ QoL.







