BACKGROUND AND AIMS
Ipsilateral external carotid artery (ECA) may supply the cerebral circulation through collateral vessels in patients with internal carotid artery (ICA) occlusion; at least 10–15% of the middle cerebral artery blood flow may be provided by ECA.1 Silent or symptomatic, permanent or transient, and retinal or cerebral ischaemic events could be triggered by emboli originating from the ICA or ECA or by a haemodynamic mechanism.2 Furthermore, it was observed that isolated ECA plaque was an independent predictor of all-cause mortality.3
As angiographic studies revealed that different cerebral regions depend on ipsilateral ECA contribution, different procedures for revascularisation have been tried during the last decades; some of them, such as surgical ICA and ECA bypass, did not show any benefit.4 There are numerous reports regarding endarterectomy for ECA stenosis alone or simultaneous to ICA revascularisation, but stenting has rarely been reported.
The aim of this paper is to present the case of a patient with ECA stenosis and ipsilateral ICA occlusion in whom stenting of the ECA was performed.
MATERIALS AND METHODS
A 73-year-old male was admitted for the first time to the author’s neurology department 3 years ago for angiographic examination of carotid and vertebral artery stenoses. The patient had medical history of a right frontal and insular ischaemic stroke, arterial hypertension, dyslipidaemia, peripheral artery disease, and mild neurocognitive impairment.
Neurologic examination revealed slight left central facial palsy and hemiparesis. Digital subtraction angiography of the cervical and cerebral arteries revealed the presence of a right ICA occlusion, 60% right ECA stenosis, 80% left ICA stenosis, and 90% left vertebral artery stenosis with intracerebral filling of right middle and anterior cerebral arteries from the left ICA. Left ICA stenting was performed due to an increased risk of stroke.
One year later, digital subtraction angiography of the cervical and cerebral arteries showed progression of right ECA stenosis under best medical treatment, with intracerebral filling of the right middle cerebral artery from the right ECA. Additionally, the cerebral CT depicted extension of the hypodensity located in the territory of the right middle cerebral artery and right anterior cerebral artery. As a result, ECA stenting was decided.
RESULTS
One year later, the ultrasonographic examination of the cervical arteries showed increased velocities and endothelial proliferation at the ECA stent site, confirmed by digital subtraction angiography of the cervical and cerebral arteries; balloon angioplasty was performed with optimal results. There was no evidence of worsening of the scores obtained at the neuropsychological examination follow-up.
CONCLUSION
This case highlights the importance of revascularisation therapy and follow-up in patients with stenoses of cervical arteries. This approach maintains the patency of these arteries and prevents further ischaemic events and vascular cognitive impairment. As these cases are not so frequent, it is important to gather evidence regarding the best approach and treatment strategy.
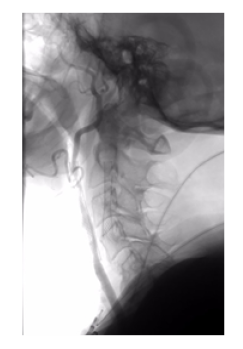
Figure 1: Digital sutraction angiography of the cervical and cerebral arteries showing intra-stent restenosis of the right external carotid artery. Left internal carotid artery stent can also be observed.








