INTRODUCTION
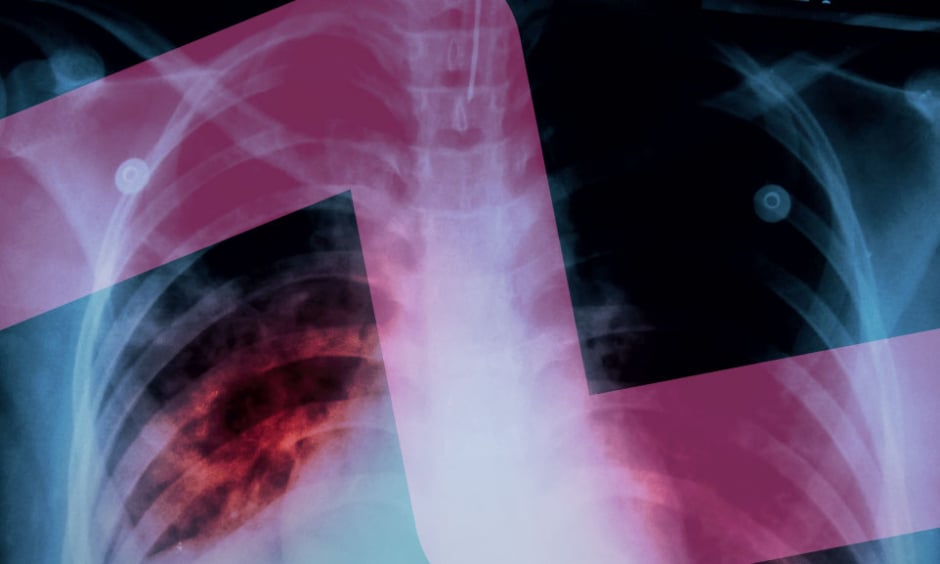
Drug resistance among patients with tuberculosis (TB) is an emergent topic that requires intervention. According to a survey of TB drug resistance in India,1 resistance to any fluoroquinolones (FQ) reported in cases of multidrug resistance (MDR) to TB was 21.82%. On the other hand, in a developing country like India, amongst the commonest causes of pyrexia of unknown origin, TB and typhoid fever are two important differentials, and it is a standard practice to order a Widal test when evaluating fever, especially at the primary health centre. The Widal test has very low specificity and sensitivity, and is confusing and difficult to interpret when diagnosing typhoid fever because cross agglutinating antibodies remain from previous infection with related Salmonella serotypes, which give a false-positive result. There are equal chances of getting false-positive results for the Widal test in non-typhoid infectious fever and in healthy individuals.2 In typhoid-endemic areas, it has been demonstrated that a number of illnesses caused by non-Salmonella organisms (such as malaria, dengue, miliary TB, endocarditis, chronic liver disease, brucellosis, etc.) exhibit this cross-reactivity, and this increases the error rate of the Widal test result.3
DISCUSSION
In a cohort study by Roberts et al.,4 it was found that the most common cause of delay in initiating TB treatment was a delay in making the decision to refer a patient to TB specialists, with a median delay of around 88 days. In fact, evidence suggests that each infectious case of TB in areas with a high frequency of the disease can cause up to 20 secondary infections before being discovered.5
Here, the authors discuss one cause for the same scenario (i.e., a false-positive interpretation of a Widal test). To date, there is no consensus concerning diagnostic criteria for interpreting the test. Serological diagnosis classically relies on the demonstration of a rising titre of antibodies in paired samples that are 10–14 days apart, which is usually not demonstrable in most blood culture-positive typhoid cases.6
As initial titres in endemic areas such as India may be higher than anticipated, a single positive Widal test is never considered to be diagnostic. Thus, a rising titre has to be seen, and each titre has to have been taken 2 weeks apart.7 As laboratories lack the qualified, experienced personnel and infrastructure needed to detect and serotype Salmonella isolates, clinicians in India rely primarily on the Widal test for the diagnosis of typhoid fever, which has been used without determining the locally appropriate threshold titre.
If the Widal test is positive, a course of FQs is usually given as monotherapy at primary centres. But in a time of increasing resistance to FQs, it is necessary to rule out TB before treating the patient as a case of typhoid fever. A positive Widal test leads to a delay in the diagnosis of TB, and FQs resistance in mycobacteria may develop in the short exposure to quinolone monotherapy.8 The Widal test has a sensitivity rate varying from 61.0–81.5%,9 18.3% for specificity, 10.1% for positive predictive value, and 89.7% for negative predictive value.10
Furthermore, a positive Widal test leads to the prescription of FQs, causing an increase in the emergence of FQ resistance in patients with TB. According to reports, 36% of MDR TB infections have extra FQ resistance in India.11,12 Here, the authors emphasise the need to rule out TB at primary health centres in patients with persistent fever and prevent the delay in diagnosis, which is one of the causes of increased morbidity and mortality in TB.
In a case report studied by Skoutelis et al.,13 very high titres of typhoid and paratyphoid agglutinins were obtained with the Widal test, and these titres returned to normal after successful anti-TB treatment. Both TB and typhoid fever are common in India. In a case series including 31 patients with TB and 29 patients without TB, the Widal test was found positive in 22.58% of TB cases and 37.50% in non-TB cases, indicating a very high rate of false-positives from the Widal test in both groups. A total of 22.58% of patients with TB had already received a course of quinolone monotherapy based on the positive test result.14
In one study, 11% of patients had Mycobacterium tuberculosis isolates, with a decreased susceptibility to FQs amongst those who received FQ therapy; however, no FQ-resistant M. tuberculosis isolates were recovered from patients who had not received previous FQ therapy.3
In the past, a true agglutination reaction from a case of typhoid fever, along with a false partial reaction in TB, has been pictured. The microscopic Widal test has been found to give positive results in many cases of TB with no history of typhoid fever. The TB fixation and microscopic Widal test corresponded in 62% of the cases. 15
The Widal test is no longer being used in developed countries due to its poor performance.16 Hence, its use and interpretation should be done cautiously and in accordance with the clinical context, which is an arduous job.6 Even in non-endemic countries, the diagnostic value of the Widal test is too low. Due to its limited value, it is recommended for use in patients who experience negative repeated cultures.17
In India, healthcare professionals can adopt a strategy that prevents delay in typhoid or TB, as both have dreaded complications. Therefore, the authors propose that, at the primary care centre, a patient presenting for persistent pyrexia should be evaluated with a limited number of investigations such as a chest X-ray, ultrasonography of the whole abdomen, the Widal test, and other routine tests, including a complete blood count and inflammatory markers. In light of clinical history and screening investigation positivity, healthcare professionals can then proceed further (i.e., if the chest X-ray shows lesions, a sputum for Ziehl–Neelsen stain can be completed and, in case of a positive result from the Widal test, blood cultures can be sent).
CONCLUSION
Throughout this feature, the authors point to a situation where the clinician feels justified in using quinolone monotherapy based on a positive Widal test in India. This can lead to resistance of mycobacteria to quinolones, and thus facilitate the emergence of MDR or extensively drug-resistant TB. Along with it, there is an emerging need to rule out TB at primary health centres in patients with persistent fever to prevent the delay in diagnosis, which is one of the causes of increased morbidity and mortality in TB. Although data related to this issue in the literature is scarce, more studies are required for understanding the pathophysiology of a positive Widal test in various other diseases and the exact duration of FQ therapy, which can cause resistance. Although more trials and research are needed, healthcare professionals should interpret the results of the Widal test cautiously, as misdiagnosis and improper patient management may come from incorrect interpretation of the test results, which may cause significant morbidity and mortality.