BACKGROUND AND AIMS
Percutaneous coronary intervention of bifurcation lesions accounts for approximately 20% of intervention,1,2 and leads to higher risk of restenosis, thrombosis, and recurrent adverse clinical events.1-4 The mismatch between the proximal and the distal landing zone constitutes the major anatomical challenge and interventions in left anterior descending artery (LAD) ostial lesions remain defiant.3 A left main (LM) to LAD crossover stenting provides favourable outcomes, but challenges current devices.1 There is a need for comparative, independent data on the performance of currently available stents. In clinical practice, wide anatomical variation impairs such studies. However, 3D-printing allows accurate anatomical reproduction that can be used in simulation testing.5,6 The aim was to assess stent performance in 3D-printed diseased LM bifurcation model (Medina classification 0,1,0) using a realistic simulation environment.
MATERIALS AND METHODS
A standard realistic LM anatomy with an eccentric ostial LAD lesion was replicated using 3D-printing (Figure 1A). Tests were performed on a realistic pulsatile flow simulator in the catheterisation laboratory (Figure 1B). Five 3.5 mm x 18–21 mm stents (XIENCE [Abbott, Abbott Park, Illinois, USA]; Onyx [Medtronic, Minneapolis, Minnesota, USA]; SYNERGY™ [Boston Scientific, Marlborough, Massachusetts, USA]; SYNERGY MEGATRON™ [Boston Scientific]; and Ultimaster [Terumo Corporation, Tokyo, Japan]) were implanted in 3D-printed models using a standardised protocol (Figure 1C) that included proximal optimisation technique (POT). Angiographic and optimal coherence tomography (OCT [Abbott]) runs were acquired at each procedural step, and images were blindly reviewed and analysed offline. The authors report descriptive and comparative data of stent platform performance with a focus on stent placement accuracy, longitudinal deformation, over-expansion ability, and radial strength.
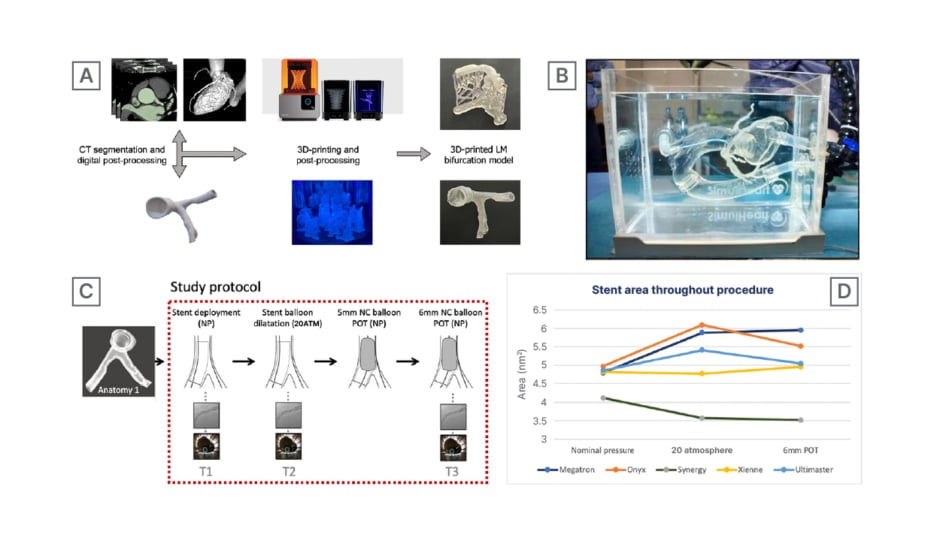
Figure 1: Study workflow and protocol.
A) Workflow of simulated interventional and intravascular imaging procedure. The 3D-printed LM anatomies;
B) the 3D-printed LM anatomies were connected to SimulHeart interventional cardiology Simulator;
C) study protocol – provisional stenting; D) stent area throughout the procedure.
RESULTS
In total, five test procedures were performed, and a total of 15 OCT runs and 20 angiographic images were reviewed. Stent placement accuracy, defined as balloon marks to stent distance in angio, was highest with XIENCE (0.27 mm) and lowest with SYNERGY™ (1.01 mm). Proximal overexpansion ability after sequential 5 mm and 6 mm POT was also highest with XIENCE (stent area: 26.99 mm2), and lowest with SYNERGY™ (stent area: 15.58 mm2). Regarding longitudinal deformation, OCT analysis revealed shortening of Onyx (-0.1 mm), SYNERGY MEGATRON™ (-0.4 mm), and Ultimaster (-0.7 mm) stents, and elongation of SYNERGY™ (1.4 mm) and XIENCE (+3.8 mm) after POT. In angio, there was elongation of XIENCE (+3.5 mm) and shortening of all other stents (-0.9 mm to -3.5 mm). Radial strength was highest with Onyx (minimal liminal area: 4.99 mm2) and lowest with SYNERGY™ (4.12 mm2). Considering eccentricity, Ultimaster achieved the lowest (0.92) and Onyx the highest (0.84). High pressure balloon inflation increased minimal liminal area in all stents except SYNERGY™ and XIENCE (Figure 1D). POT negatively impacted stent performance at the LAD ostial lesion in two of the stents that showed recoil. There was no significant correlation of proximal stent expansion and stent strut thickness (r: 0.296; p=0.629).
CONCLUSION
In this study of percutaneous coronary intervention in 3D-printed realistic models of left main bifurcation coronary artery disease, the authors have shown that stent performance is not uniform among available stents. Knowledge of strengths and weaknesses of each individual stent allows a tailored approach to bifurcation stenting in order to anticipate and optimise results.








