Sperm DNA fragmentation (SDF) reduces fertilisation rate, embryo quality, and pregnancy rate,1 and ~30–50% of infertility cases are due to sperm defects.2 However, 20% of sperm abnormalities like SDF cannot be detected by light microscopy. Exposure to environmental pollutants, drugs, radiation, smoking, febrile illness, varicocele, advanced age, and obesity can increase SDF.3 Intracytoplasmic sperm injection (ICSI) allows injection of sperm directly into the egg to induce fertilisation and embryo development, thus enabling a man with an extremely low sperm count to have a biological child. The purpose of this study was to investigate lifestyle factors associated with increased SDF and their impact on ICSI outcome.
The SDF data from 94 men undergoing ICSI from January 2015–June 2016 were analysed. The study parameters were male age, BMI, smoking, standard semen parameters, and SDF. The semen samples were grouped into three categories based on percentage levels of SDF (Figure 1): <15%, 15–30%, and >30%. The SDF was determined by the Sperm Chromatin Dispersion Assay, using the Halosperm G2® kit (Halotech®, Madrid, Spain).
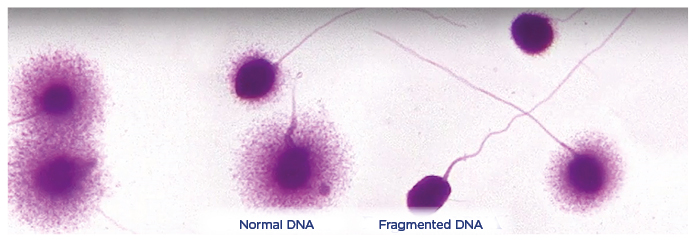
Figure 1: A sperm chromatin dispersion analysis showing sperm with unfragmented DNA with a ‘halo’ and sperm with fragmented DNA without a ‘halo’.
Source: Halotech®, Madrid, Spain.
The results of this study are shown in Table 1. Male BMI and smoking were positively correlated with SDF. Age was also positively correlated with the 15–29% and >30% SDF categories. However, sperm concentration and progressive motility were negatively correlated with SDF, as well as the sperm morphology, which was negatively correlated with the <15% and 15–30% SDF categories. There was no difference in pregnancy rates after ICSI in low and moderate SDF categories; however, in the high SDF category, no men achieved pregnancy (data not shown).
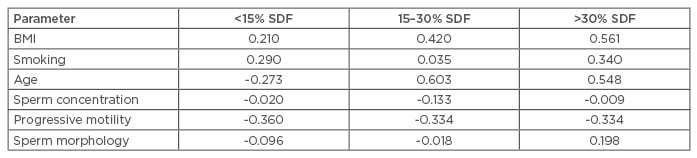
Table 1: The correlations of SDF with lifestyle factors and semen parameters.
SDF: sperm DNA fragmentation.
The SDF is one of the male fertility predictors.1 It is therefore vital for healthcare professionals to inform infertile male partners about the lifestyle factors that can result in high SDF and those that can have a negative impact on ICSI outcome.








