BACKGROUND AND AIMS
The growing use of substances that affect the endocrine system (endocrine disruptors [ED]), together with evidence of their role in the development of Type 2 diabetes (T2D), has led to the hypothesis that EDs may contribute to the rising incidence of gestational diabetes (GD).1-4 The aim of the authors’ study was to describe exposure to selected EDs in women diagnosed with GD compared to a control group and to identify changes in the steroid spectrum in relation to ED exposure and GD.1
MATERIALS AND METHODS
Ninety-seven pregnant women were involved in the study (55 with diagnosed GD [fetuses: 30 male and 25 female] and 42 healthy controls [fetuses: 15 male and 27 female]). The authors collected maternal blood two times during pregnancy, at delivery, 3 days after delivery, and 6 months after delivery, and collected mixed fetal cord blood5 after delivery. In all samples, steroids (nine C21 steroids, nine androgens, three oestrogens, and their conjugates) and EDs (bisphenols A, S, F, P, AF, AP, methylparaben, ethylparaben, propylparaben, butylparaben, benzylparaben, and their conjugates) were analysed using liquid chromatography-tandem mass spectrometry.6,7 Data were statistically analysed using the Mann–Whitney test, with fetal sex considered.8
RESULTS
The differences between women with GD and controls were as follows: women carrying a male fetus had a lower level of conjugated ethylparaben and butylparaben, as well as lower conjugated androstenedione, conjugated progesterone, conjugated and free 5α-dihydroprogesterone, pregnenolone, 11-deoxycortisol, 11-deoxycorticosterone, and higher 11-ketotestosterone.1 Meanwhile, there were no differences in women carrying a female fetus.1 Important results were found in cord blood: the authors demonstrated the shift from bisphenol A to alternative bisphenols, compared to the authors’ previous study, where no alternative bisphenols were found in cord blood.9 In the cord blood of girls (those who were offspring of women with GD), there were higher levels of conjugated butylparaben and lower levels of dehydroepiandrosterone and oestradiol. In the cord blood of boys (those who were offspring of women with GD), there were higher levels of bisphenol A and bisphenol S1 (Figure 1).
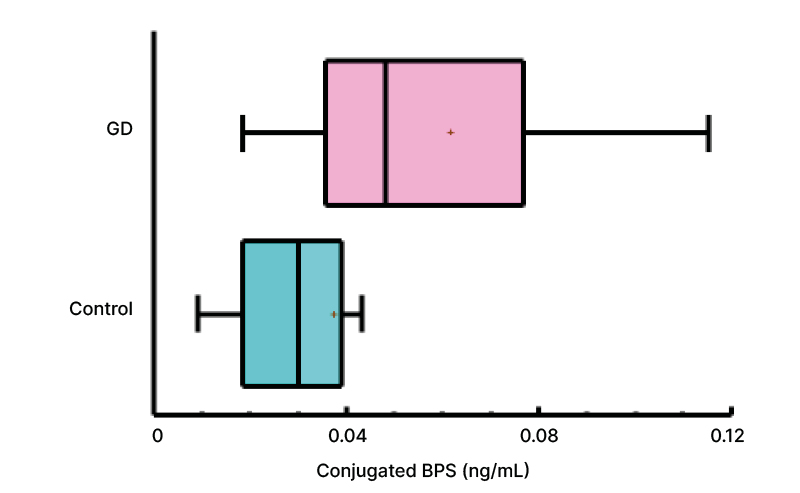
Figure 1: Conjugated bisphenol S levels in mixed umbilical blood (male fetus) detected in both newborn groups.
The red cross indicates the mean value. Significantly, there were higher levels of BPS in the group whose mothers had GD compared to the control group.
GD: gestational diabetes; BPS: bisphenol S.
CONCLUSION
The authors demonstrated the occurrence of ED not only in pregnant women, but also in their offspring, where a higher level was found in the offspring of women with GD. The authors also observed alterations in steroid levels in women with GD carrying a male fetus,1,9 some of which have been described in the literature in male patients with T2D.10







