BACKGROUND
Hypertension and obesity in adults have been associated with increased P-wave dispersion (PwD). This is postulated due to the correlation of hypertension with diastolic dysfunction and atrial enlargement. In hypertension, left ventricular hypertrophy and diastolic dysfunction can cause an increase in atrial strain, fibrosis, and dilation. These changes result in inhomogeneous atrial conduction. Heterogeneity in atrial conduction can be seen as variation in P-wave duration between differently oriented surface electrocardiogram (ECG) leads. Interlead variation in P-wave duration is called PwD.
OBJECTIVE
The aim of the study was to measure PwD and its association with hypertension in the REDISCOVER Malaysia population.
METHODS
The REDISCOVER study is a longitudinal, community-based study that tracks lifestyle changes, risk factors, and chronic disease in urban and rural areas of Malaysia. This study was conducted between 2007 and 2014, and included consenting adults of >30 years of age. Participants were required to complete questionnaires on cardiovascular risk factors and medical history, and undergo physical examinations, blood tests, ECG, and echocardiography examinations. Demographic variables including weight, height, blood pressure, serum glucose, and serum lipid were recorded. Exclusion criteria included previous myocardial infarction, thyroid dysfunction, diabetes, valvular heart disease, cardiomyopathy, electrolyte imbalance, alcoholism, and medications that affect atrial conduction. Maximum and minimum P-wave durations were calculated from standard 12 lead ECG in sinus rhythm. A minimum of 9 out of 12 leads of P-wave duration were measured. PwD was then calculated by subtracting the minimum P-wave duration from the maximum P-wave duration in any of the 12 leads. PwD were calculated manually with hand-held callipers on paper by two cardiologists, independently. A total of 125 participants with hypertension were randomly selected and their PwD were compared to 125 randomly selected, age-matched healthy control subjects.
RESULTS
A total of 10,805 subjects participated in the REDISCOVER study. Mean age for the cohort was 52.6 (±11.6) years, and 56% were female. Of these subjects, 4.4% had a diagnosis of ischaemic heart disease, 1.3% had experienced a previous stroke, 16.7% had diabetes, and 45.6% had hypertension. The baseline characteristics of the hypertensive and normotensive groups are summarised in Table 1.
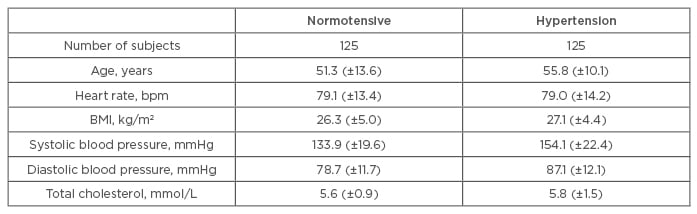
Table 1: Mean baseline characteristics of hypertension.
bpm: beats per minute.
The mean age for the hypertensive cohort was 55.8 years (±10.1) while the control group was 51.3 (±13.6). Mean blood pressure for the hypertensive cohort was 154/87 mmHg, compared to the control group with 134/79 mmHg. In the hypertensive cohort, maximum P-wave duration was significantly increased at 116.8±17.7 ms, compared to 103.2±22.0 ms in the control group (p<0.001). There was also a significant increase in minimum P-wave duration in hypertensive subjects at 53.7±11.8 ms, compared to control group with 48.6±15.7 ms (p=0.004). There was a significant increase in the PwD in the hypertensive group at 63.0±18.2 ms, compared to controls with 54.6±21.9 ms (p=0.001).
CONCLUSION
Both maximum P wave duration and PwD were significantly increased in our hypertensive cohort. Surface ECG markers could be a simple, non-invasive method of screening and predicting risk of hypertensive cardiomyopathy in prehypertensive and hypertensive patients.








