In Europe, there is a lack of detection of neurocognitive disorders (NCD) in primary care, particularly in nursing homes. Obstacles in nursing homes include general practitioners’ limited time, unawareness of diagnosis guidelines and tools, and difficulties to refer patients who are disabled to NCD specialist doctors. Telemedicine (TLM) could improve access to specialist doctors and increase NCD diagnosis.
In the context of the “Act On Dementia” European Joint Action, three countries (Bulgaria, France, and Greece) tested TLM for NCD detection and diagnosis in six nursing homes (one in Bulgaria, three in Greece, and two in France). NCD detection tools for patients were shared as well as satisfaction and dementia attitude questionnaires for nursing homes staffs. The experiments were planned from April 2018 to June 2018.
The six nursing homes were faced with various legal, ethical, and practical requirements before TLM could be implemented. Results at 3 months varied. In Greece, the nursing homes’ staffs were trained about NCD via a 30-hour tele-educational programme. In France, despite altered Mini-Mental State Examination (MMSE) scores and current TLM for behavioural disorders (behavioural and psychological symptoms of dementia [BPSD]), there were few requests for NCD diagnosis, probably a result of unawareness of diagnosis benefits for nursing homes’ residents. In Bulgaria, nursing homes’ staff training and 17 teleconsultations for NCD diagnosis took place and led to mild-to-major NCD diagnosis, including aetiological diagnosis in 16 cases. Despite the challenges, all the nursing homes‘ teams were satisfied with TLM. The dementia attitude scale results were similar between the different nursing homes, countries, and health professionals and other nursing homes’ professionals.
Each country identified facilitators to improve NCD diagnosis in nursing homes, e.g., a shared tool explaining the benefits of NCD aetiological diagnosis for nursing homes’ patients (Table 1) to be included in the NCD educational programme for nursing homes’ staff and general practitioners, which represents a crucial step for a successful TLM programme.The first request for TLM for NCD in nursing homes was for BPSD; NCD detection and diagnosis in nursing homes could be improved by TLM when combined with BPSD evaluation.
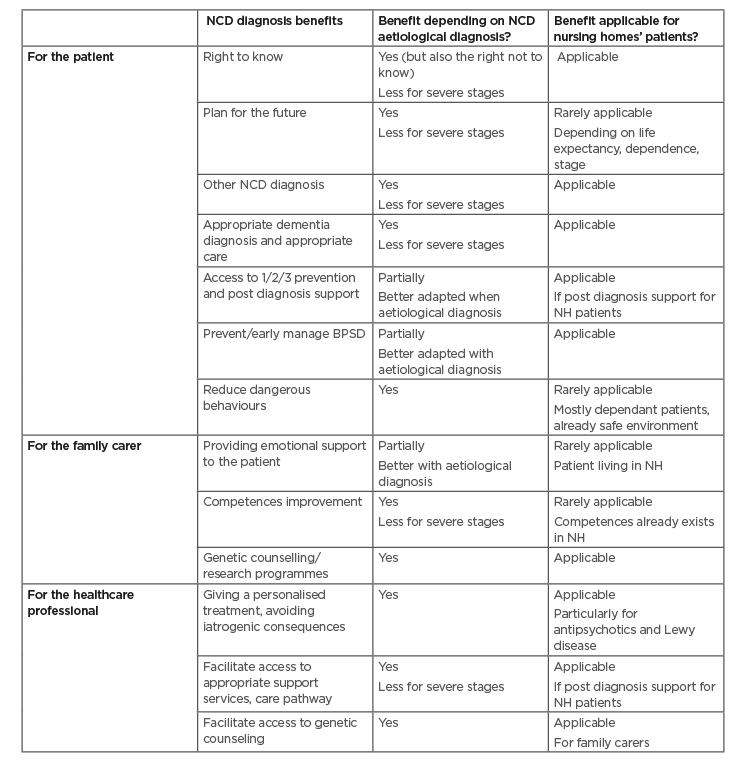
Table 1: Benefits of neurocognitive disorders aetiological diagnosis for nursing homes’ patients: a tool proposed by « ACT ON DEMENTIA » to support neurocognitive disorder diagnosis in nursing homes.2
BPSD: behavioural and psychological symptoms of dementia; NCD: neurocognitive disorder; NH: nursing home.