BACKGROUND AND AIMS
Imparting the required psychomotor skills for trainees to become proficient in percutaneous nephrolithotomy (PCNL) and retrograde intrarenal surgery (RIRS) is tricky for surgical educators due to the challenging nature of the procedures and the lack of realistic simulators. The current COVID-19 pandemic has compounded these issues by reducing learning opportunities for trainees through reduced case numbers and the availability of surgical skills courses. To address these contemporaneous issues, the authors have developed 3D printed inexpensive combined RIRS and PCNL training models for both in-person and video conference skills training.
MATERIALS AND METHODS
Anonymised CT data was used to develop the training model, using medical image processing software (3D Slicer version 4.12 [Surgical Planning Lab, Harvard Medical School, Harvard University, Boston, Massachusetts, USA]). The model was 3D printed using flesh-coloured resin, which best approximated the appearance of the collecting system during ureteroscopy. The face validity of the simulator was assessed by surgical educators for its suitability for both in-person and remote training.
RESULTS
The RIRS and PCNL training model was evaluated by expert urologists involved in the national training of the procedures and found to be more realistic and affordable when compared with available alternatives. The 3D printed model was developed for under 3 EUR, allowing multiple identical copies to be 3D printed for both in-person courses and scheduled video conferencing workshops, with the models distributed to each participating centre beforehand. This hub and spoke method of surgical skills training is greatly facilitated by the affordability of the 3D printed models.
CONCLUSION
The authors have developed an inexpensive combined RIRS and PCNL training model for both in-person and remote training at the Urological Society of Australia and New Zealand (USANZ) and other international training courses. 3D printed simulators have great future potential in the training of endourological and other urological procedures, enhancing connectivity and facilitating the decentralisation of training courses for the acquisition of key surgical skills.
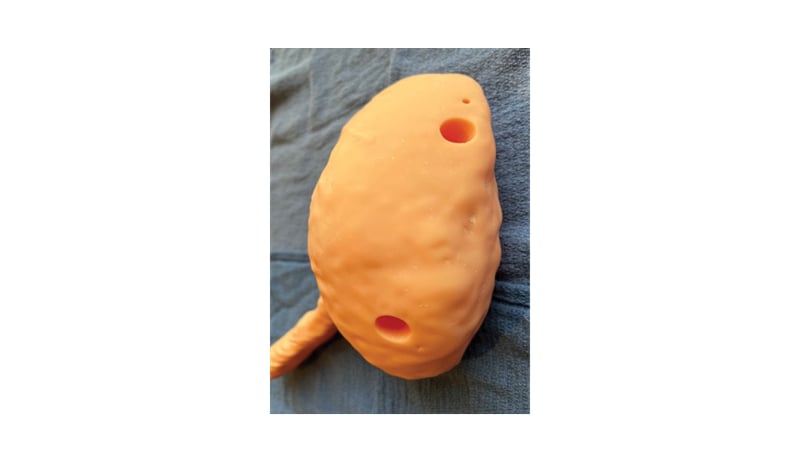
Figure 1: The 3D printed retrograde intrarenal surgery and percutaneous nephrolithotomy trainer.








