BACKGROUND AND AIMS
Lichen planus is a chronic inflammatory disorder characterized by cytotoxic T cell-mediated interface dermatitis targeting the dermoepidermal junction.¹ The disease demonstrates significant clinical heterogeneity, including cutaneous, mucosal, hypertrophic, and scarring variants such as lichen planopilaris, and remains challenging to manage due to frequent relapse and limited durability of conventional therapies. Systemic corticosteroids, retinoids, and immunosuppressive agents provide incomplete disease control and are associated with substantial adverse effects.¹
Emerging evidence implicates cytokine-driven inflammation mediated through the JAK-STAT pathway as a central driver of disease activity. Interferon γ and other proinflammatory cytokines promote keratinocyte injury and sustained immune activation through this signaling cascade.² Targeting upstream immune signaling, therefore, represents a rational therapeutic approach.
MATERIALS AND METHODS
This case series evaluates the clinical response to upadacitinib, a selective JAK1 inhibitor, in six patients with refractory lichen planus across multiple subtypes. All patients had failed prior therapies, including topical and systemic corticosteroids, cyclosporine, and other immunosuppressive agents. The cohort included patients with oral lichen planus, hypertrophic disease, annular variants, and scarring alopecia consistent with lichen planopilaris (Table 1).¹
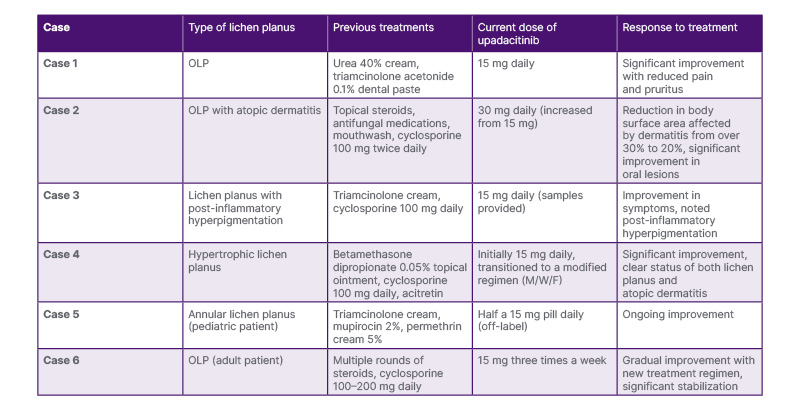
Table 1: Case presentation summary of patients with lichen planus.
M/W/F: Monday/Wednesday/Friday; OLP: oral lichen planus
RESULTS
Treatment with upadacitinib resulted in consistent clinical improvement across all patients and disease subtypes. Patients with oral involvement demonstrated a reduction in pain and pruritus with improvement in mucosal lesions. Cutaneous variants showed decreased erythema, scale, and plaque thickness, with several cases achieving near-complete clearance or marked stabilization. Improvement was observed across a range of dosing strategies, including standard daily dosing and modified regimens, suggesting flexibility in real-world use.¹
The observed responses support the role of JAK-STAT signaling as a key pathogenic mechanism in lichen planus. By inhibiting JAK1, upadacitinib reduces cytokine-mediated T cell activation and keratinocyte injury, thereby interrupting the self-perpetuating inflammatory loop characteristic of this disease.²
These findings highlight the potential of targeted immunomodulation in patients with refractory lichen planus who have failed conventional therapies. The consistent response across diverse clinical phenotypes, including mucosal and scarring disease, suggests the broad applicability of
this approach.
CONCLUSION
In conclusion, upadacitinib demonstrates promising efficacy in the treatment of refractory lichen planus across multiple variants. Further studies with larger cohorts and longer follow-up are needed to establish long-term safety and durability of response and to define its role in treatment algorithms.¹







