There has been increasing interest in the literature on the disease-specific psychological wellbeing of patients with cancer, and it has been estimated that less than half of all cancer subjects are properly identified and subsequently treated for anxiety or depression.1 It is now widely recognised that psychosocial care is a crucial part of high-quality cancer care centres.1 An elevated level of anxiety increases the risk associated with surgery (such as elevated heart rate, blood pressure, or the need for more medication to maintain an adequate level of sedation during procedure), including the morbidity and mortality.2 Unfortunately, significant psychological disorders usually remain undetected and underestimated until their impact on quality of life becomes more visible.3 This underestimation highlights the need to investigate different indicators of the psychosocial risk in oncology populations.4
The aim of the present study was to assess the prevalence of preoperative anxiety, depression, and psychological distress using validated self-administered questionnaires in patients with urological malignancies (prostate, bladder, and renal) undergoing radical surgery. We performed a cross-sectional study in consecutively enrolled patients with bladder, kidney, or prostate cancer, scheduled for surgery. Demographic data, socioeconomic status, education level, and diagnoses were recorded. Patients with a previous diagnosis of depression or anxiety were excluded.
We evaluated the level of clinically meaningful depression and anxiety with two assessment tools: The Hospital Anxiety and Depression Scale ([HADS]; a score ≥8 indicated the presence of anxiety and depression; a score ≥11 indicated clinical anxiety and depression) and the State-Trait Anxiety Inventory (STAI). In order to determine variables related to depression and anxiety among the demographic variables, logistic regression analyses were conducted with p<0.05 considered as statistically significant. Two hundred and twenty consecutive patients admitted for oncological disease had their psychological profile evaluated.
Two hundred and seven patients completed the questionnaires and were included in the final study. The patients presented a mean age of 70.8 (±10.8) years, 89% were male (n=184), and 19% of patients presented previous cancer. Patients more frequently underwent surgery for bladder tumours (60.4%) and the most common type of surgery was transurethral resection. The most frequent procedures were performed for bladder tumours (60.4%), with transurethral resection the most common type of surgery (52.7%) followed by radical prostatectomy (24.6%). The mean STAI-state score was 19.3 (±10.3), and the mean STAI-trait score was 18.4 (±11.9) points. Patients showed HADs depression and anxiety scores of 3.3 (±3) and 5.6 (±3.3) points, respectively. Female patients showed a higher level of anxiety and STAI-trait compared to males. See Table 1.
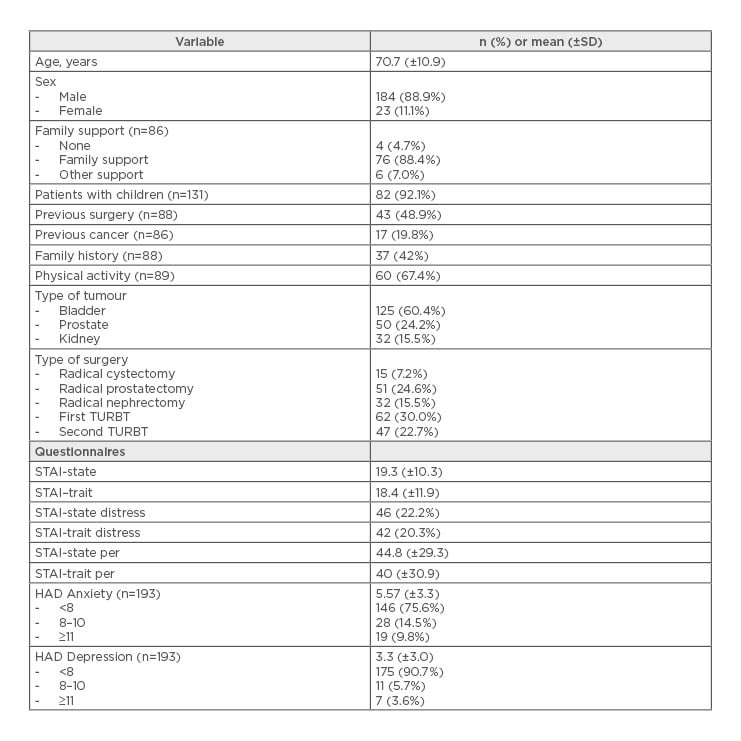
Table 1: Patient characteristics (N=207).
STAIT distress was defined according to the sex cut-off.
SD: standard deviation; TURBT: transurethral resection of bladder tumour; HADS: Hospital Anxiety
and Depression Scale; STAI: The State-Trait Anxiety Inventory.
The present results showed that our patients had lower levels of anxiety and depression than those described in the literature. Sex, tumour type, and surgical approach were significantly related to psychological distress in patients undergoing surgery for urological cancer. Females and patients with a kidney tumour and patients undergoing radical nephrectomy presented higher levels of anxiety. Patients with radical cystectomy showed a higher level of STAI-state compared with other surgeries.








