BACKGROUND AND AIMS
Melanoma remains the deadliest form of skin cancer, accounting for a disproportionate share of skin cancer-related mortality despite relatively low incidence.1,2 Early detection is critical, with 5-year survival rates exceeding 99% in localized disease compared to approximately 27% in advanced-stage melanoma.2 However, persistent disparities exist, particularly among rural populations and individuals with skin of color, who experience higher mortality due to reduced access to dermatologic care, lower health literacy, and underrepresentation in skin cancer education initiatives.2,3
This prospective interventional study evaluates the impact of a brief, video-based educational intervention on melanoma knowledge, lesion recognition, and self-skin examination (SSE) behaviors in an underserved population.
MATERIALS AND METHODS
The study was conducted at a regional cancer center in Albany, Georgia, USA, and included 201 adult participants recruited from clinic waiting areas and survivorship programs. Participants completed surveys at baseline, immediately following the intervention, and at 3-month follow-up (Table 1). The intervention consisted of a 5-minute, visually driven educational video written at a fifth-grade reading level, covering melanoma risk factors, ABCDE detection criteria (asymmetry, border irregularities, color variation, diameter >6 mm, and evolution), sun protection strategies, and SSE techniques.¹
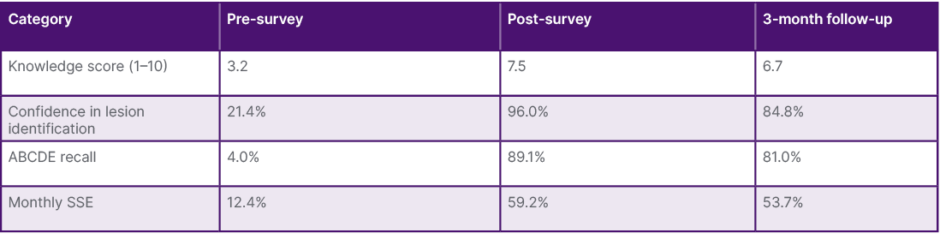
Table 1: Participant outcomes from pre-survey to post-survey and 3-month follow-up.
Knowledge scores (1–10) improved from 3.2 at baseline to 7.5 post-survey, with partial retention at 6.7 at follow-up. Confidence in lesion identification increased from 21.4% to 96.0% post-survey, remaining high at 84.8% after 3 months. ABCDE recall rose from 4.0% to 89.1% and was sustained at 81.0% at follow-up. Monthly self-skin exam practice improved from 12.4% to 59.2% post-survey, with continued adherence of 53.7% at 3 months.
ABCDE: Asymmetry, border irregularities, color variation, diameter >6 mm, and evolution; SSE: self-skin examination.
RESULTS
The intervention produced significant improvements across all primary outcomes, including melanoma knowledge scores, confidence in lesion identification, ABCDE recall, and frequency of SSE. Knowledge scores increased from a baseline mean of 3.2 to 7.5 post-intervention and remained elevated at 6.7 at 3 months. Confidence in lesion identification improved from 21.4% at baseline to 96% immediately post-intervention, with sustained improvement at 84.8% at follow-up. Similarly, ABCDE recall increased from 4% to 89.1%, and monthly SSE frequency improved from 12.4% to 59.2%, with retention at 53.7% at 3 months.¹
Importantly, subgroup analysis demonstrated that participants with lower baseline awareness, disproportionately represented by underserved and minority populations, experienced the greatest improvements. Racial disparities in melanoma knowledge and SSE practices narrowed following the intervention, highlighting its potential to address inequities in dermatologic education and early detection.1
These findings emphasize the effectiveness of brief, accessible educational tools in overcoming structural barriers to care. In settings where access to dermatology is limited, empowering patients with practical knowledge and self-examination skills may facilitate earlier detection and reduce reliance on specialty services.3 The low cost, scalability, and minimal resource requirements of this intervention make it particularly well suited for implementation in primary care settings, oncology clinics, and underserved communities.
CONCLUSION
In conclusion, a short, literacy-conscious video intervention delivered at the point of care can produce significant and sustained improvements in melanoma awareness and preventive behaviors while reducing racial disparities in knowledge and screening practices. This scalable, patient-centered approach represents a practical strategy to improve early melanoma detection and advance equity in cancer outcomes.¹







